Bladder Gross Anatomy - The Bodily Balloon
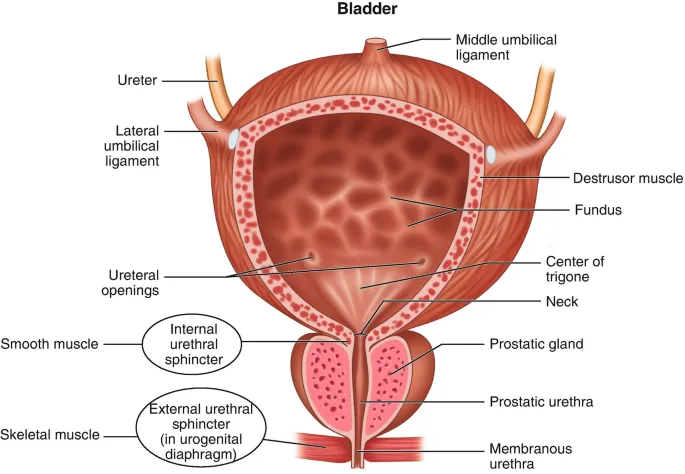
- Location: True pelvis, posterior to the pubic symphysis; primarily retroperitoneal.
- Key Parts:
- Apex: Anterosuperior aspect, points to the pubic symphysis. Attached to the median umbilical ligament (urachal remnant).
- Body: Main area between the apex and fundus.
- Fundus: Posterior wall (base).
- Neck: Inferior constricted part, opens into the urethra.
- Trigone: Smooth, triangular mucosal area on the fundus, defined by the two ureteric orifices and the internal urethral orifice.
- Musculature: Composed of the detrusor muscle (smooth muscle).
⭐ The trigone has a separate embryological origin (mesoderm) from the rest of the bladder (endoderm), resulting in its smooth surface.
Bladder & Urethra Neurovasculature - Plumbing & Wiring
- Arterial Supply: Internal iliac a. → superior & inferior vesical arteries.
- Venous Drainage: Vesical venous plexus → internal iliac vein.
- Innervation (Micturition Reflex):
- Sympathetic (Storage): Hypogastric n. (T11-L2) relaxes detrusor, contracts internal sphincter.
- Parasympathetic (Peeing): Pelvic splanchnic n. (S2-S4) contracts detrusor.
- Somatic (Voluntary): Pudendal n. (S2-S4) contracts external sphincter.
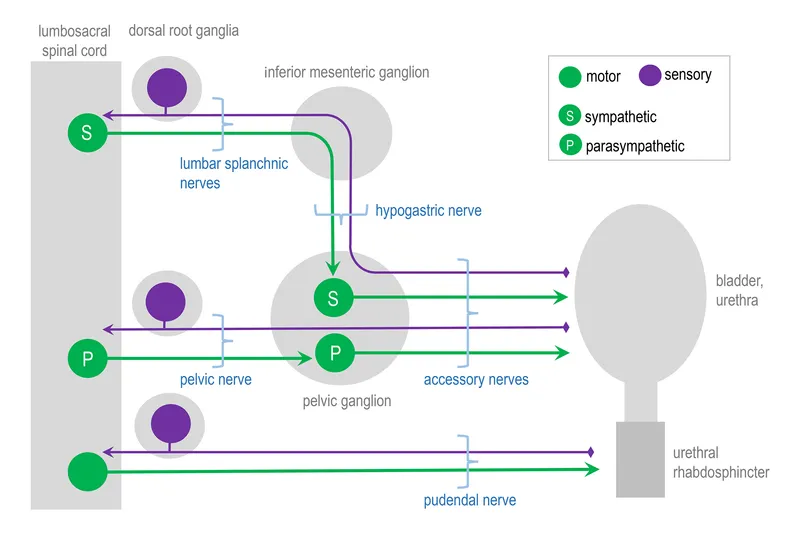
⭐ S2, S3, S4 keep the pee off the floor. This mnemonic links the sacral nerve roots to both parasympathetic (micturition) and somatic (continence) control via the pelvic splanchnic and pudendal nerves.
Male vs. Female Urethra - His and Hers Pipes
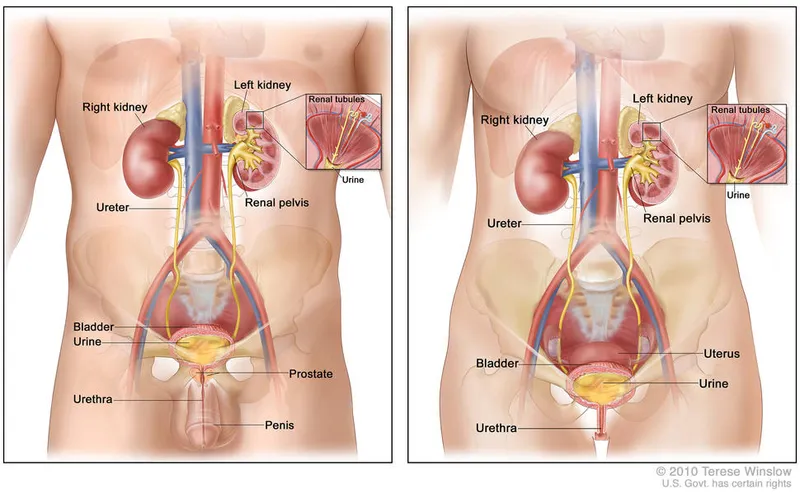
| Feature | Male Urethra | Female Urethra |
|---|---|---|
| Length | ~20 cm | ~4 cm |
| Pathway | Passes through prostate & penis | Passes directly to perineum |
| Segments | Prostatic - Membranous - Spongy (Penile) | Single, short tube |
| Sphincters | Internal & External (more developed) | Internal & External |
| Clinical Risk | ↑ Trauma, strictures, obstruction (BPH) | ↑ Urinary Tract Infections (UTIs) |
Clinical Correlates - When Leaks Happen
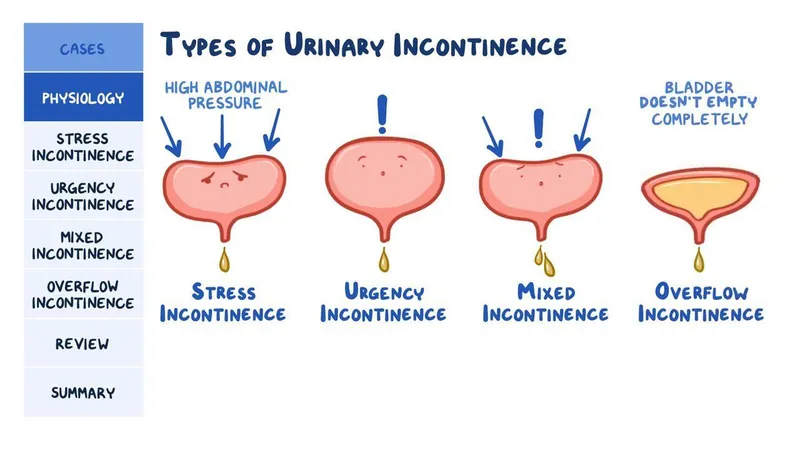
- Stress Incontinence:
- Leakage with ↑ intra-abdominal pressure (e.g., coughing, sneezing, lifting).
- Mechanism: ↓ urethral support from weakened pelvic floor muscles or intrinsic sphincter deficiency.
- Common in multiparous women.
- Urge Incontinence (Overactive Bladder):
- Sudden, compelling desire to void that is difficult to defer, often leading to leakage.
- Mechanism: Uninhibited detrusor muscle contractions (overactivity).
- Can be idiopathic or due to neurological disorders.
- Overflow Incontinence:
- Involuntary release of urine from an overly full bladder, without the urge to urinate.
- Mechanism: Impaired detrusor contractility (e.g., diabetic neuropathy) or bladder outlet obstruction (e.g., BPH).
- Characterized by high post-void residual volume.
⭐ Pudendal nerve (S2-S4) injury, often during childbirth, can weaken the external urethral sphincter, leading directly to stress incontinence.
High‑Yield Points - ⚡ Biggest Takeaways
- The bladder trigone is a smooth-walled area defined by the two ureteric orifices and the internal urethral orifice.
- Micturition is driven by parasympathetic (pelvic splanchnic n., S2-S4) stimulation, causing detrusor muscle contraction.
- Urine storage is a sympathetic function, relaxing the detrusor and contracting the internal urethral sphincter.
- The membranous urethra is the narrowest part in males and most vulnerable to pelvic fracture injury.
- The pudendal nerve provides voluntary control to the external urethral sphincter.
- Stress incontinence involves pelvic floor weakness; urge incontinence involves detrusor overactivity.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

