A-a Gradient - The Great Divide
- Measures the difference between alveolar ($PAO_2$) and arterial ($PaO_2$) oxygen tension, localizing the cause of hypoxemia.
- Calculated as: $PAO_2 - PaO_2$.
- Normal value is age-dependent, roughly $(Age/4) + 4$. A value > 15 mmHg is generally considered elevated.
- Normal Gradient: Indicates an extra-pulmonary cause.
- Hypoventilation (e.g., CNS depression)
- Low inspired $FiO_2$ (e.g., high altitude)
- Elevated Gradient: Suggests an intrinsic lung problem.
- V/Q Mismatch
- Shunt
- Diffusion Limitation (e.g., fibrosis)
⭐ A key differentiator: hypoxemia from V/Q mismatch corrects with 100% O2, while hypoxemia from a true shunt does not.
Hypoxemia Causes - A Tale of Two Gradients
- The Alveolar-arterial (A-a) gradient differentiates causes of hypoxemia by comparing alveolar oxygen ($PAO_2$) to arterial oxygen ($PaO_2$).
- Calculated as: $A-a,gradient = PAO_2 - PaO_2$.
- A normal A-a gradient is < 15 mmHg; it increases with age (approx. Age/4 + 4).
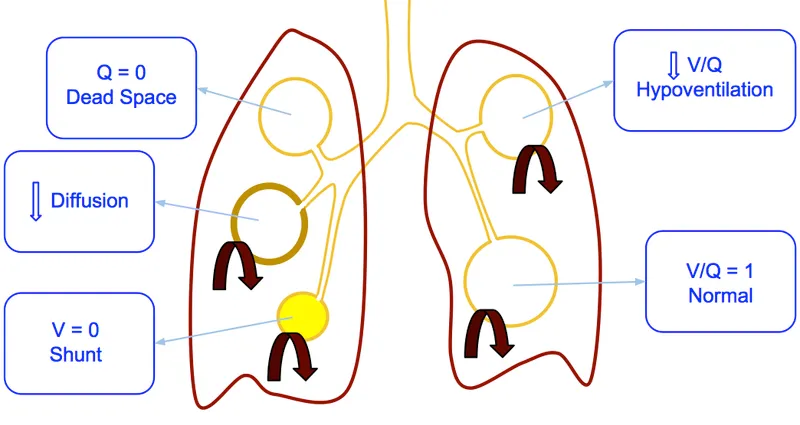
⭐ Hypoxemia from V/Q mismatch typically corrects with supplemental O₂, whereas hypoxemia from a true shunt does not significantly improve, as shunted blood bypasses ventilated alveoli entirely.
- Normal Gradient: Lungs are functional; problem is inadequate O₂ delivery to the alveoli.
- Elevated Gradient: Lungs are dysfunctional; problem is impaired O₂ transfer from alveoli to blood.
Correcting Hypoxemia - Oxygen to the Rescue?
- The response to supplemental O₂ helps differentiate causes of hypoxemia.
- Normal A-a Gradient Hypoxemia:
- Caused by hypoventilation or low inspired O₂ (FiO₂).
- Readily corrects with 100% O₂ because the alveolar-capillary interface is intact.
- Elevated A-a Gradient Hypoxemia:
- V/Q Mismatch & Diffusion Limitation: Both improve and correct with 100% O₂. Supplemental oxygen overcomes the diffusion or perfusion limitations by increasing the partial pressure of oxygen in the alveoli.
- Shunt (Right-to-Left): Shows minimal or no correction with 100% O₂.
⭐ In a true shunt, deoxygenated blood bypasses ventilated alveoli entirely. Since it never gets exposed to the high FiO₂, the resulting arterial hypoxemia is refractory to oxygen therapy. This is a classic exam clue for intracardiac or large intrapulmonary shunts.
High‑Yield Points - ⚡ Biggest Takeaways
- The A-a gradient measures the difference between alveolar (PAO2) and arterial (PaO2) oxygen levels, reflecting gas exchange efficiency.
- A normal A-a gradient (5-15 mmHg) with hypoxemia suggests hypoventilation or low inspired O2.
- An elevated A-a gradient indicates a primary lung problem, such as V/Q mismatch, shunt, or diffusion limitation.
- Key causes of a high A-a gradient include pulmonary embolism, pneumonia, ARDS, and pulmonary fibrosis.
- The gradient naturally increases with age.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

