Angina Pectoris - Chest's Cry for Help
Myocardial ischemia from an oxygen supply/demand mismatch.
- Stable Angina: Due to fixed coronary stenosis (>70%). Predictable, exertional chest pain relieved by rest or nitroglycerin.
- Unstable Angina: Plaque rupture with a non-occlusive thrombus. New, worsening, or rest pain. High risk for MI.
- Prinzmetal's (Variant) Angina: Focal coronary artery vasospasm. Transient, occurs at rest, often at night.
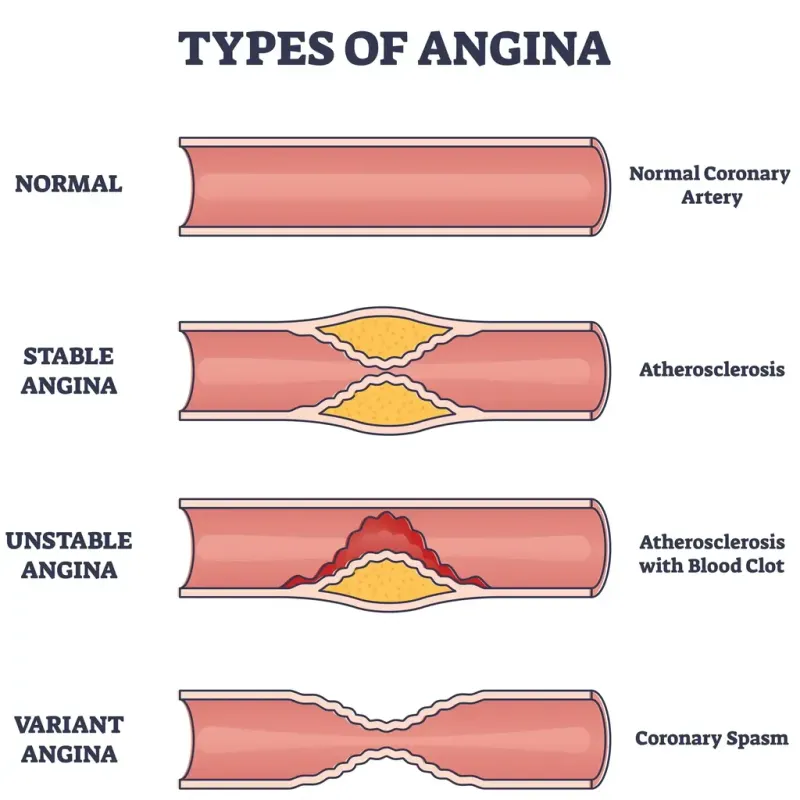
⭐ Prinzmetal's angina is associated with transient ST-segment elevation on ECG, unlike stable or unstable angina which typically show ST-segment depression.
Nitrates - Vessels on Vacation
- Drugs: Nitroglycerin, Isosorbide Dinitrate, Isosorbide Mononitrate.
- Mechanism: Primarily venodilators. They release nitric oxide, causing $NO \rightarrow \uparrow cGMP \rightarrow Venodilation$, which leads to a ↓ in preload (left ventricular end-diastolic pressure).
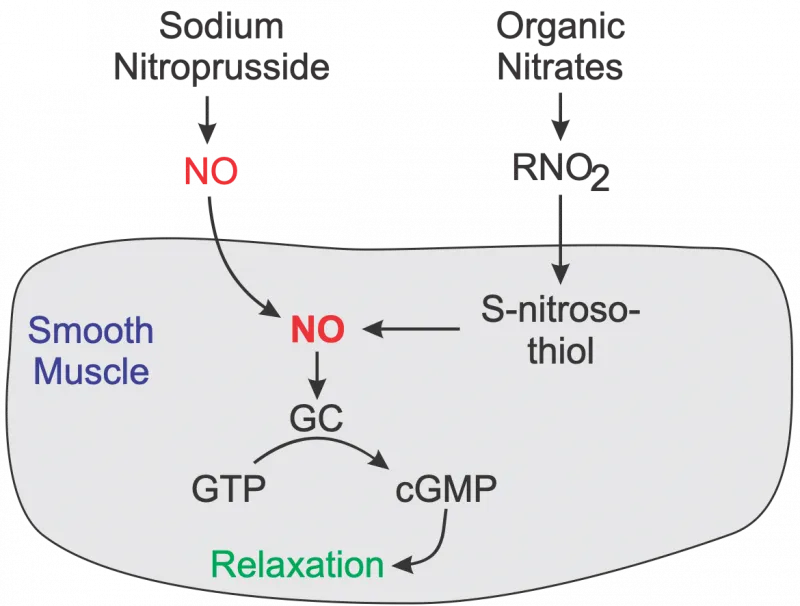
- Adverse Effects: Reflex tachycardia, hypotension, flushing, and headaches.
- 📌 Tachyphylaxis: Tolerance develops rapidly. A daily "nitrate-free" interval (8-10 hours, typically overnight) is required to restore sensitivity.
⭐ Workers in dynamite factories (exposed to nitrates) would develop tolerance. After a weekend off, re-exposure caused tachycardia, dizziness, and headache, known as "Monday disease."
Beta-Blockers - Heart's Chill Pill
-
Mechanism: Act as negative chronotropes and inotropes → ↓ heart rate & ↓ contractility. This reduces cardiac workload and overall myocardial oxygen demand ($↓ MVO_2$).
-
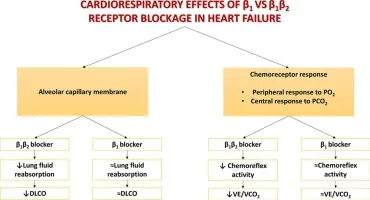
Types & Selectivity:
- Cardioselective (β1): Metoprolol, Atenolol, Bisoprolol. Preferred in patients with pulmonary issues.
- Non-selective (β1 + β2): Propranolol. Use with caution in asthma/COPD due to bronchoconstriction risk.
⭐ Beta-blockers are proven to reduce mortality post-myocardial infarction.
📌 Mnemonic: "BAM" for β1-selective blockers: Bisoprolol, Atenolol, Metoprolol.
Calcium Channel Blockers - Calcium's Gate Crashers
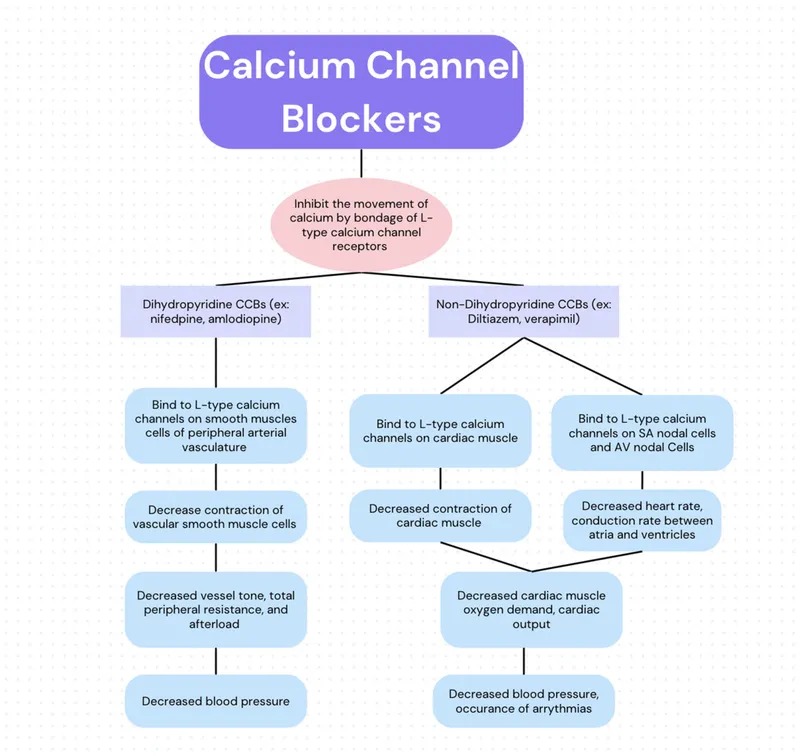
- Mechanism: Block L-type Ca²⁺ channels → ↓ intracellular Ca²⁺ → coronary vasodilation & ↓ systemic vascular resistance (afterload).
| Class | Agents | Primary Site | Clinical Effect |
|---|---|---|---|
| Dihydropyridines | Amlodipine, Nifedipine | Vascular Smooth Muscle | Potent Vasodilation (↓ Afterload) |
| Non-dihydropyridines | Verapamil, Diltiazem | Myocardium | ↓ Contractility & Heart Rate |
⭐ Exam Favorite: Can cause gingival hyperplasia (esp. Nifedipine, Verapamil) and peripheral edema (esp. Dihydropyridines).
Newer Agents - The Modern Arsenal
- Ranolazine: Inhibits the late $I_{Na}$ current, reducing intracellular Ca²⁺ overload and diastolic wall tension. Has minimal effect on heart rate or blood pressure.
- Ivabradine: Selectively inhibits the $I_f$ (“funny”) current in the SA node, slowing the heart rate without affecting contractility or blood pressure.
⭐ Ranolazine can prolong the QT interval.
High‑Yield Points - ⚡ Biggest Takeaways
- Nitrates cause potent venodilation, reducing preload. They are key for acute angina relief but require a nitrate-free interval to prevent tachyphylaxis.
- Beta-blockers are first-line for chronic stable angina, decreasing myocardial O2 demand by lowering heart rate and contractility.
- Calcium channel blockers are the treatment of choice for vasospastic (Prinzmetal) angina.
- Ranolazine treats refractory angina by inhibiting the late sodium current, but carries a risk of QT prolongation.
- Avoid combining non-dihydropyridine CCBs with beta-blockers due to the additive risk of severe bradycardia and AV block.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

