Bioterrorism Basics - Threat Unmasked
- Bioterrorism: Intentional release of biological agents (e.g., bacteria, viruses, toxins) to cause harm.
CDC agent categories: A, B, C.
| Cat. | Risk | Dissemination | Mortality | Examples | Feats. |
|---|---|---|---|---|---|
| A | Highest | Easy | High | 📌 Anthrax, Botulism, Plague, Smallpox, Tularemia, Viral Hemorrhagic Fevers (VHF) | Easily spread; high mortality; public panic; special action. |
| B | Moderate | Moderate | Low | Brucellosis, Q fever, Ricin toxin, Food/water safety threats (e.g., Salmonella, E. coli O157:H7) | Moderately spread; moderate illness, low death; enhanced surveillance. |
| C | Emerging | Potential | Potential | Nipah virus, Hantavirus, MDR-TB, Influenza (pandemic potential) | Emerging; potential high morbidity/mortality; availability. |
Alert Systems - Early Warning Radar
- Objective: Rapid detection & notification of unusual health events indicating potential bioterrorism.
- Key Components:
- Surveillance:
- Syndromic: Monitors pre-diagnostic data (e.g., symptom clusters like unexplained fever/rash, OTC sales).
- Epidemiological: Tracks confirmed disease cases; pattern recognition (Passive & Active).
- Event-based: Informal reports (media, community).
- Clinician Acuity: Frontline detection of atypical disease patterns or clusters.
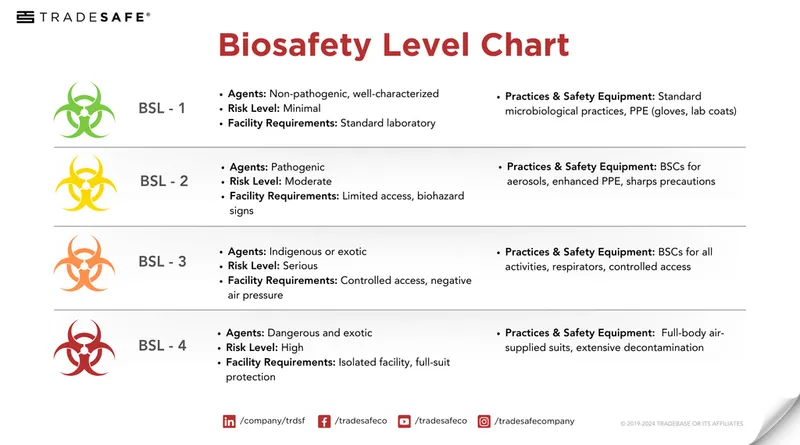
- Laboratory Confirmation: Network (District, State, NCDC) for agent ID. Requires BSL-3/4 for dangerous pathogens.
- Surveillance:
- Reporting Cascade (India - IDSP):
⭐ India's Integrated Disease Surveillance Programme (IDSP) is pivotal, using 'S', 'P', 'L' forms for reporting from sub-centres, facilities, and labs for rapid response.
Countermeasures - Shield & Sword

-
Prevention (Shield):
- Vaccination: Key for agents like Anthrax (e.g., Anthrax Vaccine Adsorbed - AVA), Smallpox (e.g., ACAM2000).
- Personal Protective Equipment (PPE): Crucial barrier; levels A, B, C, D based on risk.
- Level A: Highest protection (vapors, splashes, contact).
- Level D: Standard work uniform, minimal protection.
- Decontamination: For personnel, equipment, environment (e.g., soap & water, 0.5% hypochlorite solution).
-
Post-Exposure Management (Sword):
- Post-Exposure Prophylaxis (PEP):
Agent Preferred PEP Duration Anthrax Ciprofloxacin 500mg BD or Doxycycline 100mg BD 60 days Plague Doxycycline 100mg BD or Ciprofloxacin 500mg BD 7 days Tularemia Doxycycline 100mg BD or Ciprofloxacin 500mg BD 14 days - Isolation & Quarantine:
- Isolation: Separates symptomatic individuals.
- Quarantine: Restricts movement of asymptomatic exposed individuals.
- Supportive Care: Essential for managing clinical manifestations.
- Post-Exposure Prophylaxis (PEP):
⭐ Ring vaccination, vaccinating contacts of confirmed cases and their contacts, is a key strategy for smallpox containment and eradication efforts worldwide.
Response & Control - Damage Limitation
- Core Goals: Rapid containment, ↓morbidity/mortality, protect responders & infrastructure.
- Key Actions:
- Detection & Assessment: Enhanced surveillance (IDSP), rapid lab confirmation, epidemiological investigation.
- Patient Care & Infection Control:
- Decontamination (skin, environment).
- Isolation (source control) & cohorting.
- Medical countermeasures (antibiotics, antitoxins).
- Strict infection control (standard & transmission-based precautions).
- Public Health Measures:
- Contact tracing & quarantine.
- Mass prophylaxis/vaccination.
- Risk communication: clear, timely updates.
- Hospital Preparedness:
- Emergency plans: designated zones (Hot, Warm, Cold).
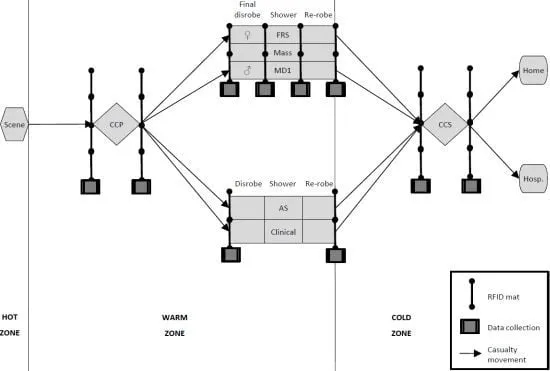
- Surge capacity (staff, beds, resources).
- Stockpiles: PPE, drugs, decontamination agents.
- Emergency plans: designated zones (Hot, Warm, Cold).
⭐ The National Disaster Management Authority (NDMA) and National Centre for Disease Control (NCDC) are key agencies in India's bioterrorism response framework.
High‑Yield Points - ⚡ Biggest Takeaways
- Robust surveillance & early warning are critical for timely response.
- Rapid lab identification of bioterror agents is essential.
- Strategic stockpiling of vaccines, antitoxins, antimicrobials is key.
- Effective inter-agency coordination & clear communication are vital.
- Decontamination & patient isolation strategies must be in place.
- Continuous training for HCWs & first responders is mandatory.
- Public health preparedness plans need regular drills & updates.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

