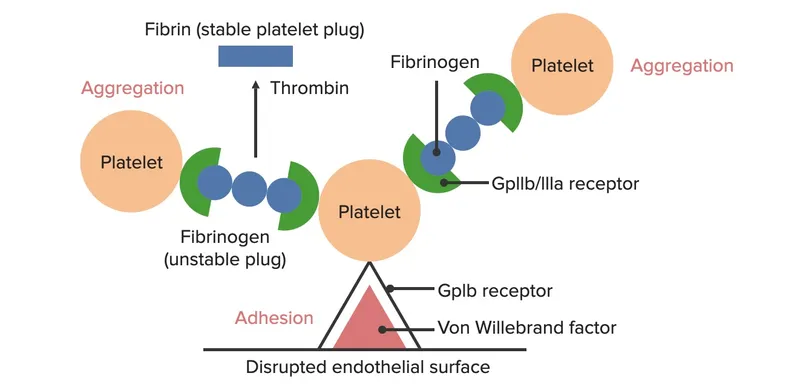
Primary Hemostasis - The First Responders
- Goal: Form a weak platelet plug at sites of vascular injury.
- Involves platelets, von Willebrand factor (vWF), and vessel wall.
- Clinical signs: Mucocutaneous bleeding (petechiae, epistaxis).
- Labs: Prolonged bleeding time.
⭐ Glanzmann thrombasthenia: Autosomal recessive defect in GpIIb/IIIa. Leads to impaired aggregation. Patients present with a normal platelet count but significant bleeding.
Thrombocytopenia - The Platelet Plummet
- Definition: Platelet count < 150,000/μL.
- Etiology Overview:
- ↓ Production: Marrow failure (aplastic anemia), infiltration (leukemia), drugs (chemo), infection (HIV).
- ↑ Destruction: Immune (ITP, TTP, HIT) or non-immune (DIC, hypersplenism).
- Clinical Signs: Petechiae, purpura, ecchymoses. Spontaneous bleeding risk ↑ if < 20,000/μL.
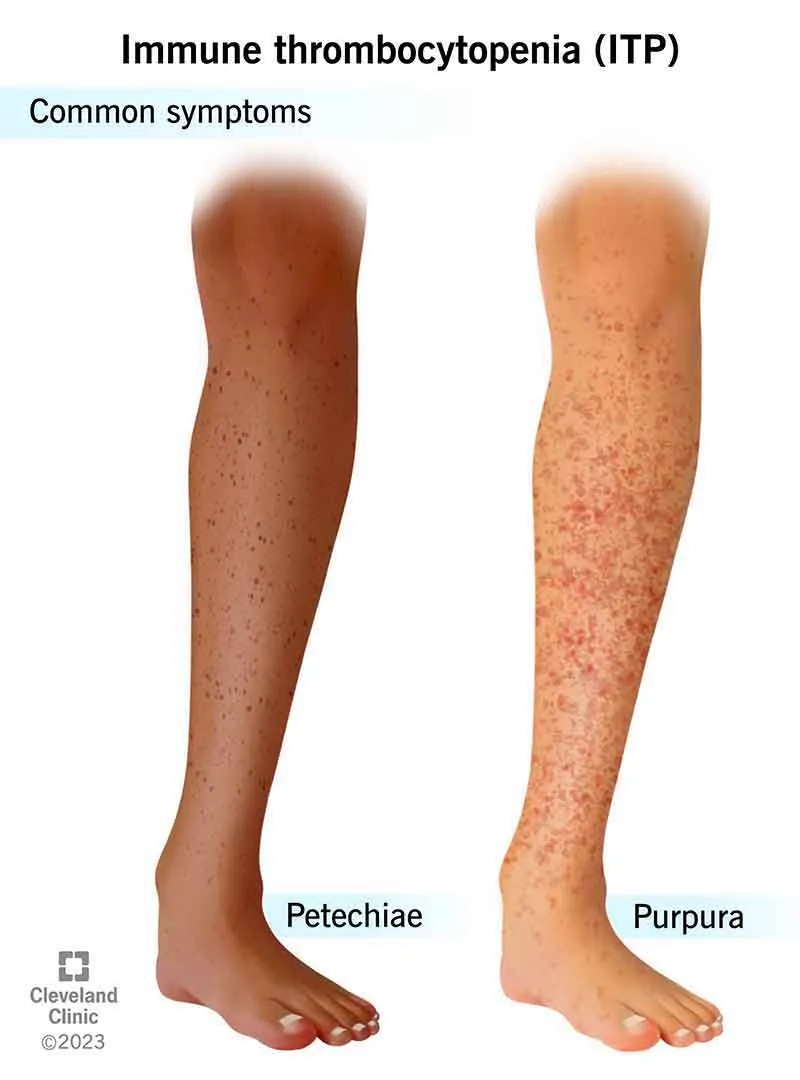
⭐ Immune Thrombocytopenic Purpura (ITP): An acquired autoimmune disorder with isolated thrombocytopenia. Often triggered by a recent viral infection in children. Antibodies target platelet glycoproteins like GpIIb/IIIa.
Qualitative Disorders - A Dysfunctional Crew
- Presentation: Normal platelet count, but ↑ Bleeding Time.
- Bernard-Soulier Syndrome:
- Big Suckers: giant platelets (mild thrombocytopenia is common).
- Defect in GpIb receptor → impaired adhesion to von Willebrand factor (vWF).
- Glanzmann Thrombasthenia:
- Defect in GpIIb/IIIa receptor → impaired aggregation.
- No platelet clumping in response to ADP, epinephrine, or collagen.
- Acquired Causes:
- Aspirin: Irreversibly inhibits COX, leading to ↓ Thromboxane A₂ (TXA₂) synthesis.
- Uremia: Impairs both adhesion and aggregation functions.
⭐ The Ristocetin cofactor assay helps differentiate these disorders. Platelet aggregation is abnormal in Bernard-Soulier syndrome (as ristocetin requires vWF-GpIb interaction) but is normal in Glanzmann thrombasthenia.
Thrombocytosis - Overcrowded Traffic
- Definition: Platelet count > 450,000/μL.
- Reactive Thrombocytosis (More Common):
- Caused by an underlying condition driving cytokine release (e.g., IL-6).
- Etiologies: Post-splenectomy, iron deficiency anemia, malignancy, chronic inflammation or infection.
- Platelets are numerous but functionally normal.
- Essential Thrombocythemia (ET):
- Myeloproliferative neoplasm (MPN) with autonomous platelet production.
- Key mutations: JAK2, CALR, MPL.
- Presents with thrombosis (arterial/venous), erythromelalgia (burning pain in hands/feet), or bleeding.
⭐ Despite high platelet numbers, paradoxical bleeding can occur when counts exceed 1 million/μL due to acquired von Willebrand syndrome, as platelets adsorb and clear large vWF multimers.
High‑Yield Points - ⚡ Biggest Takeaways
- Immune Thrombocytopenic Purpura (ITP) involves IgG anti-GpIIb/IIIa antibodies, often post-viral in children.
- Thrombotic Thrombocytopenic Purpura (TTP) results from ADAMTS13 deficiency, causing uncleaved vWF multimers and a classic pentad.
- Hemolytic Uremic Syndrome (HUS) is typically due to Shiga-like toxin (E. coli O157:H7), causing a triad of MAHA, thrombocytopenia, and AKI.
- Bernard-Soulier syndrome is a GpIb defect causing impaired adhesion and giant platelets.
- Glanzmann thrombasthenia is a GpIIb/IIIa defect causing impaired aggregation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

