Insulin - The Sugar Shuttle
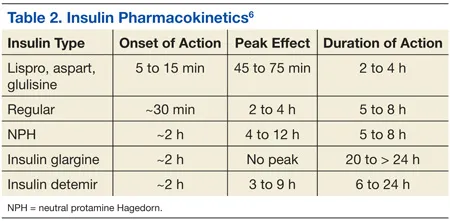
- Insulin Analogs & Action Profiles: Essential for mimicking physiologic insulin secretion. Basal-bolus regimens combine long-acting with rapid/short-acting insulin.
| Type | Examples | Onset | Peak | Duration |
|---|---|---|---|---|
| Rapid | Lispro, Aspart, Glulisine | ~15 min | 1-2 hr | 4-6 hr |
| Short | Regular (Humulin R) | ~30 min | 2-4 hr | 6-8 hr |
| Intermediate | NPH (Humulin N) | 2-4 hr | 4-8 hr | 10-18 hr |
| Long | Glargine, Detemir, Degludec | 1-2 hr | Flat/Peakless | >24 hr |
⭐ High-Yield: Regular insulin is the only type suitable for IV administration, crucial in diabetic ketoacidosis (DKA). Long-acting insulins like Glargine form microprecipitates, providing slow, sustained release.
Oral Agents Pt 1 - The First Responders
| Agent | MOA | AEs | Key Facts |
|---|---|---|---|
| Metformin | ↓ Hepatic gluconeogenesis, ↑ peripheral glucose uptake. | GI upset, lactic acidosis (rare), B12 deficiency. | First-line therapy. Weight neutral/loss. Hold if eGFR < 30. |
| Sulfonylureas (e.g., Glipizide) | Close K-ATP channels → ↑ insulin secretion. | Hypoglycemia, weight gain. | 📌 "-ide"s glide insulin out. High hypoglycemia risk. |
| Meglitinides (e.g., Repaglinide) | Close K-ATP channels (shorter duration). | Hypoglycemia (less risk), weight gain. | Postprandial glucose control. Take with meals. |
Oral Agents Pt 2 - The New Wave
| Agent Class | Mechanism of Action (MOA) | Adverse Effects (AEs) | Key Benefits |
|---|---|---|---|
| TZDs (-glitazone) | Upregulate PPAR-γ → ↑ insulin sensitivity and glucose uptake in muscle, adipose tissue. | Weight gain, edema, fluid retention (⚠️ contraindicated in HF), ↑ bone fracture risk. | No hypoglycemia, durable glycemic control. |
| DPP-4i (-gliptin) | Inhibit DPP-4 enzyme → prolongs endogenous GLP-1 action → glucose-dependent ↑ insulin & ↓ glucagon. | Pancreatitis, disabling arthralgia. | Weight neutral, generally well-tolerated, low hypoglycemia risk. |
| SGLT-2i (-gliflozin) | Inhibit Sodium-Glucose Co-Transporter 2 (SGLT-2) in the PCT, blocking glucose reabsorption. | Genitourinary infections (UTIs, vulvovaginal candidiasis), euglycemic DKA, hypotension. | Weight loss, blood pressure reduction, significant cardiovascular & renal benefits. |
⭐ SGLT-2 inhibitors are now a cornerstone therapy for T2DM patients with established heart failure or CKD, as they significantly reduce hospitalizations and mortality.
Injectables & Algorithms - Beyond The Pill
- GLP-1 Receptor Agonists (-tide): Liraglutide, Semaglutide, Dulaglutide.
- Benefits: ↓Weight, ↓Major Adverse CV Events (MACE), low hypoglycemia risk.
- Use: Often 2nd line after metformin, especially with established ASCVD.
- ⚠️ BBW: Medullary thyroid cancer (rodents).
- Amylin Analogue: Pramlintide.
- Adjunct to mealtime insulin (T1DM & T2DM).
- ↓Postprandial glucose, promotes satiety.
- Insulin Therapy:
- Basal: Glargine, Detemir, Degludec. Controls fasting glucose.
- Prandial (Bolus): Lispro, Aspart, Glulisine. Covers mealtime excursions.
⭐ In T2DM with established ASCVD, Heart Failure, or CKD, specific GLP-1 RAs or SGLT2i have compelling benefits independent of HbA1c.
High‑Yield Points - ⚡ Biggest Takeaways
- Metformin is first-line for T2DM; its biggest risk is lactic acidosis, especially with renal insufficiency.
- SGLT-2 inhibitors (-gliflozins) offer significant cardioprotective and renal benefits but risk euglycemic DKA.
- GLP-1 agonists (-tides) promote weight loss and reduce cardiovascular events; pancreatitis is a key risk.
- Sulfonylureas and meglitinides carry the highest risk of hypoglycemia among oral agents.
- TZDs (-glitazones) increase insulin sensitivity but can cause fluid retention and worsen heart failure.
- Basal-bolus insulin (glargine/detemir + lispro/aspart) is the most physiologic replacement strategy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

