Granulomatous Inflammation - The Cellular Crew

- Macrophages: The core component.
- Transform into epithelioid histiocytes (elongated, pink cytoplasm), which are secretory, not phagocytic.
- Fuse to form multinucleated giant cells (e.g., Langhans type in TB).
- Lymphocytes: A surrounding collar, primarily CD4+ Th1 cells.
- Orchestrate the response by secreting cytokines.
- Fibroblasts: Encapsulate the granuloma with a rim of fibrosis over time.
⭐ Macrophage activation and differentiation is driven by IFN-γ, secreted by Th1 cells. This cytokine interaction is a classic high-yield point for exams.
Granuloma Formation - Building the Fortress
A cellular attempt to contain an offending agent that is difficult to eradicate. Key players orchestrate a defense.
- Initiation: Antigen-presenting cells (APCs), mainly macrophages, present the antigen to CD4+ helper T cells.
- Cytokine Cascade:
- APCs secrete IL-12, inducing CD4+ T cells to differentiate into Th1 cells.
- Th1 cells then secrete IFN-γ, the critical signal for macrophage activation.
- The Fortress Walls:
- IFN-γ transforms macrophages into immobile, pink-cytoplasm epithelioid histiocytes and fused multinucleated giant cells (Langhans or foreign-body type).
- A collar of lymphocytes surrounds this core.

⭐ TNF-α, secreted by macrophages, is crucial for maintaining the granuloma. Anti-TNF-α drugs (e.g., infliximab) can cause reactivation of latent tuberculosis by breaking down existing granulomas.
Granuloma Types - The Case Files
-
Immune Granulomas: Type IV hypersensitivity. Driven by activated T-cells and macrophages (epithelioid cells).
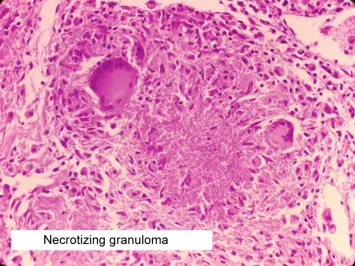
- Caseating: Central necrosis; cheesy, amorphous, eosinophilic core.
- Tuberculosis: Acid-fast bacilli on Ziehl-Neelsen stain.
- Fungal Infections: (e.g., Histoplasma). GMS or PAS stain positive.
- Non-Caseating: No central necrosis; collection of epithelioid cells.
- Sarcoidosis: May contain Schaumann or Asteroid bodies.
- Crohn's Disease: Granulomas found in bowel wall.
- Berylliosis: History of aerospace or electronics industry exposure.
- Caseating: Central necrosis; cheesy, amorphous, eosinophilic core.
-
Foreign Body Granulomas: Response to inert material; not T-cell mediated.
- Contain foreign body giant cells (nuclei scattered).
- Examples: Sutures, talc, splinters.
-
Suppurative/Stellate Granulomas: Central neutrophilic abscess.
- Cat-scratch disease, LGV, Yersiniosis.
⭐ In Sarcoidosis, look for bilateral hilar lymphadenopathy on chest X-ray and elevated serum Angiotensin-Converting Enzyme (ACE) levels.
High‑Yield Points - ⚡ Biggest Takeaways
- A pattern of chronic inflammation defined by collections of activated macrophages (epithelioid histiocytes).
- Primarily driven by a Th1-cell response and the secretion of IFN-γ.
- Differentiated into caseating (e.g., Tuberculosis, with central necrosis) and non-caseating (e.g., Sarcoidosis, Crohn's disease).
- Often contains Langhans giant cells, formed by the fusion of multiple macrophages.
- Its main function is to wall off an offending agent that is difficult to eliminate.
- Can cause hypercalcemia due to 1α-hydroxylase activity in activated macrophages.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

