Quick Overview
Upper GI bleeding (UGIB) is defined as haemorrhage proximal to the ligament of Treitz. Annual incidence: 50-150/100,000, with 10-14% mortality. NICE NG158 emphasizes risk stratification (Glasgow-Blatchford Score pre-endoscopy, Rockall post-endoscopy), immediate resuscitation, and timing of endoscopy based on risk. Variceal vs non-variceal bleeding requires distinct management pathways.
Core Facts & Concepts
Risk Stratification Systems:
| Score | Timing | Variables | Use |
|---|---|---|---|
| Glasgow-Blatchford (GBS) | Pre-endoscopy | Urea, Hb, BP, pulse, melaena, syncope, hepatic/cardiac disease | Score ≥1: needs intervention; Score 0: safe for outpatient |
| Rockall | Post-endoscopy | Age, shock, comorbidity, diagnosis, stigmata of bleeding | Predicts rebleeding/mortality |
Key Numbers:
- 🩸 Transfusion threshold: Hb <70 g/L (restrictive strategy); consider <100 g/L if acute coronary syndrome
- 📊 GBS = 0: 0.5% risk of intervention/death; safe for discharge
- ⏱️ Endoscopy timing: <24h unstable patients; within 24h for all others (NICE NG158)
- 🚩 Massive bleed: >30% blood volume loss or ongoing haemodynamic instability
Initial Management (NICE NG158):
- ABC approach: 2× large-bore IV cannulae (16G)
- Crystalloid resuscitation (target systolic BP >100 mmHg)
- Tranexamic acid: Consider within 3h of bleeding onset
- Cross-match 4-6 units; activate major haemorrhage protocol if needed
- NBM status for endoscopy
Problem-Solving Approach
Immediate Assessment (First 15 minutes):
- Haemodynamic stability: Pulse, BP, capillary refill, urine output
- Calculate GBS: Determines admission vs discharge
- Bloods: FBC, U&E (urea:creatinine ratio >100 suggests UGIB), coagulation, LFTs, group & save/cross-match
- Stigmata of chronic liver disease: Spider naevi, ascites, jaundice → suspect varices
- Drug history: NSAIDs, anticoagulants, antiplatelets, SSRIs
🚩 Red Flags for Immediate Endoscopy (<24h):
- Haemodynamic instability despite resuscitation
- GBS ≥12
- Suspected variceal bleeding
- Inpatient with active bleeding
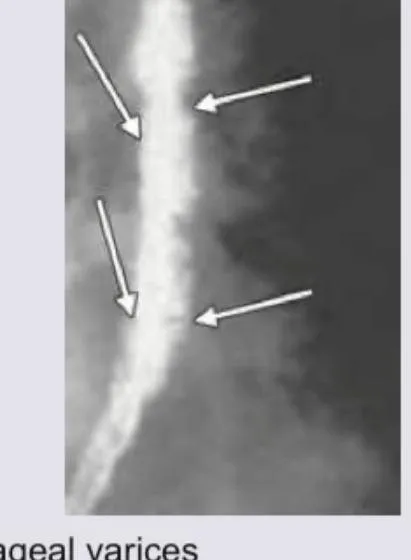
Variceal vs Non-Variceal Pathway:
VARICEAL (suspect if chronic liver disease):
- Terlipressin 2mg IV bolus, then 1-2mg/4-6h for 5 days
- Prophylactic antibiotics: Ceftriaxone 1g IV daily (reduces infection/mortality by 20%)
- Urgent endoscopy: variceal band ligation (first-line) or sclerotherapy
- Sengstaken-Blakemore tube: temporary bridge if uncontrolled
NON-VARICEAL:
- PPI therapy: High-dose IV (e.g., omeprazole 80mg bolus, then 8mg/h infusion) post-endoscopy for high-risk lesions
- Endoscopic therapy: adrenaline injection + thermal coagulation/clips for Forrest Ia/Ib/IIa lesions
Analysis Framework
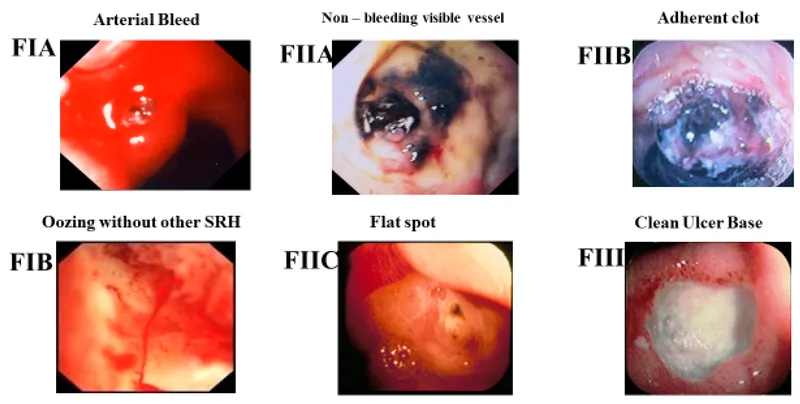
Forrest Classification (Peptic Ulcer Bleeding):
| Grade | Description | Rebleed Risk | Endoscopic Treatment |
|---|---|---|---|
| Ia | Spurting arterial bleed | 90% | Yes - dual therapy |
| Ib | Oozing bleeding | 50% | Yes - dual therapy |
| IIa | Visible vessel | 40% | Yes - dual therapy |
| IIb | Adherent clot | 20% | Consider therapy |
| IIc | Haematin base | 5% | No |
| III | Clean ulcer base | 3% | No |
Differential Diagnosis by Presentation:
- Haematemesis (fresh blood): Oesophageal/gastric source, rapid bleeding
- Coffee-ground vomit: Slower gastric bleeding, acid exposure
- Melaena alone: Duodenal/small bowel (sticky, black, offensive stool)
Visual Aid
Transfusion Strategy (NICE NG158):
| Clinical Context | Threshold | Target |
|---|---|---|
| Standard | Hb <70 g/L | 70-90 g/L |
| ACS/significant CVD | Hb <100 g/L | 100 g/L |
| Ongoing bleeding | Clinical judgment | Maintain perfusion |
Key Points Summary
✓ GBS = 0: Safe for outpatient management; GBS ≥1 requires admission (NICE NG158)
✓ Transfusion: Restrictive strategy (Hb <70 g/L) reduces mortality vs liberal approach
✓ Variceal bleeding: Terlipressin + prophylactic antibiotics (ceftriaxone) + urgent endoscopy with banding
✓ High-dose PPI: Only indicated post-endoscopy for high-risk non-variceal lesions (Forrest Ia-IIa)
✓ Endoscopy timing: <24h if unstable/high-risk; within 24h for all admitted patients
✓ Dual endoscopic therapy: Adrenaline injection PLUS mechanical/thermal method for active bleeding/visible vessel
✓ Anticoagulant management: Reverse if life-threatening; balance thrombotic vs bleeding risk with haematology input
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more