Definition & Diagnosis - Pressure Points
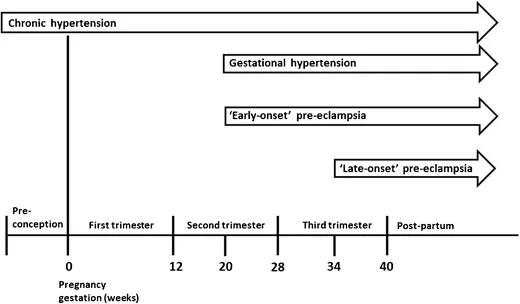
- Definition: Hypertension (SBP ≥ 140 or DBP ≥ 90 mmHg) that is:
- Present before pregnancy.
- Diagnosed before 20 weeks of gestation.
- Persists > 12 weeks postpartum.
- Diagnostic Criteria:
- BP ≥ 140/90 mmHg on 2 occasions at least 4 hours apart.
- Baseline Evaluation:
- Assess for end-organ damage & risk of superimposed preeclampsia.
- Labs: CBC, CMP (LFTs, Creatinine), Urinalysis, Urine Protein/Creatinine ratio.
⭐ Women with chronic hypertension have a 10-25% risk of developing superimposed preeclampsia.
Maternal & Fetal Risks - A Double Danger
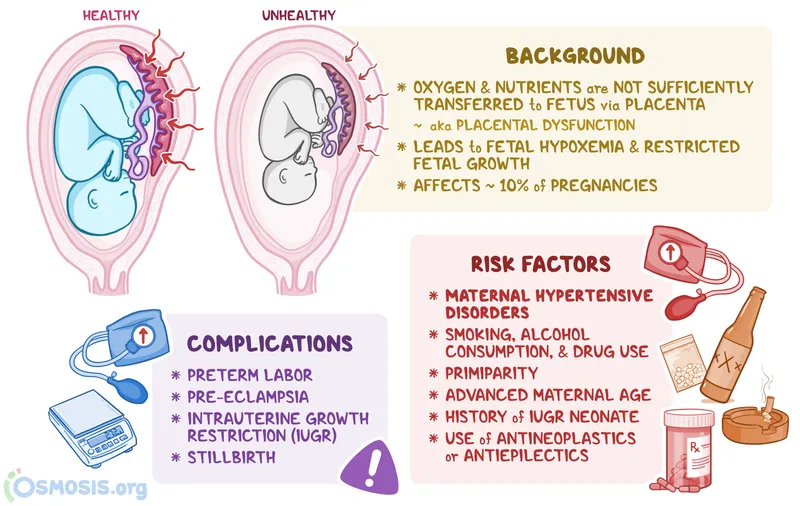
Chronic hypertension creates a hostile uterine environment, jeopardizing both mother and fetus through vascular and placental compromise.
-
Maternal Risks:
- Superimposed Preeclampsia: Develops in ~25% of cases.
- Placental Abruption: Acute, life-threatening separation.
- ↑ rates of Cesarean Delivery.
- End-organ damage: Stroke, pulmonary edema, renal failure.
- Postpartum hemorrhage.
-
Fetal Risks:
- Fetal Growth Restriction (FGR): Resulting from uteroplacental insufficiency.
- Preterm Birth: Often iatrogenic.
- Oligohydramnios
- Intrauterine fetal demise (IUFD).
⭐ Superimposed preeclampsia is the most common and feared maternal complication, dramatically worsening prognosis for both mother and baby. It's a key sentinel event to monitor for.
Antenatal Management - The Control Tower
- Goal: Maintain blood pressure < 140/90 mmHg.
- Pharmacotherapy:
- 1st Line: Labetalol, Nifedipine (long-acting), Methyldopa.
- 📌 Mnemonic: Hypertensive Moms Love Nifedipine.
- ⚠️ AVOID: ACE inhibitors, ARBs, renin inhibitors (teratogenic).
- Preeclampsia Prophylaxis:
- Low-dose Aspirin (81 mg/day) initiated between 12-16 weeks gestation.
- Fetal Surveillance:
- Serial growth ultrasounds and antenatal testing (NST, BPP) starting in the 3rd trimester.
⭐ Delivery for well-controlled chronic hypertension is recommended at ≥38 0/7 weeks. If severe or refractory, delivery may occur earlier after maternal stabilization.
Delivery & Postpartum - The Final Lap
- Delivery Timing: Guideline-driven, balancing maternal risk & neonatal maturity.
- Well-controlled cHTN: 38 0/7 - 39 6/7 wks.
- Poorly controlled / superimposed preeclampsia: Consider delivery at ≥37 0/7 wks.
- Intrapartum Management:
- Target BP <160/110 mmHg.
- IV Labetalol or Hydralazine for severe hypertension.
- Postpartum Care:
- Continue close BP monitoring for 72 hrs inpatient.
- Breastfeeding-safe meds: Labetalol, Nifedipine.
- Re-evaluate therapy 2 weeks postpartum.
⭐ High-Yield: Blood pressure often peaks 3-6 days postpartum, a period of high vulnerability. Schedule a follow-up BP check 7-10 days after discharge.
High-Yield Points - ⚡ Biggest Takeaways
- Defined as BP ≥140/90 mmHg before pregnancy or at <20 weeks gestation.
- Significantly increases risk for superimposed preeclampsia, placental abruption, and fetal growth restriction (FGR).
- First-line medications safe in pregnancy are Labetalol, Nifedipine, and Methyldopa.
- ACE inhibitors and ARBs are strictly contraindicated due to severe fetal toxicity.
- The management goal is to maintain BP <140/90 mmHg to reduce maternal and fetal complications.
- Delivery is typically planned at 38-39 weeks for well-controlled hypertension without complications.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

