Pathophysiology - Gut Garden Gone Wild
- A breakdown in host defenses allows excessive bacterial proliferation (esp. anaerobes, coliforms) in the small bowel, an area that should normally have a low bacterial count.
- Primary Mechanisms:
- ↓ Gastric Acid: Achlorhydria, often from chronic PPI use.
- ↓ Intestinal Motility: Impaired peristaltic "housekeeping" waves (e.g., diabetes, scleroderma, opioids).
- Anatomic Stasis: Surgical blind loops, strictures, or fistulas that create stagnant areas.
⭐ Chronic use of Proton Pump Inhibitors (PPIs) is a major iatrogenic risk factor by suppressing the natural gastric acid barrier against bacterial colonization.
Presentation & Risks - The Usual Suspects
- Clinical Picture: Chronic, non-specific GI symptoms.
- Bloating, excessive flatulence, abdominal pain/cramping.
- Watery diarrhea; may have steatorrhea (foul-smelling, floating stools).
- Unintentional weight loss & signs of malabsorption.
- Key Risk Factors:
- ↓ Motility: Diabetic gastroparesis, scleroderma, intestinal pseudo-obstruction.
- Anatomic: Surgical blind loops (Roux-en-Y), strictures (Crohn's), fistulae, small intestinal diverticula.
- ↓ Acid: Chronic PPI therapy.
- Immune: IgA deficiency, CVID.
⭐ SIBO paradox: Bacteria consume Vitamin B12 leading to deficiency (megaloblastic anemia, neuropathy), but produce folate and Vitamin K, so levels may be normal or high.
Diagnosis - Breath & Beyond
- Gold Standard: Endoscopy with jejunal aspirate culture showing > 10³ CFU/mL (some use 10⁵ CFU/mL). Invasive, rarely the first step.
- Non-Invasive Testing (Preferred): Carbohydrate breath tests.
- Glucose Breath Test (GBT): Detects proximal SIBO. Easier to interpret.
- Lactulose Breath Test (LBT): Can detect more distal SIBO, but higher false-positive rate due to normal colonic fermentation.
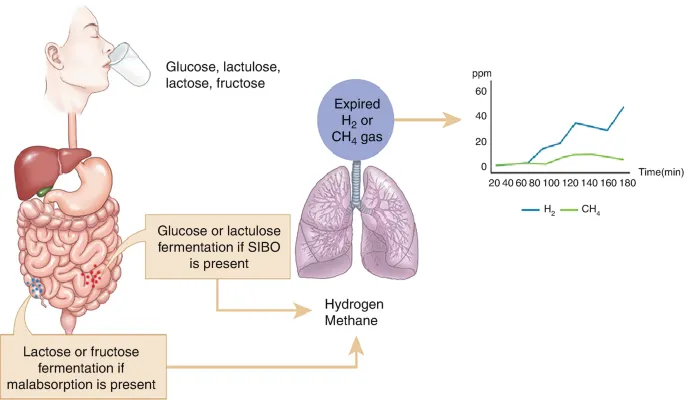
⭐ False Positives: A rapid small bowel transit time can cause the lactulose substrate to reach the colon prematurely, leading to a false-positive result that mimics SIBO.
Management - Weeding the Overgrowth
Primary goal: Eradicate bacteria, manage underlying causes, and correct nutritional deficits.
- Antibiotic Therapy (“Weeding”):
- Rifaximin: First-line agent. Dose: 550 mg TID for 14 days. Non-absorbable, acts locally.
- Alternatives: For methane-predominant SIBO or rifaximin failure.
- Neomycin (often with Rifaximin).
- Metronidazole.
- Address Root Cause:
- Treat motility disorders (e.g., gastroparesis).
- Correct anatomical issues (e.g., surgical strictures).
- Review medications (e.g., PPIs, opioids).
- Nutritional Support:
- Supplement Vitamin B12, fat-soluble vitamins (A, D, E), and iron.
- Low FODMAP diet for symptom control.
⭐ Recurrence is common. If symptoms return, consider cyclic antibiotic therapy or using prokinetics (e.g., low-dose erythromycin) to stimulate gut motility and prevent relapse.
High‑Yield Points - ⚡ Biggest Takeaways
- SIBO results from excessive bacteria in the small bowel, typically due to stasis from impaired motility (e.g., diabetes, scleroderma) or anatomic alterations.
- Key symptoms include bloating, flatulence, watery diarrhea, and abdominal pain; severe cases cause malabsorption and steatorrhea.
- Gold standard for diagnosis is a jejunal aspirate culture showing >10^5 CFU/mL, but carbohydrate breath tests (glucose, lactulose) are more common.
- Strongly associated with long-term PPI use, diabetes, and Roux-en-Y gastric bypass.
- Treatment is primarily with antibiotics like rifaximin or neomycin.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

