Quick Overview
Epilepsy is a neurological disorder characterized by recurrent unprovoked seizures (≥2 seizures >24 hours apart). Status epilepticus (SE) is a life-threatening emergency requiring immediate intervention. NICE NG217 provides evidence-based guidance on diagnosis, when to initiate treatment, first-line AED selection, and legal driving requirements-all critical for safe, effective management.
Core Facts & Concepts
Definitions & Thresholds
- Epilepsy diagnosis: ≥2 unprovoked seizures >24 hours apart OR 1 seizure + high recurrence risk (>60% over 10 years)
- Status epilepticus: Seizure lasting ≥5 minutes OR ≥3 seizures in 1 hour without full recovery
- Provoked seizure: Identifiable acute cause (hypoglycemia, alcohol withdrawal, acute stroke, CNS infection)
Seizure Classification (ILAE 2017)
| Type | Subtypes | Key Features |
|---|---|---|
| Focal | Aware/Impaired awareness | Originates one hemisphere; may generalize |
| Generalized | Tonic-clonic, Absence, Myoclonic, Atonic | Bilateral onset from start |
| Unknown onset | - | Insufficient information |
First-Line AED Selection (NICE NG217)
- Focal seizures: Lamotrigine or levetiracetam (carbamazepine if unsuitable)
- Generalized tonic-clonic: Sodium valproate (males), lamotrigine/levetiracetam (females of childbearing potential)
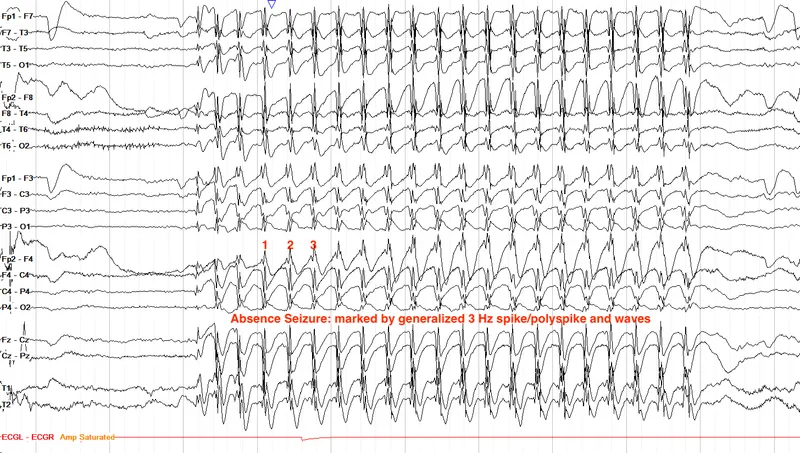
- Absence seizures: Ethosuximide or sodium valproate
- Myoclonic seizures: Sodium valproate or levetiracetam
⚠️ Warning: Avoid sodium valproate in women of childbearing potential unless Pregnancy Prevention Programme in place (teratogenicity risk 30-40%)
Problem-Solving Approach
Status Epilepticus Emergency Protocol (NICE NG217)
- 0-5 minutes: ABCDE approach, secure airway, high-flow O₂, check glucose, IV access
- 5-10 minutes: Benzodiazepine (first-line)
- IV lorazepam 4mg (repeat once after 10 minutes if ongoing)
- Alternatives: Buccal midazolam 10mg OR rectal diazepam 10-20mg
- 10-25 minutes: If seizure continues after 2 benzodiazepine doses → second-line
- IV levetiracetam 60mg/kg (max 4.5g) OR
- IV phenytoin 20mg/kg (max rate 50mg/min) OR
- IV valproate 40mg/kg (max 3g)
- 25+ minutes: Refractory SE → call anesthetics for intubation, propofol/thiopental, ICU transfer

When to Start Treatment After First Seizure
- Start AED if: Brain imaging abnormality, EEG showing epileptiform activity, nocturnal seizure, or recurrence risk >60%
- Otherwise: Discuss risks/benefits; many clinicians defer until second seizure
Analysis Framework
Differential Diagnosis: Seizure vs. Syncope vs. Non-Epileptic Attack
| Feature | Seizure | Syncope | Non-Epileptic Attack |
|---|---|---|---|
| Duration | 1-3 minutes | <30 seconds | >5 minutes (variable) |
| Posture | Any position | Upright → falls | Often witnessed, gradual |
| Tongue biting | Lateral (specific) | Rare | Tip (non-specific) |
| Post-ictal confusion | Minutes-hours | Seconds | Absent or prolonged |
| Eyes during event | Open | Closed | Closed (resists opening) |
| Injury | Common (falls, burns) | Possible | Rare |
Red Flags Requiring Urgent Investigation
- 🚩 First seizure in adult >25 years (exclude tumor, stroke)
- 🚩 Focal neurology (suggests structural lesion)
- 🚩 Persistent fever/headache (CNS infection)
- 🚩 Head trauma within 3 months
Visual Aid
Driving Regulations (DVLA - UK)
| License Type | Requirement |
|---|---|
| Group 1 (car/motorcycle) | Seizure-free 12 months OR established 3-year pattern of sleep-only seizures |
| Group 2 (HGV/PCV) | Seizure-free 10 years off AEDs (5 years for provoked seizure) |
| After first seizure | 6 months off driving (Group 1) if low recurrence risk |
Key Points Summary
✓ Status epilepticus: Treat at 5 minutes with IV lorazepam 4mg (repeat once); second-line at 10-25 minutes with levetiracetam/phenytoin/valproate
✓ First-line AEDs: Focal = lamotrigine/levetiracetam; Generalized TC = valproate (males) or lamotrigine (females); Absence = ethosuximide
✓ Start AED after first seizure if: Brain lesion, epileptiform EEG, nocturnal seizure, or recurrence risk >60%
✓ Avoid valproate in women of childbearing age unless Pregnancy Prevention Programme (30-40% teratogenicity risk)
✓ Driving: Group 1 requires 12 months seizure-free; Group 2 requires 10 years off AEDs
✓ Lateral tongue biting + post-ictal confusion strongly suggest true epileptic seizure vs. syncope/non-epileptic attack
✓ Red flags: First seizure >25 years, focal neurology, fever/headache → urgent imaging/LP to exclude tumor/stroke/infection
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

