Mechanism of Action - The Pump Stopper
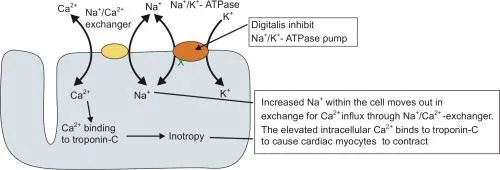
- Primary Action: Directly inhibits the $Na^+/K^+$-ATPase pump in cardiac myocytes.
- Ionic Shift: This inhibition leads to ↑ intracellular $Na^+$ concentration.
- Calcium Effect: The high intracellular $Na^+$ reduces the activity of the $Na^+/Ca^{2+}$ exchanger (NCX), which normally pumps $Ca^{2+}$ out.
- Result: ↑ intracellular $Ca^{2+}$ which is stored in the sarcoplasmic reticulum, leading to increased contractility (positive inotropy).
⭐ Exam Favorite: Hypokalemia potentiates digoxin's effects, as digoxin and $K^+$ compete for the same binding site on the $Na^+/K^+$-ATPase. Low potassium = less competition = more digoxin binding and potential toxicity.
Clinical Uses - Heart's Helping Hand
-
Systolic Heart Failure (HFrEF):
- Increases contractility (positive inotropy) to alleviate symptoms.
- Considered second-line therapy for patients remaining symptomatic on standard guideline-directed medical therapy.
- ⚠️ Does not improve mortality; used for symptomatic control only.
-
Atrial Fibrillation & Atrial Flutter:
- Slows the ventricular rate (negative chronotropy).
- Mechanism: ↑ parasympathetic (vagal) tone, which decreases conduction velocity through the AV node.
⭐ Digoxin is uniquely beneficial in patients with concurrent atrial fibrillation and systolic heart failure, as it addresses both rate control and contractility with a single agent.
Toxicity & Management - When Good Goes Bad
- Triggers: ↓K⁺, ↓Mg²⁺, ↓renal function, drugs (e.g., amiodarone, verapamil, quinidine).
- Clinical Features:
- GI: Nausea, vomiting, abdominal pain (often first signs).
- CNS: Confusion, weakness, fatigue.
- Visual: Xanthopsia (yellow-green halos), blurred vision, scotomas.
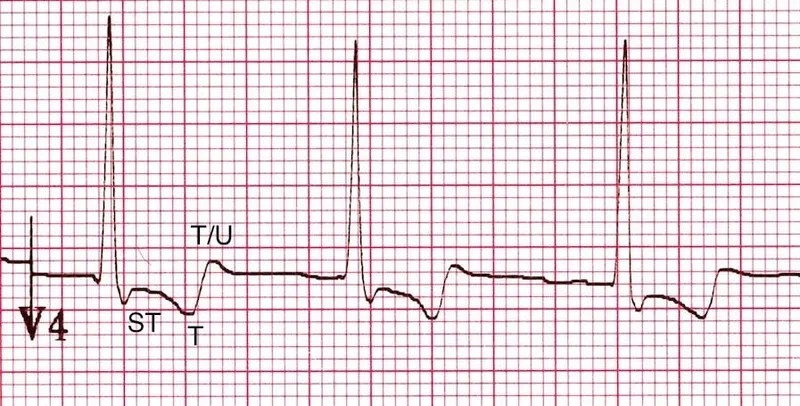
- EKG Findings:
- Most common arrhythmia: PVCs.
- Most specific: Atrial tachycardia with AV block.
- Bradycardia, heart blocks, hyperkalemia (in acute overdose).
⭐ Hypokalemia is a key precipitant. Low potassium potentiates digoxin's effect by increasing its binding to the Na⁺/K⁺-ATPase pump.
Pharmacokinetics - The Body's Tour
- Absorption:
- Oral bioavailability: ~75% (tablets).
- P-glycoprotein substrate: Inhibitors (e.g., verapamil, amiodarone, quinidine) ↑ digoxin levels.
- Gut flora (Eubacterium lentum) can inactivate it; antibiotics may ↑ absorption.
- Distribution:
- Large volume of distribution (Vd: 4-7 L/kg); concentrates in tissues (heart, skeletal muscle).
- Long half-life (t½): ~40 hours, often requiring a loading dose.
- Metabolism & Excretion:
- Primarily cleared by the kidneys as unchanged drug.
- ⚠️ Dose reduction is critical in renal dysfunction.
⭐ Due to its very large volume of distribution and extensive tissue binding, digoxin is not effectively removed by hemodialysis in cases of toxicity.
- Mechanism: Directly inhibits the Na+/K+ ATPase pump, leading to increased intracellular Na+, which then decreases Ca2+ efflux, ultimately increasing intracellular calcium and contractility.
- Clinical Use: Primarily for heart failure (positive inotropy) and atrial fibrillation (AV node conduction slowing).
- Toxicity: Very narrow therapeutic index. Toxicity is classically precipitated by hypokalemia.
- ECG Changes: Characteristic ST segment scooping (“Salvador Dalí mustache” sign); toxicity can cause AV block.
- Antidote: Digoxin immune Fab (Digibind) is used for life-threatening toxicity.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

