Acute Pancreatitis - Fiery Digestive Fury
- Etiology: 📌 I GET SMASHED (Idiopathic, Gallstones, Ethanol, Trauma, Steroids, Mumps, Autoimmune, Scorpion sting, Hypercalcemia/Hypertriglyceridemia, ERCP, Drugs).
- Pathophysiology: Premature activation of trypsinogen to trypsin within the pancreas, leading to autodigestion.
- Diagnosis: Requires 2 of 3 criteria:
- Acute epigastric pain radiating to the back.
- ↑ Serum amylase or lipase (>3x ULN).
- Characteristic findings on imaging.
⭐ Hypocalcemia is a poor prognostic sign, resulting from saponification of peripancreatic fat by activated lipases.
- Complications: Pseudocyst, abscess, necrosis, ARDS, renal failure.
Chronic Pancreatitis - Scars & Stones
- Pathophysiology: Irreversible inflammation leads to fibrosis and calcified stones, causing progressive loss of exocrine (digestion) and endocrine (insulin) function.
- Etiology: Alcohol abuse (most common, adults); Cystic fibrosis (children). Also autoimmune, hereditary, or idiopathic.
- Clinical Features: Persistent epigastric pain radiating to the back, malabsorption (steatorrhea, weight loss), and late-onset diabetes mellitus.
- Diagnosis: CT scan is best for detecting calcifications & ductal dilation ("chain of lakes" appearance). ↓ fecal elastase confirms exocrine insufficiency.
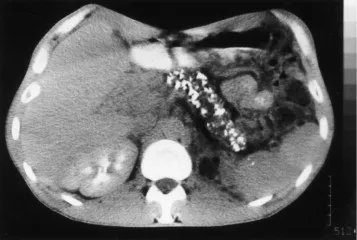
⭐ Amylase and lipase are often normal due to burnout of acinar cells, unlike in acute pancreatitis.
Pancreatic Neoplasms - Silent Tumors
-
Pancreatic Ductal Adenocarcinoma (PDAC): Most common, aggressive malignancy.
- Presentation: Late; often unresectable.
- Head (~75%): Painless obstructive jaundice, weight loss, steatorrhea.
- Body/Tail: Abdominal pain radiating to the back, weight loss.
- Risk Factors: Smoking (strongest), chronic pancreatitis, diabetes, age > 50, family history (BRCA2).
- Tumor Marker: ↑ CA 19-9.
- Genetics: KRAS (most common), p53, SMAD4.
- Presentation: Late; often unresectable.
-
Pancreatic Neuroendocrine Tumors (PanNETs): Functional or non-functional.
- Insulinoma: Hypoglycemia (Whipple's triad).
- Gastrinoma: Zollinger-Ellison syndrome (refractory peptic ulcers).
- Glucagonoma: Necrolytic migratory erythema, diabetes, DVT.
- VIPoma: Watery diarrhea, hypokalemia, achlorhydria (WDHA syndrome).
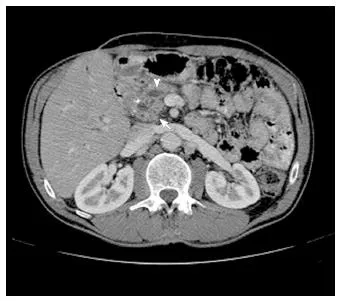
⭐ Courvoisier's Sign: A palpable, non-tender gallbladder in a jaundiced patient suggests malignant obstruction (e.g., pancreatic cancer), not gallstones.
High‑Yield Points - ⚡ Biggest Takeaways
- Acute pancreatitis is most commonly caused by gallstones and alcohol; diagnosis relies on elevated serum lipase.
- Chronic pancreatitis, mainly from alcoholism, leads to pancreatic calcifications, steatorrhea, and diabetes mellitus.
- Pancreatic adenocarcinoma typically presents as painless jaundice if in the pancreatic head; CA 19-9 is the tumor marker.
- Courvoisier sign-a palpable, non-tender gallbladder-suggests malignant obstruction.
- Pancreatic pseudocysts are a hallmark complication of acute pancreatitis, lacking a true epithelial lining.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

