ANS Pharmacology - The Players & The Field
- Cholinergic Receptors (ACh):
- Nicotinic ($N_N, N_M$): Autonomic ganglia, adrenal medulla, neuromuscular junction.
- Muscarinic ($M_1, M_2, M_3$): Glands, smooth muscle, heart.
- Adrenergic Receptors (NE, Epi):
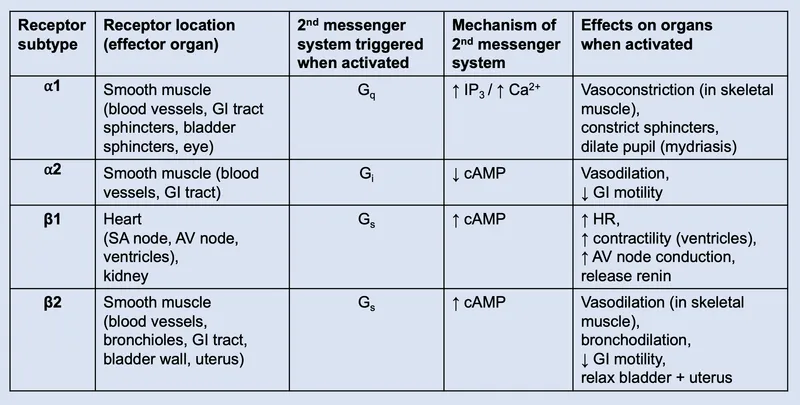
- Alpha ($\.alpha_1, \.alpha_2$): Vascular smooth muscle (vasoconstriction), presynaptic terminals.
- Beta ($\.beta_1, \.beta_2$): Heart (↑ rate/contractility), Lungs (bronchodilation).
⭐ At low doses, dopamine stimulates D1 receptors (renal vasodilation); at medium doses, B1 receptors (↑ cardiac contractility); at high doses, a1 receptors (vasoconstriction).
📌 G-Protein Coupling: "QISS and QIQ" for ($\.alpha_1, \.alpha_2, \.beta_1, \.beta_2$) and ($M_1, M_2, M_3$).
Adrenergic Interactions - The Reversal Heist
- Epinephrine Reversal: A paradoxical fall in Mean Arterial Pressure (MAP) when epinephrine is given after a non-selective α-blocker (e.g., phentolamine, phenoxybenzamine).
- Mechanism:
- Normally, epinephrine stimulates α1 (vasoconstriction) and β2 (vasodilation). The α1 effect dominates, causing ↑ MAP.
- After an α-blocker, the α1 vasoconstriction is blocked. Epinephrine's β2-mediated vasodilation becomes unopposed, causing ↓ Total Peripheral Resistance (TPR) and a fall in MAP.
- 📌 Mnemonic: Alpha-blockade before epi makes the pressure dip!
⭐ This reversal is unique to mixed α/β agonists. The pressor effect of a pure α-agonist like phenylephrine is simply abolished, not reversed. Norepinephrine's effect is blunted but not reversed due to its weak β2 activity.
Cholinergic Interactions - The SLUDGE-fest
-
Additive Toxicity (Cholinergic Crisis): Occurs when multiple cholinergic agents are combined.
- Examples: Cholinomimetics (pilocarpine, bethanechol) + AChE inhibitors (neostigmine, physostigmine).
- Leads to a "SLUDGE-fest" of muscarinic overstimulation.
- 📌 SLUDGE: Salivation, Lacrimation, Urination, Defecation, GI distress, Emesis.
-
Antagonism: Cholinergic effects can be blocked by antimuscarinic agents.
- Atropine: A competitive inhibitor at muscarinic receptors; reverses CNS and peripheral muscarinic effects of organophosphate poisoning.
- Pralidoxime: Regenerates AChE, reversing both muscarinic and nicotinic effects of organophosphates.
⭐ In organophosphate poisoning, atropine treats the muscarinic "SLUDGE" symptoms but does not reverse the nicotinic effect of muscle paralysis. Pralidoxime is required for this.
Systemic Effects - The Cardio Crossover
-
Baroreceptor Reflex: A key homeostatic loop. Drug effects can be direct (on vessels/heart) or indirect (reflex-mediated).
- An ↑ in BP triggers a reflex ↓ in HR.
- A ↓ in BP triggers a reflex ↑ in HR.
-
Clinical Interaction Example:
- Phenylephrine (pure α₁-agonist) → potent vasoconstriction → ↑ BP.
- The body compensates via the baroreceptor reflex → ↑ vagal tone → ↓ HR (reflex bradycardia).
⭐ Pre-treatment with atropine (a muscarinic antagonist) blocks the M₂ receptors on the heart, thus preventing the reflex bradycardia caused by agents like phenylephrine.
High‑Yield Points - ⚡ Biggest Takeaways
- Beta-blockers can blunt the therapeutic effects of beta-agonists (e.g., albuterol), which is dangerous in asthmatics.
- Alpha-blockers (e.g., phentolamine) can cause epinephrine reversal, a paradoxical hypotension from unopposed β2-mediated vasodilation.
- MAOIs with tyramine-rich foods (wine, cheese) can precipitate a hypertensive crisis.
- TCAs and cocaine block norepinephrine reuptake, potentiating direct-acting sympathomimetics.
- Cholinesterase inhibitors reverse non-depolarizing neuromuscular blockade but potentiate succinylcholine.
- Atropine reverses the muscarinic effects of cholinesterase inhibitor toxicity.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

