Physiologic Changes - The Overworked Pump
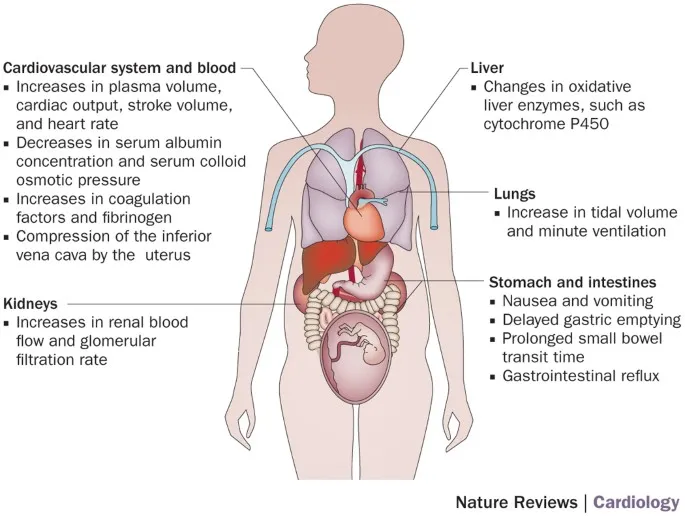
- Blood Volume: ↑ 40-50%, with plasma volume increasing more than red cell mass, causing physiologic anemia.
- Cardiac Output (CO): ↑ 30-50%, peaking in the second trimester. Driven by ↑ stroke volume and ↑ heart rate (15-20 bpm).
- Systemic Vascular Resistance (SVR): ↓ ~20% due to progesterone-mediated smooth muscle relaxation and AV shunting to the placenta.
- Physical Exam: Expect peripheral edema, a systolic flow murmur, and a third heart sound (S3).
⭐ Exam Favorite: Blood pressure, particularly diastolic, reaches its lowest point (nadir) during the second trimester. This can mask a diagnosis of chronic hypertension if the first prenatal visit occurs during this period.
Risk Stratification - Gauging the Danger
-
WHO Classification (Modified): Stratifies maternal cardiovascular risk from I (low) to IV (extremely high).
- WHO I: Uncomplicated, repaired lesions (e.g., PDA, ASD).
- WHO II: Most arrhythmias, unrepaired ASD/VSD.
- WHO III: Mechanical valves, Fontan circulation, cyanotic heart disease.
- WHO IV (Contraindicated): Severe pulmonary arterial hypertension (PAH), LVEF <30%, severe mitral stenosis.
-
CARPREG II Score: Predicts adverse maternal cardiac events based on:
- Prior cardiac event (heart failure, TIA, arrhythmia).
- NYHA class >II or cyanosis.
- Left heart obstruction.
- Reduced systemic ventricular function (LVEF <40%).
⭐ Severe pulmonary hypertension (WHO Class IV) carries the highest risk of maternal mortality, approaching 30-50%.
Specific Conditions - When Hearts Falter
-
Mitral Stenosis: Most common rheumatic valvular lesion in pregnancy. Poorly tolerated due to ↑ plasma volume causing ↑ left atrial pressure & pulmonary edema. Manage with β-blockers & diuretics.
-
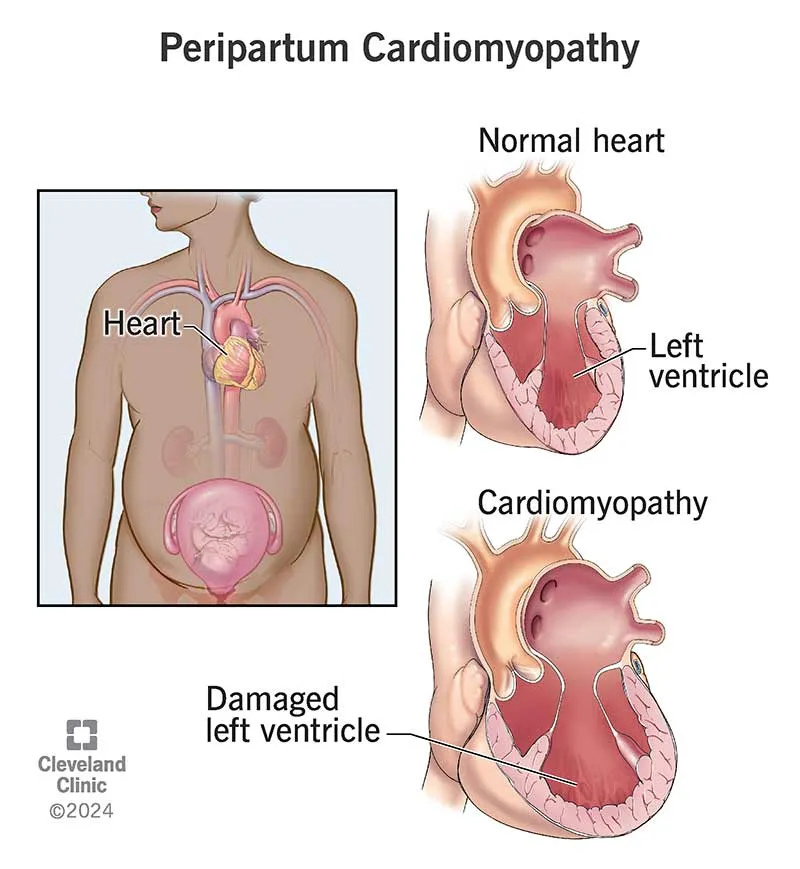
Peripartum Cardiomyopathy (PPCM): Idiopathic heart failure in the last month of pregnancy or within 5 months postpartum.
- Diagnosis: New-onset LV systolic dysfunction (LVEF < 45%).
- Management: Standard heart failure therapy (hydralazine, nitrates, diuretics). Avoid ACE inhibitors/ARBs during pregnancy.
-
Eisenmenger Syndrome: Severe pulmonary HTN with a reversed (right-to-left) shunt. Carries the highest maternal mortality risk (>50%); pregnancy is contraindicated.
⭐ Exam Favorite: Risk of PPCM recurrence is 30-50%. Counsel patients on the high risk with future pregnancies, especially if LV function has not completely recovered.
Management - The Final Gauntlet
- Multidisciplinary team (Cardiology, MFM, Anesthesia) guides peripartum care.
- Goal: Minimize cardiac stress. Vaginal delivery is preferred.
- Anesthesia: Early epidural to blunt catecholamine surge from pain.
⭐ The greatest hemodynamic shifts and risk of decompensation occur immediately postpartum. Autotransfusion from the involuting uterus adds ~500 mL of volume to central circulation, which can overwhelm a compromised heart.
High‑Yield Points - ⚡ Biggest Takeaways
- Physiologic cardiovascular changes (↑ cardiac output, ↓ SVR) can unmask or worsen underlying heart disease.
- The highest risk period for decompensation is at 28-32 weeks gestation and the immediate postpartum period.
- Mitral stenosis is the most common rheumatic lesion and is poorly tolerated due to tachycardia and volume load.
- Peripartum cardiomyopathy is a diagnosis of exclusion for new-onset heart failure in late pregnancy or postpartum.
- Management favors vaginal delivery with epidural analgesia to minimize cardiac strain.
- ACE inhibitors, ARBs, and warfarin are contraindicated during pregnancy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

