Prophylaxis - Shields Up, Bugs Down
Primary prophylaxis against opportunistic infections (OIs) is initiated based on specific CD4 count thresholds. The goal is to protect the immunocompromised host before infection occurs. Key recommendations are summarized below.
| CD4 Count (cells/mm³) | Pathogen | Primary Prophylaxis |
|---|---|---|
| < 200 | Pneumocystis jirovecii (PJP) | TMP-SMX |
| < 100 | Toxoplasma gondii | TMP-SMX |
| < 50 | Mycobacterium avium complex (MAC) | Azithromycin |
⭐ Prophylaxis can generally be discontinued once the CD4 count rises above the respective threshold for >3 months on antiretroviral therapy (ART).
CD4 < 200 - The Sub-200 Scoundrels
Pneumocystis jirovecii Pneumonia (PJP) is the hallmark infection in this range. Prophylaxis is critical.
| Feature | Description |
|---|---|
| Pathogen | Pneumocystis jirovecii (fungus) |
| Presentation | Gradual onset of dyspnea on exertion, non-productive cough, fever. Significant hypoxia. |
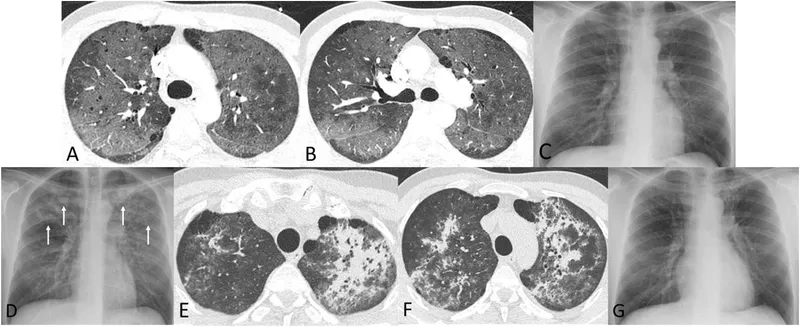
| Diagnosis | CXR: bilateral, diffuse interstitial infiltrates ("bat-wing"). ↑ LDH (>200 U/L). Definitive: BAL with silver stain. |
| Treatment | TMP-SMX. Add steroids if PaO₂ < 70 mmHg or A-a gradient > 35 mmHg. |
⭐ High-Yield: Serum LDH is often dramatically elevated in PJP, disproportionate to the severity of other clinical signs, and can be used to monitor treatment response.
CD4 < 100 - Danger Zone Pathogens
At this stage, patients are at high risk for severe, life-threatening infections. Prophylaxis is critical.

| Pathogen | Presentation | Diagnosis | Prophylaxis/Treatment |
|---|---|---|---|
| Toxoplasma gondii | Multiple ring-enhancing brain lesions, seizures, encephalitis | Serology (IgG), Brain biopsy (definitive) | Prophylaxis: TMP-SMX. Tx: Pyrimethamine + Sulfadiazine + Leucovorin. |
| Cryptococcus neoformans | Meningitis, fever, headache | India ink stain (CSF), Cryptococcal antigen (CrAg) test | Tx: Amphotericin B + Flucytosine, then Fluconazole maintenance. |
| Histoplasma capsulatum | Disseminated: Pancytopenia, HSM, fever, ulcers | Urine/serum antigen, biopsy (oval yeast in macrophages) | Tx: Itraconazole (mild), Amphotericin B (severe). |
CD4 < 50 - Endgame Invaders
| Pathogen | Presentation | Diagnosis | Prophylaxis / Treatment |
|---|---|---|---|
| MAC | Wasting, fever, sweats, diarrhea, anemia. Hepatosplenomegaly. | Blood culture, AFB stain. ↑ALP, ↑LDH. | Prophylaxis: Azithromycin/Clarithromycin. Tx: Clarithromycin + Ethambutol. |
| CMV | Retinitis (“pizza-pie”), esophagitis (linear ulcers), colitis, pneumonitis, encephalitis. | Fundoscopy, biopsy with owl’s eye inclusions. | Tx: Valganciclovir, Ganciclovir. Foscarnet for resistance. |
High‑Yield Points - ⚡ Biggest Takeaways
- The CD4 count is the primary predictor of opportunistic infection (OI) risk.
- Pneumocystis jirovecii pneumonia (PJP) is the classic OI at CD4 < 200 cells/mm³.
- Toxoplasma gondii (ring-enhancing lesions) and Cryptococcus neoformans (meningitis) occur at CD4 < 100.
- Mycobacterium avium complex (MAC) and CMV retinitis are critical concerns at CD4 < 50.
- Prophylaxis (e.g., TMP-SMX for PJP/Toxo, azithromycin for MAC) is guided by CD4 thresholds.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

