Physiological Stresses - Gasping for Gains & Air
Exercise:
- ↑ O₂ demand, ↑ CO₂ production → ↑ alveolar ventilation (hyperpnea).
- PaO₂, PaCO₂, pH largely normal in moderate exercise.
- Drives: Neurogenic (central command, proprioceptors) & humoral (K⁺, temp).
- Anaerobic threshold: Lactic acidosis → further ↑ ventilation.
- VO₂ max: Index of cardiorespiratory fitness.
High Altitude (HA):
- ↓ Barometric pressure → ↓ $P_IO_2$ → hypoxic hypoxia.
- Acute: Hyperventilation (via peripheral chemoreceptors) → respiratory alkalosis.
- AMS (Acute Mountain Sickness) common.
- Acclimatization (days-weeks):
- Sustained hyperventilation; renal HCO₃⁻ excretion (pH normalization).
- ↑ 2,3-DPG → ODC right shift (↑ O₂ unloading).
- ↑ Erythropoietin (EPO) → ↑ Hb & Hct.
- Chronic hypoxic pulmonary vasoconstriction → risk of pulmonary hypertension/HAPE.
⭐ At high altitude, initial hyperventilation causes respiratory alkalosis; renal excretion of HCO₃⁻ compensates over days, returning pH towards normal.

Altered Gas Exchange - Balancing Act
- Hypoxemia (↓ $P_aO_2$): Low blood oxygen.
- Key Causes: V/Q mismatch (PE, pneumonia), shunt (ARDS), hypoventilation, diffusion impairment (fibrosis), ↓ $P_IO_2$ (altitude).
- Acute Response: Hyperventilation (via peripheral chemoreceptors), ↑ cardiac output.
- Chronic Adaptation: Polycythemia, ↑ 2,3-DPG (improves O₂ release).
- 📌 A-a gradient ($P_AO_2 - P_aO_2$): Normal (<15 mmHg) in hypoventilation & ↓ $P_IO_2$; ↑ in V/Q mismatch, shunt, diffusion defect.
- Hypercapnia (↑ $P_aCO_2$): Excess CO₂ retention.
- Primary Cause: Alveolar hypoventilation (e.g., COPD, CNS depression, neuromuscular disease).
- Response: ↑ Ventilation (central & peripheral chemoreceptors); renal HCO₃⁻ retention (chronic compensation for respiratory acidosis).
- Hypocapnia (↓ $P_aCO_2$): Low CO₂ levels due to hyperventilation.
- Common Causes: Anxiety, hypoxia (stimulates hyperventilation), metabolic acidosis (respiratory compensation).
- Effects: Respiratory alkalosis, cerebral vasoconstriction (↓ CBF), ↓ ionized Ca²⁺ (risk of tetany).

⭐ > In chronic hypercapnia (e.g., COPD), central chemoreceptors adapt (desensitize) to high $P_aCO_2$; respiratory drive then becomes more dependent on hypoxic stimulus via peripheral chemoreceptors.
Disease State Drama - When Lungs Rebel
- Disease alters lung function, causing distinct patterns.
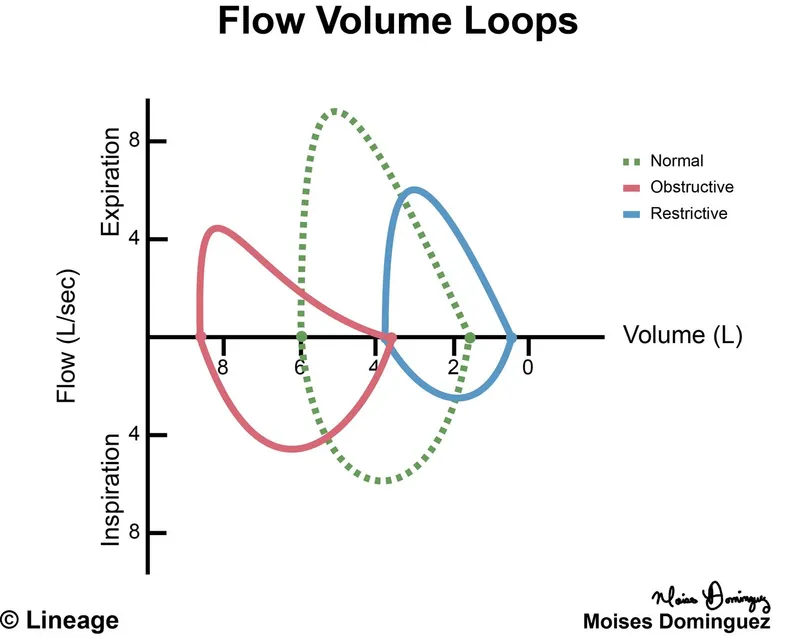
- Obstructive Lung Diseases (OLD): Difficulty exhaling.
- Examples: COPD (Emphysema, Chronic Bronchitis), Asthma.
- Patho: ↑ Airway resistance, air trapping.
- PFTs: ↓ FEV1, ↓ FVC (or normal), FEV1/FVC < 0.7, ↑ RV, ↑ TLC.
- Gas Exchange: Low $V_A/Q_C$ mismatch, $\downarrow P_{a}O_2$, late $\uparrow P_{a}CO_2$.
- 📌 OLD = Outflow problem.
- Restrictive Lung Diseases (RLD): Difficulty inhaling, reduced lung expansion.
- Examples: Fibrosis, ARDS, Myasthenia Gravis, Scoliosis.
- Patho: ↓ Lung compliance, ↓ lung volumes.
- PFTs: ↓ FEV1, ↓ FVC, FEV1/FVC \geq 0.7, ↓ RV, ↓ TLC.
- Gas Exchange: Diffusion impairment/shunt, $\downarrow P_{a}O_2$.
- 📌 RLD = Reduced volumes.
⭐ The FEV1/FVC ratio is a critical differentiator: < 0.7 suggests obstruction, while a normal or increased ratio with reduced FVC and TLC indicates restriction.
High‑Yield Points - ⚡ Biggest Takeaways
- High Altitude: ↑ Ventilation, ↑ 2,3-DPG, polycythemia, respiratory alkalosis.
- Exercise: ↑ V̇E & V̇O₂, improved V/Q matching; PaO₂ & PaCO₂ stable initially.
- COPD: Irreversible airflow obstruction (↓ FEV₁/FVC), air trapping, hypoxemia, hypercapnia.
- Asthma: Reversible bronchoconstriction, inflammation; spirometry shows reversibility.
- RLD: ↓ Lung volumes (↓ TLC, ↓ FVC); FEV₁/FVC normal or ↑.
- V/Q Mismatch: Key cause of hypoxemia; includes shunts (V/Q=0) & dead space (V/Q=∞).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

