GBS Microbiology - The Beta-Hemolytic Baddie
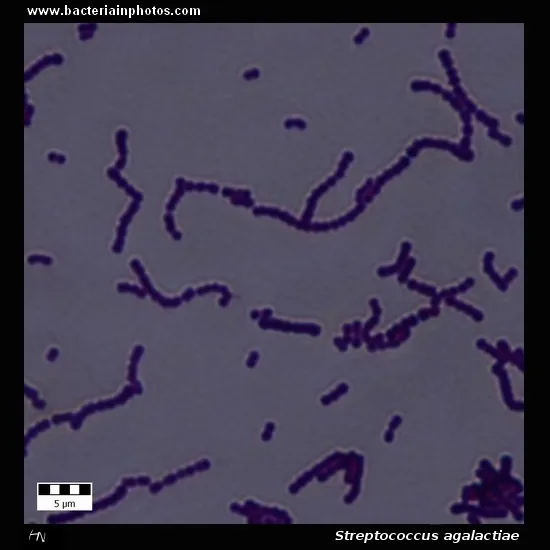
- Organism: Streptococcus agalactiae, a Gram-positive coccus forming chains.
- Culture: Exhibits a narrow zone of β-hemolysis on blood agar.
- Key Biochemical Markers:
- Catalase-negative.
- Bacitracin-resistant (differentiates from S. pyogenes).
⭐ CAMP Test Positive: GBS produces a diffusible CAMP factor that synergistically enhances the hemolysis of Staphylococcus aureus, creating a characteristic arrowhead-shaped clearing on blood agar. This is a hallmark identification test.
Transmission & Risks - The Perilous Passage
- Primary Source: Maternal rectovaginal colonization.
- Transmission: Primarily vertical, occurring either in-utero (ascending infection) or during delivery.
- Risk Factors for Early-Onset Disease (EOD):
- GBS bacteriuria at any point during the current pregnancy.
- Preterm delivery (< 37 weeks).
- Prolonged rupture of membranes (PROM) ≥ 18 hours.
- Intrapartum fever ≥ 38°C (100.4°F).
⭐ A previous infant with invasive GBS disease is the most significant risk factor, mandating automatic intrapartum antibiotic prophylaxis (IAP) in subsequent pregnancies.
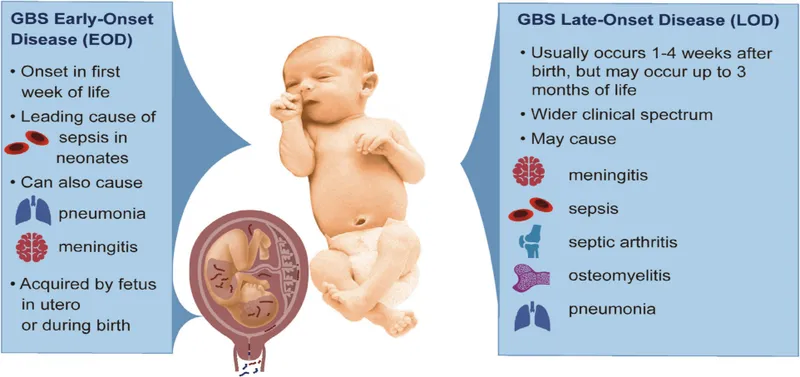
Clinical Syndromes - Early vs. Late Onset
| Feature | Early-Onset Disease (EOD) | Late-Onset Disease (LOD) |
|---|---|---|
| Onset | <7 days of life (typically <24-48h) | 7 days to 3 months |
| Source | Maternal genital tract (vertical) | Maternal or nosocomial/community (horizontal) |
| Presentation | Sepsis, pneumonia, respiratory distress | Bacteremia without a focus, meningitis |
⭐ Exam Favourite: Late-onset disease (LOD) is strongly associated with meningitis (~30% of cases), often presenting with subtle signs like poor feeding, irritability, or fever.
Prevention & Treatment - The Prophylaxis Plan
- Diagnosis: Gold standard is blood culture. For suspected meningitis, perform CSF analysis.
- Treatment: High-dose IV Penicillin G or Ampicillin is the first-line therapy.
⭐ Universal screening via rectovaginal swab is performed between 36+0 and 37+6 weeks of gestation to guide prophylaxis.
High‑Yield Points - ⚡ Biggest Takeaways
- Most common cause of neonatal sepsis and meningitis in term infants.
- Early-onset disease (EOD) at <7 days is acquired vertically and typically presents with respiratory distress/pneumonia.
- Late-onset disease (LOD) at 7-90 days is acquired horizontally and often presents as bacteremia or meningitis.
- Universal maternal screening via rectovaginal culture at 35-37 weeks gestation is key.
- Intrapartum antibiotic prophylaxis (IAP) with IV Penicillin G is the cornerstone of prevention for colonized mothers.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

