Introduction & Etiology - Tiny Tickers Trouble
- Heart Failure (HF): Clinical syndrome where the heart cannot pump enough blood to meet the body's metabolic demands or can do so only at elevated filling pressures.
- Etiology (Common Causes):
- Congenital Heart Defects (CHD): Predominant cause in infancy.
- Volume Overload: Ventricular Septal Defect (VSD), Patent Ductus Arteriosus (PDA).
- Pressure Overload: Aortic Stenosis (AS), Coarctation of Aorta.
- Myocardial Dysfunction: Cardiomyopathies (dilated, hypertrophic), myocarditis.
- Arrhythmias: Persistent tachyarrhythmias or bradyarrhythmias.
- High-Output States: Severe anemia, large AV malformations.

- Congenital Heart Defects (CHD): Predominant cause in infancy.
⭐ In infants, the most common cause of heart failure is a large left-to-right shunt, such as a Ventricular Septal Defect (VSD).
Pathophysiology & Classification - Pump Under Pressure
- Heart failure (HF): Heart unable to meet body's metabolic demands.
- Pathophysiology: ↓ Cardiac Output (CO) triggers neurohormonal activation (SNS, RAAS).
- Initially adaptive; chronic activation → maladaptive ventricular remodeling (hypertrophy, dilation), worsening HF.
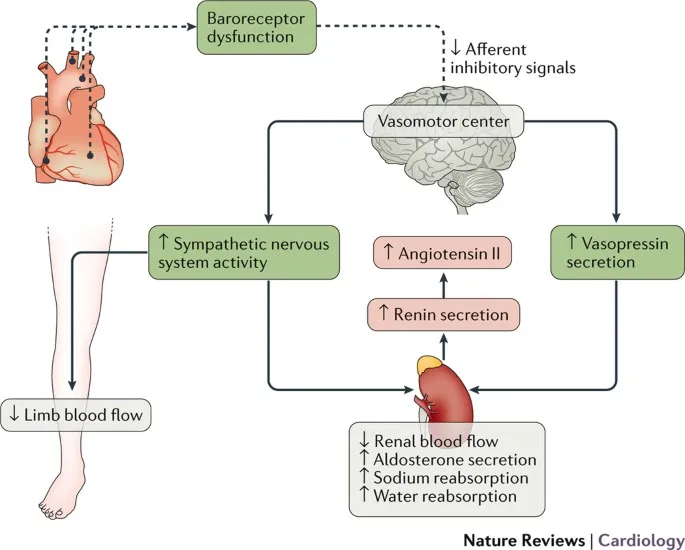
- Initially adaptive; chronic activation → maladaptive ventricular remodeling (hypertrophy, dilation), worsening HF.
- Classification based on:
⭐ BNP & NT-proBNP are key biomarkers; levels ↑ with ventricular wall stress, aiding diagnosis & severity assessment.
Clinical Features & Severity - Spotting the Signs
- Infants & Young Children (Ross Classification):
- Poor feeding, failure to thrive (FTT)
- Tachypnea (>60/min), diaphoresis (esp. with feeds)
- Hepatomegaly (>2-3 cm BCM), irritability
- Ross Class III/IV: Marked symptoms, FTT, symptoms at rest (e.g., grunting)
- Older Children (NYHA-like):
- Dyspnea on exertion, orthopnea
- Fatigue, exercise intolerance
- Peripheral edema, persistent cough
- General Signs: Tachycardia (>160/min infant, >100/min child), S3 gallop, cool extremities, cardiomegaly.
⭐ > In infants, diaphoresis during feeding is a classic sign of heart failure, often mistaken for normal sweating.
Diagnostic Approach - Cracking the Case
- Clinical suspicion: Poor feeding, tachypnea, FTT, tachycardia, hepatomegaly.
- Key Investigations:
- CXR: Cardiomegaly (CTR > 0.6 infants, > 0.5 children), pulmonary venous congestion/edema.

- ECG: Ventricular hypertrophy, arrhythmias.
- Echocardiography: Gold standard. Confirms diagnosis. Assesses structure, function (EF), etiology.
- Biomarkers: ↑ BNP or NT-proBNP levels.
⭐ Elevated BNP/NT-proBNP aids differentiating cardiac vs. non-cardiac dyspnea & correlates with severity.
- CXR: Cardiomegaly (CTR > 0.6 infants, > 0.5 children), pulmonary venous congestion/edema.
Management Strategies - Mending Little Hearts
- Primary Goals: Improve symptoms & quality of life, slow progression, ↑survival. Always treat underlying cause.
- General Measures: Oxygen PRN, optimal nutrition (caloric density), judicious Na+/fluid restriction.
- Pharmacotherapy (Chronic HF):
- Diuretics: Furosemide (loop); Spironolactone (K-sparing, anti-remodeling).
- ACE inhibitors (e.g., Captopril 0.1-0.3 mg/kg/dose TID initially) or ARBs: ↓afterload & ↓preload.
- Beta-blockers (e.g., Carvedilol): Only in stable, euvolemic patients. Start low, titrate slow.
- Digoxin: Positive inotrope for symptomatic relief. Narrow therapeutic index. 📌 Monitor levels & for toxicity (nausea, vomiting, arrhythmia).
- Acute Decompensated HF (ADHF):
- IV loop diuretics (Furosemide).
- IV inotropes (e.g., Milrinone, Dobutamine).
- Oxygen; consider non-invasive/invasive ventilation.
⭐ In ADHF with low output ("cold & wet"), Milrinone (inodilator) is often preferred for reducing preload/afterload.
High‑Yield Points - ⚡ Biggest Takeaways
- Congenital Heart Defects (CHD), especially VSD & PDA, are the primary cause in infants.
- Myocarditis and cardiomyopathies are key acquired causes.
- Clinical signs: Infants show poor feeding, tachypnea, diaphoresis; older children exhibit dyspnea, edema.
- Failure to thrive (FTT) is a common presentation in infants.
- Echocardiography is crucial for diagnosis and assessing cardiac function.
- Mainstay treatment: Diuretics (Furosemide), ACE inhibitors, Digoxin (monitor toxicity).
- Address underlying causes and precipitating factors like anemia or infection.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

