Anatomy & Etiology - Liver's Weak Spots
- Relevant Anatomy:
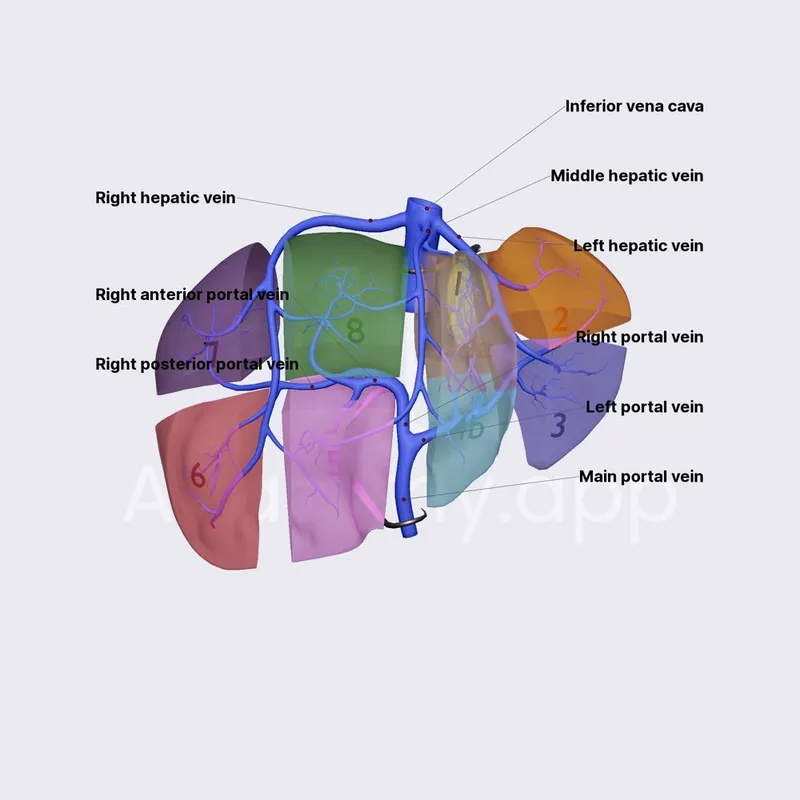
- Lobes (Right/Left), 8 Couinaud segments.
- Ligaments: Falciform, coronary, triangular.
- Dual Blood Supply: Portal Vein (75%), Hepatic Artery (25%).
- Glisson's capsule: Fibrous, pain-sensitive covering.
- Mechanisms of Injury:
- Blunt Trauma: Most common (e.g., MVCs, falls, direct blows).
- Penetrating Trauma: (e.g., GSW, stab wounds).
- Common Injury Sites: Posterior segments of the right lobe (especially VI, VII, VIII).
⭐ The right lobe of the liver is injured in approximately 75-80% of cases of hepatic trauma, with segments VI, VII, and VIII being most commonly affected.
 oka
oka
Classification & Diagnosis - Grading the Hurt
AAST (American Association for the Surgery of Trauma) Liver Injury Scale:
| Grade | Key Features |
|---|---|
| I | Subcapsular hematoma <10% SA; Capsular tear <1cm depth. |
| II | Subcapsular hematoma 10-50% SA; Intraparenchymal <10cm; Laceration 1-3cm depth, <10cm length. |
| III | Subcapsular hematoma >50% SA / expanding / ruptured; Intraparenchymal >10cm / expanding; Laceration >3cm depth. |
| IV | Laceration 25-75% hepatic lobe OR 1-3 Couinaud segments (single lobe). |
| V | Laceration >75% hepatic lobe OR >3 Couinaud segments; Juxtahepatic venous injuries. |
| VI | Hepatic avulsion. |
Diagnostic Approach:
- Initial: ATLS principles (ABCDE).
- Hemodynamically Stable:
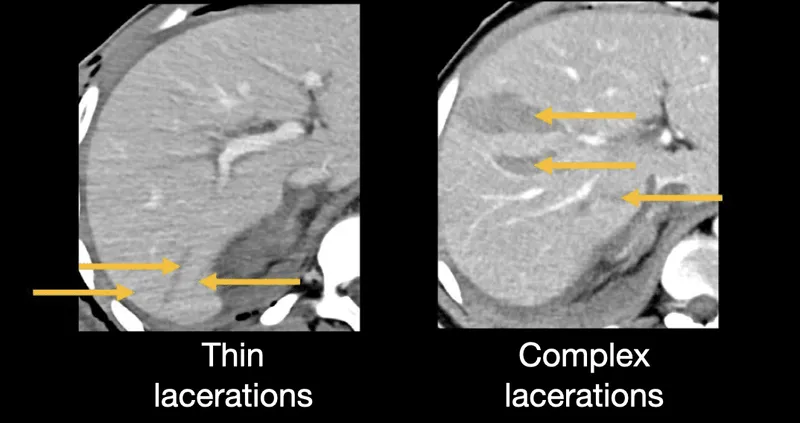
- CT scan with IV contrast (gold standard).
- Findings: Laceration, hematoma (subcapsular, intraparenchymal), active contrast extravasation, pseudoaneurysm.
- Hemodynamically Unstable:
- FAST scan (Focused Assessment with Sonography for Trauma) for free fluid.
- If FAST equivocal/unavailable: DPL (Diagnostic Peritoneal Lavage).
- Or direct laparotomy.
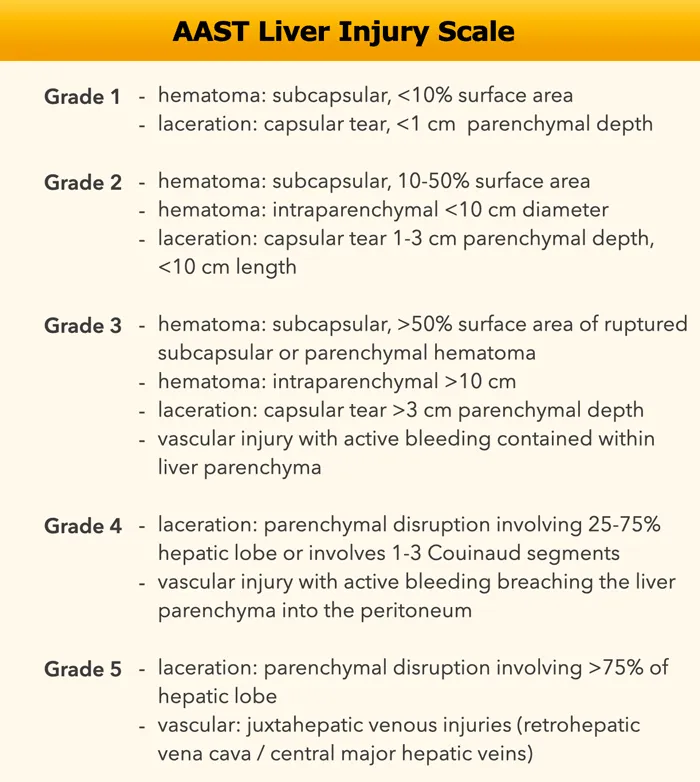
⭐ The AAST liver injury scale is crucial for guiding management decisions, particularly for non-operative management (NOM) candidacy.
Management Principles - Stop the Bleed!
- Non-Operative Management (NOM): Standard for stable blunt liver trauma.
- Criteria: Hemodynamic stability, no peritonitis/laparotomy indications.
- CT: Grade; contrast blush → consider angioembolization.
- Monitoring: ICU (high-grade); serial Hct, vitals, abdominal exams.
- Failure: Instability, peritonitis, transfusion >4 units PRBC.
- Operative Management (OM):
- Indications: Hemodynamic instability (post-resuscitation), peritonitis, evisceration, other surgical injuries.
- Damage Control Surgery (DCS): For exsanguination.
- Principles: Abbreviated laparotomy → control hemorrhage (packing, Pringle) & contamination → temporary closure → ICU → re-laparotomy.
- Pringle Maneuver: Clamps hepatoduodenal ligament. 📌 'Pinch the Pedicle'.
- Controls most hepatic bleeding. Intermittent: 15-20 min on, 5 min off.
⭐ Non-operative management is standard for hemodynamically stable blunt liver trauma, regardless of injury grade, with appropriate resources (ICU, IR, surgery).

Operative Techniques & Complications - Surgical Fixes & Woes
- Surgical Fixes (when NOM fails/contraindicated):
- Hepatorrhaphy: Suture for superficial lacerations.
- Perihepatic packing: For diffuse bleeding (Damage Control Surgery).
- Resectional debridement: Devitalized tissue removal.
- Omental packing/patch: Deep lacerations.
- Hepatic artery ligation: Selective, for persistent arterial bleed.
- Balloon tamponade: For tract injuries.
- Anatomic resection: Rarely indicated in trauma.

- Angioembolization:
⭐ Angioembolization is a critical adjunct in both non-operative and operative management of liver trauma, particularly for controlling arterial hemorrhage identified by contrast extravasation on CT.
- Role in NOM (arterial blush on CT) & post-op.
- Complications (Woes): 📌 'BILE HAPpens': Bleeding, Infection/abscess, Leak (bile), Edema (compartment syndrome), Hematoma, AV fistula, Pseudoaneurysm.
- Early: Re-bleeding (↑NOM failure/death), abdominal compartment syndrome.
- Delayed: Bile leak/biloma (most common; percutaneous Rx), intra-abdominal abscess, pseudoaneurysm, AV fistula, post-traumatic biliary stricture.
- Key Mortality Factors: Associated injuries, admission shock, high AAST grade, coagulopathy, massive transfusion.
High‑Yield Points - ⚡ Biggest Takeaways
- Liver is the most common solid organ injured in blunt abdominal trauma.
- Right lobe is more frequently affected than the left.
- Non-Operative Management (NOM) is standard for hemodynamically stable patients.
- Contrast-Enhanced CT (CECT) is gold standard for diagnosis and grading.
- AAST liver injury scale (Grades I-VI) is crucial for guiding management.
- Perihepatic packing is a key damage control surgery technique for unstable patients.
- Common complications include bile leak, abscess, and delayed hemorrhage (biloma).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

