Shock Fundamentals - Little Bodies, Big Problems
- Physiology: Children have ↑ physiological reserve; they compensate via tachycardia & vasoconstriction.
- Hypotension is a LATE sign → indicates decompensated shock.
- Early signs: Tachycardia, poor perfusion (cool extremities, delayed capillary refill >2s), altered mental status.
- Pediatric Hypotension (SBP <5th percentile):
- Neonates (<1 mo): <60 mmHg
- Infants (1-12 mo): <70 mmHg
- Children (1-10 yrs): <70 + (2 × age in years) mmHg
⭐ The most common type of shock in children is hypovolemic shock, typically from dehydration (diarrhea/vomiting).
Types of Shock - The Four Horsemen
- Hypovolemic: Loss of fluid volume. Most common in children (diarrhea/vomiting).
- Cardiogenic: Pump failure. Myocarditis, congenital heart disease.
- Distributive: Vasodilation leads to maldistribution of blood flow. Sepsis, anaphylaxis.
- Obstructive: Physical obstruction to blood flow. Cardiac tamponade, tension pneumothorax, massive pulmonary embolism.
| Type | CVP/PCWP | CO | SVR | Skin |
|---|---|---|---|---|
| Hypovolemic | ↓ | ↓ | ↑ | Cold, Clammy |
| Cardiogenic | ↑ | ↓ | ↑ | Cold, Clammy |
| Distributive | ↓ | ↑ | ↓ | Warm (early) |
| Obstructive | ↑ | ↓ | ↑ | Cold, Clammy |
Clinical Recognition - Spotting the Signs
- Tachycardia: Earliest, most common sign. Heart rate ↑ to maintain cardiac output.
- Altered Mental Status: Key indicator of cerebral perfusion. Progression: Irritability → Anxiety → Lethargy → Coma.
- Skin Perfusion:
- Capillary Refill Time (CRT): > 2 seconds (prolonged).
- Temperature: Cool, clammy extremities.
- Color: Pale, mottled, or ashen skin.
- Pulses: Weak or absent peripheral pulses with bounding central pulses (early). Becomes thready everywhere as shock progresses.
- Urine Output: Decreased; < 1 mL/kg/hr is a sign of significant renal hypoperfusion.

⭐ Hypotension is a LATE and pre-terminal sign of shock in children. Their robust compensatory mechanisms can maintain blood pressure until they are critically ill. Never wait for hypotension to diagnose shock.
Initial Management - The Golden Hour Blitz
- A (Airway): Secure patent airway; intubate if GCS < 8 or respiratory failure.
- B (Breathing): Administer high-flow 100% O₂ via non-rebreather mask. Target SpO₂ > 94%.
- C (Circulation):
- Secure IV/IO access immediately.
- Give 20 mL/kg isotonic crystalloid (NS/RL) bolus over 5-10 mins.
- Reassess. May repeat up to 40-60 mL/kg.
- If unresponsive to fluids, start inotropes (e.g., Dopamine/Adrenaline).
- D (Disability): Check blood glucose (correct if < 60 mg/dL), pupils, and AVPU/GCS.
- E (Exposure): Undress to find rashes, trauma; prevent hypothermia.
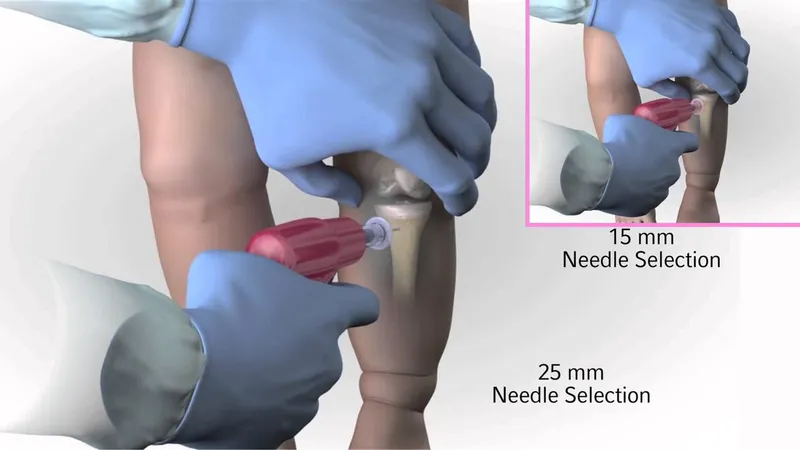
⭐ High-Yield: If IV access is not obtained within 90 seconds or after 3 attempts in a child in shock, establish intraosseous (IO) access without delay.
High‑Yield Points - ⚡ Biggest Takeaways
- Tachycardia is the earliest and most reliable sign of shock in children; hypotension is a late, ominous finding indicating decompensated shock.
- Initial management for most shock types is a 20 mL/kg bolus of isotonic crystalloid (Normal Saline or Ringer's Lactate).
- In septic shock, administer broad-spectrum antibiotics within the first hour.
- For cardiogenic shock, use cautious fluid boluses and start inotropes (like dobutamine) early.
- Anaphylactic shock requires immediate intramuscular epinephrine.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

