Introduction & Agent - The Black Death 2.0
- Causative Agent: Yersinia pestis
- Gram-negative, non-motile coccobacillus.
- Characteristic bipolar "safety-pin" appearance with Wayson or Giemsa stain.
- Facultative anaerobe, facultative intracellular pathogen.
- Historical Impact: Responsible for devastating pandemics, notably the "Black Death" (14th century).
- Bioterrorism Classification:
- CDC Category A agent: high priority.
- Reasons: Ease of aerosol dissemination, high mortality rates (especially pneumonic plague), public panic potential.
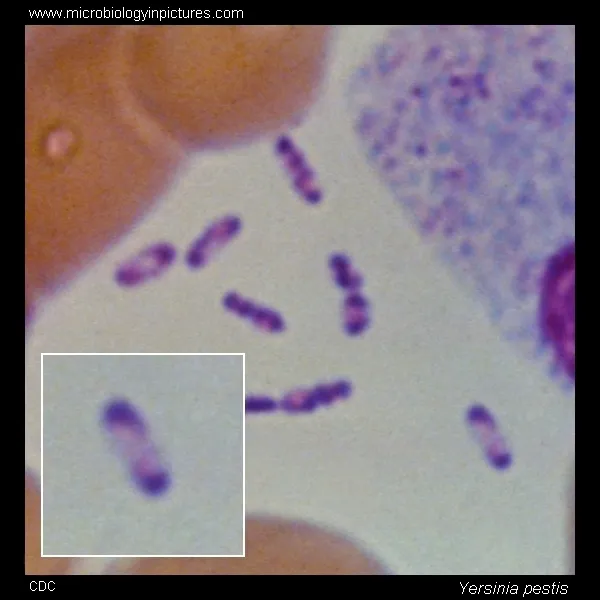
⭐ Yersinia pestis virulence factors include the F1 capsular antigen (antiphagocytic) and V/W antigens (disrupt host cell signaling).
Clinical Forms & Transmission - Lungs Under Siege
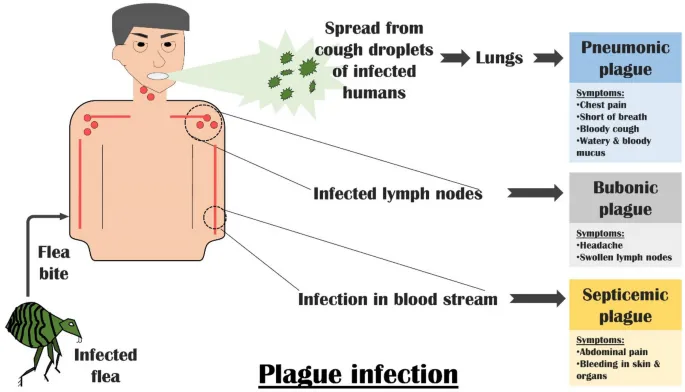
- Three Main Forms:
- Bubonic Plague: Most common natural form. Via flea bite. Results in painful, swollen lymph nodes (buboes). Low person-to-person transmission.
- Septicemic Plague: Yersinia pestis invades bloodstream. Can be primary or secondary. High mortality; may cause Disseminated Intravascular Coagulation (DIC).
- Pneumonic Plague: Lung infection. Primary concern for bioterrorism.
- Transmission: Inhalation of aerosolized bacteria (bioterrorism) or respiratory droplets from infected individuals.
- Incubation Period: 1-4 days.
- Symptoms: Acute fever, chills, cough with bloody sputum, dyspnea. Progresses rapidly.
- Highly contagious; high mortality if untreated.
⭐ Pneumonic plague is the most dangerous form in a bioterrorism scenario due to its direct person-to-person aerosol transmission and rapid progression.
Bioterrorism & Diagnosis - Spotting the Attack
-
Bioweapon Form: Aerosolized Y. pestis → primary pneumonic plague.
- Incubation: 1-6 days (aerosol: 1-3 days). Rapid progression.
-
Attack Indicators:
- Sudden cluster of severe febrile respiratory illness.
- Atypical demographics/season.
- No common travel/source.
-
Key Symptoms (Pneumonic):
- Fever, cough, dyspnea, hemoptysis.
- Sepsis, respiratory failure in 2-4 days.
-
Diagnosis:
- High suspicion in mass casualty event.
- CXR: bilateral infiltrates.
- Labs: Gram-negative coccobacilli (bipolar "safety pin" stain), culture (Y. pestis), PCR, F1 antigen.
⭐ Pneumonic plague is the most likely form in bioterrorism (aerosol) and is highly transmissible person-to-person.
Management & Prevention - Fighting Back Fast
- Treatment: Start antibiotics within 24h (pneumonic).
- Primary: Streptomycin (1g IM BD) or Gentamicin (5mg/kg/day).
- Alternatives: Doxycycline (100mg PO BD), Ciprofloxacin (500mg PO BD), Levofloxacin.
- Post-Exposure Prophylaxis (PEP):
- For close contacts (<2m pneumonic patient) or lab exposure.
- Duration: 7 days. Drugs: Doxycycline, Ciprofloxacin, Levofloxacin.
⭐ PEP for 7 days with Doxycycline or Ciprofloxacin is crucial for contacts of pneumonic plague.
- Infection Control & Prevention:
- Pneumonic: Strict respiratory (droplet) isolation for ≥48-72h post-antibiotics.
- Standard precautions for bubonic.
- Disinfection, vector (flea) & rodent control.
High‑Yield Points - ⚡ Biggest Takeaways
- Agent: Yersinia pestis, a Gram-negative coccobacillus with bipolar staining ("safety pin").
- Bioterrorism Threat: Aerosolized bacteria causing pneumonic plague is the primary concern.
- Pneumonic Plague: Presents with acute fever, bloody sputum (hemoptysis), dyspnea, and rapid shock.
- Key Diagnostic Feature: "Safety pin" appearance of Y. pestis on Wayson or Giemsa stain.
- Treatment of Choice: Aminoglycosides (Streptomycin, Gentamicin); alternatives include doxycycline, ciprofloxacin.
- Critical Timing: Treatment for pneumonic plague must start within 24 hours of symptom onset.
- Classification: A Category A bioterrorism agent due to high infectivity and mortality.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

