Clinical Applications of Biomechanics - Bones & Bolts
- Fracture Stability Principles:
- Absolute Stability: No motion at fracture site. Goal: Primary bone healing (interfragmentary strain, $\epsilon = \Delta L / L_0$, < 2%). Achieved via compression (e.g., lag screws, compression plates).
- Relative Stability: Controlled motion. Goal: Secondary bone healing via callus (strain 2-10%). Achieved via splinting, IM nails, bridging plates, external fixators.
- Load & Implant Dynamics:
- Load-sharing: Implant & bone share forces (e.g., IM nail). Promotes callus.
- Load-bearing: Implant carries entire load (e.g., bridging plate for comminuted fracture).
- Stress Shielding: Bone resorption if implant is too rigid, reducing bone stress.
- Key Implants & Techniques:
- Plates: Compression (DCP), neutralization, buttress, bridging functions.
- Screws: Lag technique for interfragmentary compression.
- Intramedullary Nails: Load-sharing; for long bone diaphyseal fractures.
- External Fixators: For open fractures, severe soft tissue damage.
- 📌 AO Principles: ARSA (Anatomic Reduction, Stable Fixation, Atraumatic Technique, Active Mobilization).
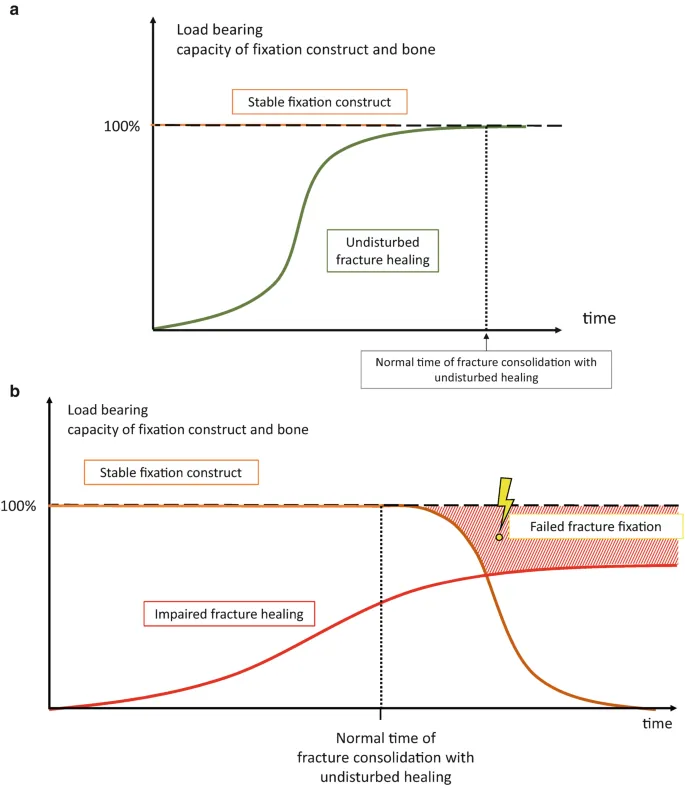
⭐ Dynamic compression plating (DCP) converts torsional and bending forces into axial compression across the fracture site.
Clinical Applications of Biomechanics - Motion Makers
-
Arthroplasty Biomechanics:
- THR: Target acetabular inclination 40±10°, anteversion 15±10° for stability & ROM.
- TKR: Aim for neutral mechanical axis, optimal component alignment & ligament balance.
-
Implant Materials & Properties:
Material Young's Modulus (GPa) Wear Resistance Key Features CoCr ~200-230 Good MoM issues, ion release Ti alloys ~100-120 Moderate Lower stiffness, biocompatible UHMWPE ~1 Fair 📌 'POLY'ethylene wears, XPE wear ↓ Ceramics ~300-400 Excellent Brittle, fracture risk, squeaking -
Wear Mechanisms: Adhesive, abrasive, fatigue, corrosive (tribocorrosion).

-
Fixation & Loosening:
- Cemented (PMMA) vs. Cementless (porous coating for bone ingrowth).
- Stress shielding: Implant-induced bone resorption due to ↓ load.
- Aseptic loosening: Primary long-term failure mode.
⭐ Osteolysis secondary to wear debris (particle disease) is a major cause of long-term failure in total joint arthroplasty.
Clinical Applications of Biomechanics - Column Control
- Denis Three-Column Theory: Assesses spinal stability. 📌 All My Patients (Ant, Mid, Post).
- Anterior: Anterior longitudinal ligament (ALL), anterior 1/2 vertebral body & annulus.
- Middle: Posterior longitudinal ligament (PLL), posterior 1/2 vertebral body & annulus.
- Posterior: Posterior elements (pedicles, facets, lamina, spinous process), ligament complex.
- Instability if ≥2 columns disrupted.
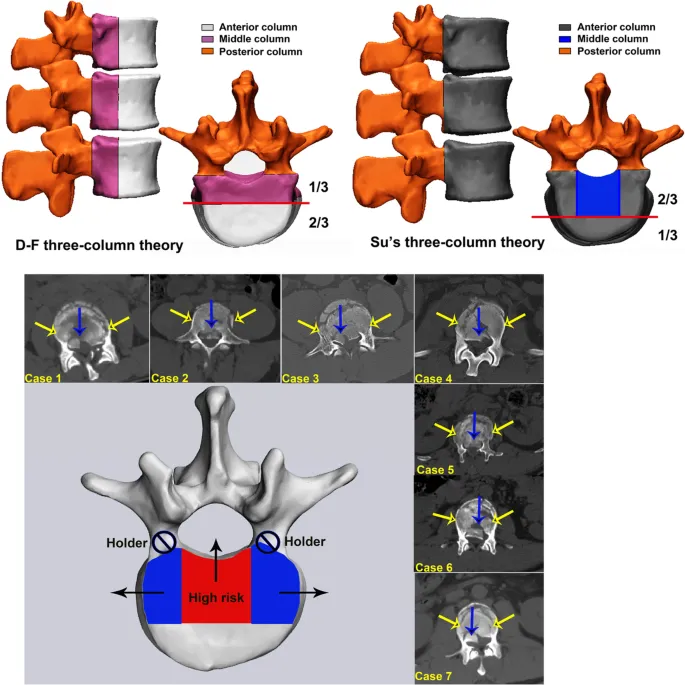
- Mechanisms of Spinal Injury: Axial compression, flexion, extension, rotation, shear, distraction.
- Spinal Instability Indicators:
- Loss of >50% vertebral body height.
- Angulation >20-30°.
- Progressive neurological deficit.
- Biomechanics of Spinal Instrumentation:
- Pedicle screws & rods: Strongest posterior fixation, load bearing.
- Cages (interbody): Restore height, promote fusion, anterior load sharing.
- Plates: Anterior/lateral stabilization.
- Load sharing: Implant + graft share loads until fusion.
- Fusion concepts: Achieve arthrodesis (bony union).

⭐ The 'tension band' principle is frequently applied in spinal fixation to counteract flexion forces and promote stability.
Clinical Applications of Biomechanics - Step & Support
- Normal Gait Cycle:
- Phases: 📌 Stance (IC, LR, MSt, TSt, PSw), Swing (ISw, MSw, TSw).
- Stance Phase Details:
Phase Event Muscle(s) IC Heel strike Tib. Ant. LR Wt. accept Quads, Glutes MSt Single support Glut. Med. TSt Heel off Gastroc/Soleus PSw Toe off Gastroc/Soleus - Parameters: Cadence 90-120 steps/min; Step length ~70-82 cm; Speed 1.2-1.4 m/s. $F_{GRF}$.
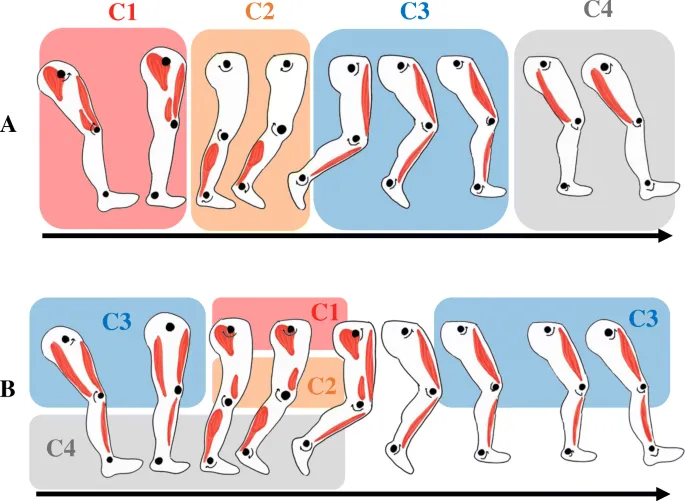
- Pathological Gaits:
- Trendelenburg: Gluteus medius weakness → pelvic drop.
- Antalgic: Pain-induced → shortened stance phase.
- Orthotics: External devices.
- Principles: Three-point pressure for control/correction.
- Materials: Thermoplastics.
 demonstrating force application)
demonstrating force application)
- Prosthetics: Artificial limbs.
- Principles: Alignment, socket fit, energy storage & return.
⭐ A three-point pressure system is a fundamental biomechanical principle used in many orthotic designs to control movement or provide correction.
High‑Yield Points - ⚡ Biggest Takeaways
- Stress shielding causes bone loss around stiff implants, risking loosening.
- Wolff's Law: Bone remodels based on applied stress, impacting healing and implant stability.
- Joint reaction forces influence implant longevity and osteoarthritis progression.
- Biomechanics guides fracture fixation choices: screws, plates, nails for optimal stability.
- Gait analysis aids in diagnosing and managing neuromuscular and musculoskeletal disorders.
- Tendon/ligament failure mechanisms (e.g., ACL) are key to understanding sports injuries.
- Ergonomics applies biomechanics to prevent work-related musculoskeletal disorders (WMSDs).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

