Intro & Virchow's - Clotting 101
- Thrombosis: Pathological intravascular clot (thrombus). Hemostasis: Physiological process (platelets, factors, endothelium) stopping blood loss.
- Virchow's Triad (critical for thrombosis):
- Endothelial Injury: Procoagulant switch (e.g., inflammation, trauma).
- Abnormal Blood Flow: Stasis (e.g., DVT) or turbulence (e.g., aneurysms).
- Hypercoagulability: ↑ procoagulants / ↓ anticoagulants (inherited/acquired).
⭐ Factor V Leiden: most common inherited thrombophilia (Activated Protein C resistance).
- Coagulation Cascade:
- Intrinsic (PTT) & Extrinsic (PT/INR) pathways converge.
- Common pathway: Factor Xa → Thrombin (IIa) → Fibrin clot.
- 📌 Vit. K-dependent factors: II, VII, IX, X; Proteins C & S.
Inherited Causes - Risky Genes
- Key inherited hypercoagulable states predisposing to Venous Thromboembolism (VTE).
- Most are autosomal dominant (AD) with variable penetrance.
- Screening considered in VTE < 50 yrs, recurrent VTE, or strong family history.
| Condition | Gene (Mutation) | Mechanism | Key Point(s) |
|---|---|---|---|
| Factor V Leiden | F5 (G1691A; R506Q) | Factor Va resistant to APC cleavage | Most common; 📌 Leiden = Leading cause |
| Prothrombin Gene Mut. | F2 (G20210A) | ↑ Prothrombin synthesis → ↑ thrombin generation | 2nd most common; ↑ VTE risk 2-3x |
| Protein C Deficiency | PROC1 | Impaired inactivation of FVa & FVIIIa | Warfarin skin necrosis; Neonatal purpura fulminans |
| Protein S Deficiency | PROS1 | Impaired Protein C cofactor activity | Warfarin skin necrosis; Similar to Protein C def. |
| Antithrombin Def. | SERPINC1 | Reduced inactivation of thrombin (IIa) & FXa | Heparin resistance; Highest thrombotic risk |
Acquired Causes - Attack of Clots
- Antiphospholipid Syndrome (APS):
- Autoantibodies: Lupus anticoagulant, Anti-cardiolipin, Anti-β2 GPI.
- Clinical: Venous/arterial thrombosis, recurrent fetal loss.
- Lab: Paradoxical ↑aPTT (Lupus Anticoagulant).
- Heparin-Induced Thrombocytopenia (HIT Type II):
- IgG to PF4-heparin complex → platelet activation → thrombosis & thrombocytopenia (↓platelets >50%).
- Onset 5-10 days post-heparin. 📌 Heparin Induces Thrombosis & Thrombocytopenia.
- Disseminated Intravascular Coagulation (DIC):
- Systemic coagulation activation & consumptive coagulopathy. Causes: Sepsis, trauma, malignancy.
- Malignancy:
- Trousseau's syndrome (migratory thrombophlebitis). Tumor procoagulants.
- Other Risk Factors:
- Immobilization, surgery, OCPs/HRT, nephrotic syndrome, Myeloproliferative Neoplasms (MPNs), PNH.
⭐ Lupus anticoagulant (APS) paradoxically prolongs aPTT in vitro but causes in vivo thrombosis.
DVT/PE & Diagnosis - Clot Detectives
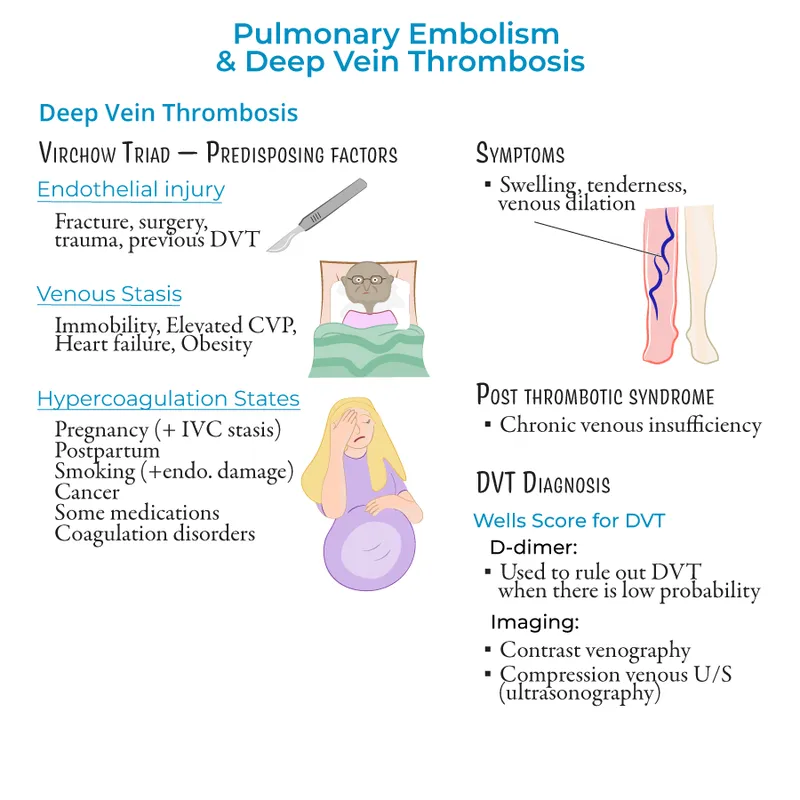
- DVT (Deep Vein Thrombosis):
- Signs: Unilateral leg swelling, pain, warmth, erythema.
- Risk: Virchow's Triad (📌 SHE: Stasis, Hypercoagulability, Endothelial injury).
- Dx: Wells Score (PTP) → D-dimer (if low PTP) → Compression US (Gold Std).
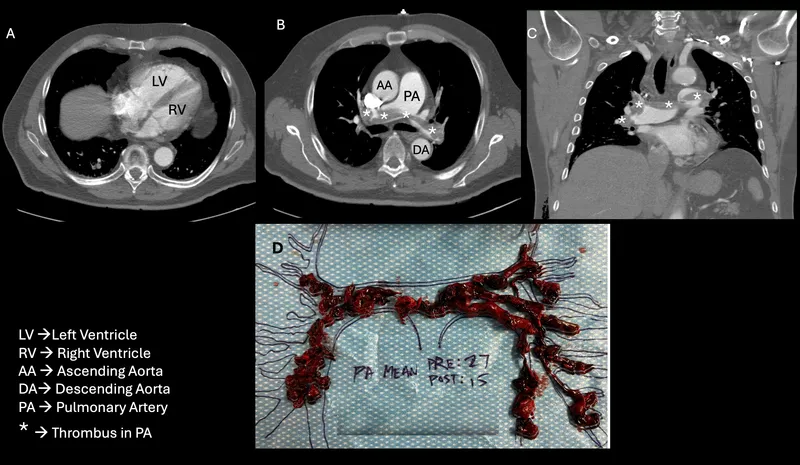
- PE (Pulmonary Embolism):
- Signs: Sudden dyspnea, pleuritic chest pain, cough, hemoptysis, tachycardia.
- Dx: Wells/Geneva Score (PTP) → D-dimer (if low PTP) → CTPA (Gold Std). V/Q if CTPA C/I.
- ECG: S1Q3T3 (classic, rare), sinus tachycardia. ABG: ↓PaO₂, ↓PaCO₂ (resp. alkalosis).
⭐ For suspected PE, if Wells score ≤ 4 (PE unlikely) AND D-dimer is negative, PE can be safely excluded (often guided by PERC rule).
High‑Yield Points - ⚡ Biggest Takeaways
- Virchow's triad (endothelial injury, stasis, hypercoagulability) is fundamental to thrombosis.
- Factor V Leiden (APC resistance) is the most common inherited thrombophilia.
- Antiphospholipid Syndrome (APS) causes thrombosis and pregnancy morbidity with characteristic autoantibodies.
- TTP presents with a pentad (MAHA, thrombocytopenia) due to ADAMTS13 deficiency.
- DIC: widespread microthrombi, consumption coagulopathy, bleeding; ↑D-dimer, ↓fibrinogen.
- Heparin-Induced Thrombocytopenia (HIT) paradoxically causes thrombosis via anti-PF4 antibodies.
- Protein C or S deficiency increases risk of warfarin-induced skin necrosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

