Starling Forces - The Great Exchange
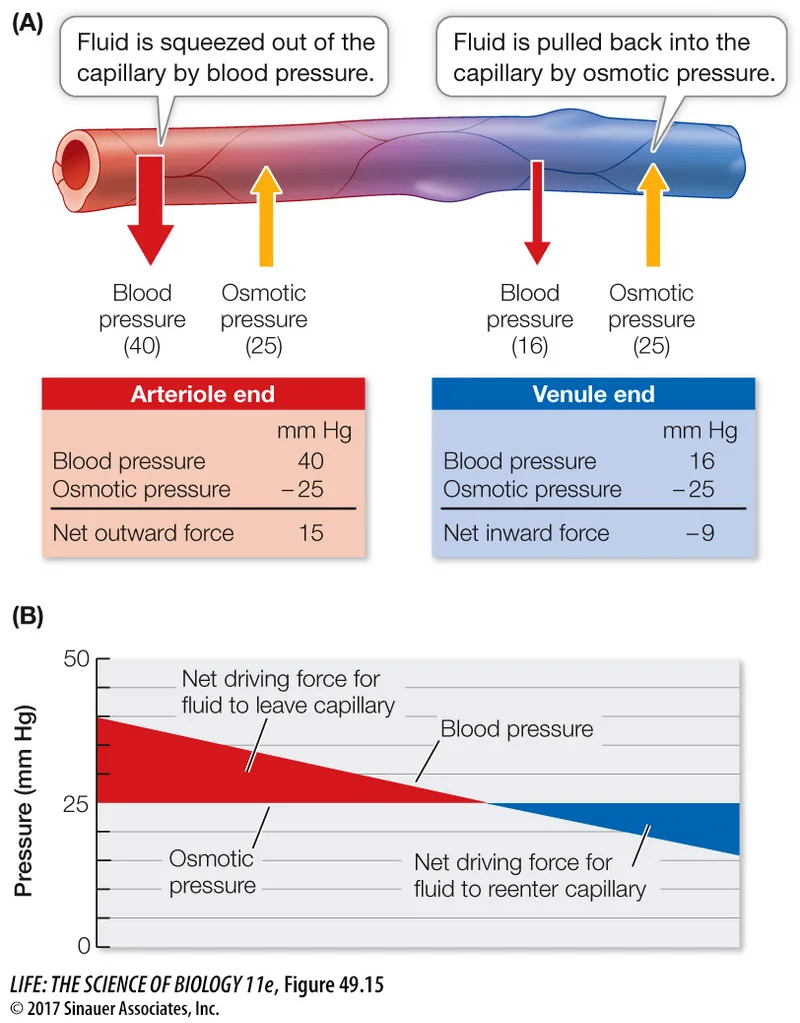
- Fluid movement across capillaries is governed by Starling forces, balancing hydrostatic (push) and oncotic (pull) pressures. Net movement determines filtration or absorption.
- Net Filtration Pressure Equation: $J_v = K_f [ (P_c - P_i) - \sigma (\pi_c - \pi_i) ]$
- $P_c$ (Capillary hydrostatic): Pushes fluid out.
- $\pi_c$ (Capillary oncotic): Pulls fluid in.
- $P_i$ (Interstitial hydrostatic): Pushes fluid in.
- $\pi_i$ (Interstitial oncotic): Pulls fluid out.
- 📌 Mnemonic: 'Push out, Pull in'. P for Hydrostatic Pressure Pushes; π for Oncotic Pressure Pulls.
⭐ The reflection coefficient (σ) indicates the effectiveness of the capillary wall in preventing protein passage. A value of 1 implies impermeability, while 0 implies free passage.
| Capillary Type | Structure & Permeability | Key Locations |
|---|---|---|
| Continuous | Least permeable; tight junctions. | Muscle, skin, lungs, CNS. |
| Fenestrated | Moderate permeability; pores. | Kidneys (glomeruli), endocrine glands. |
| Sinusoidal | Most permeable; large gaps. | Liver, spleen, bone marrow. |
Flow Regulation - Local Traffic Control
Autoregulation is the intrinsic ability of an organ to maintain constant blood flow despite changes in perfusion pressure. Key mechanisms:
- Myogenic Mechanism: Smooth muscle contracts in response to ↑ stretch (↑ pressure) and relaxes with ↓ stretch.
- Metabolic Mechanism: Tissue metabolism dictates local blood flow.
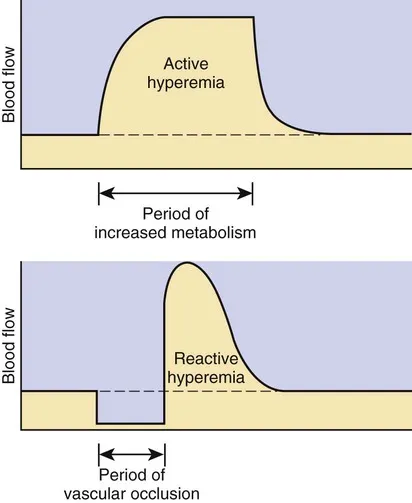
Hyperemia:
- Active Hyperemia: Blood flow increases to meet metabolic demand (e.g., exercise).
- Reactive Hyperemia: A transient increase in blood flow following a period of ischemia.
Local Vaso-regulators:
- Vasodilators:
- Nitric Oxide (NO)
- Adenosine
- $K^+$
- $CO_2$
- $H^+$
- Vasoconstrictors:
- Endothelin
- Myogenic response
⭐ In the heart, adenosine is the most critical local vasodilator linking coronary blood flow to myocardial oxygen demand.
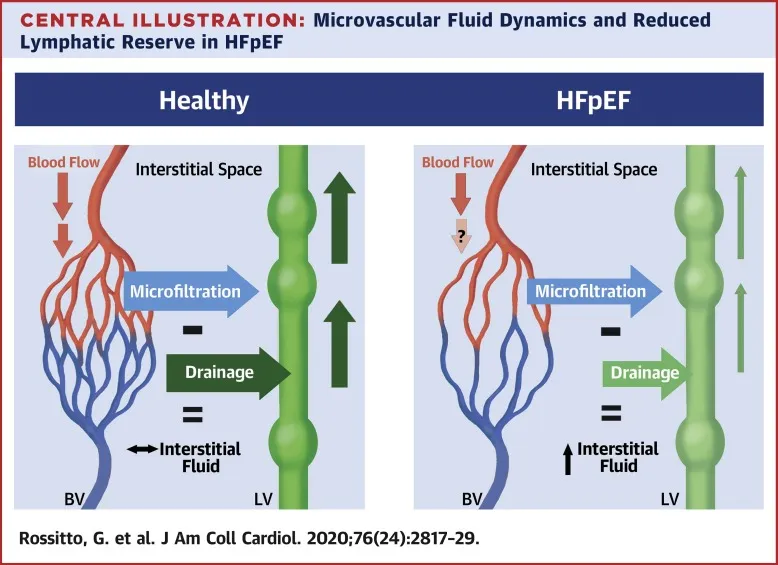
Lymphatics & Edema - The Drainage System
Lymphatic capillaries drain excess interstitial fluid, protein, and macromolecules, returning it to circulation. Failure of this system results in edema-fluid accumulation in the interstitium.
-
Pathophysiology (Altered Starling Forces):
- ↑ $P_c$ (Capillary Hydrostatic Pressure): Pushes excess fluid out (e.g., heart failure, DVT).
- ↓ $\pi_c$ (Plasma Oncotic Pressure): Fails to pull fluid in (e.g., liver failure, nephrotic syndrome).
- ↑ $K_f$ (Capillary Permeability): Allows protein and fluid to leak out (e.g., inflammation, burns).
- Lymphatic Obstruction: Impairs fluid return (e.g., post-surgery, filariasis).
-
Types: Pitting edema (low-protein fluid) vs. Non-pitting edema (protein-rich fluid).
⭐ Lymphedema, caused by lymphatic obstruction (e.g., post-mastectomy, filariasis), is a classic cause of non-pitting edema due to the high protein content of the interstitial fluid.
- Starling forces (hydrostatic & oncotic pressures) dictate fluid flux across the capillary wall.
- Capillary hydrostatic pressure (Pc) is the main force driving filtration (fluid out).
- Plasma oncotic pressure (πc) is the main force driving reabsorption (fluid in).
- Arterioles are the primary site of vascular resistance, regulating blood flow into the capillary bed.
- Lymphatics are essential for draining excess interstitial fluid, preventing edema.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

