MEN Overview - Syndrome Spotlight
⭐ Most MEN syndromes (MEN1, MEN2A, MEN2B) are inherited in an autosomal dominant pattern.
- Group of genetic disorders predisposing to tumors in ≥2 endocrine glands.
- Key syndromes: MEN1, MEN2A, MEN2B, and MEN4.
- Arise from specific germline mutations (e.g., MEN1, RET).
- Characterized by high penetrance but variable expressivity.
- Lifelong surveillance and early intervention are crucial.
- Genetic counseling and family screening are vital.
MEN 1 - Wermer's 3P Party
Autosomal dominant; MEN1 gene (menin) mutation. 📌 MEN1 = 3Ps.
- Parathyroid ( >90%): Hyperplasia/adenoma.
- Leads to hypercalcemia, nephrolithiasis, bone issues.
- Pancreatic NETs (40-70%):
- Gastrinoma (ZES), Insulinoma, VIPoma, Glucagonoma.
- Pituitary Adenoma (30-40%):
- Prolactinoma (most common), GH-oma, ACTH-oma.
Other tumors: Carcinoid (thymic, bronchial), adrenal cortical, lipomas, angiofibromas.

- Prolactinoma (most common), GH-oma, ACTH-oma.
Other tumors: Carcinoid (thymic, bronchial), adrenal cortical, lipomas, angiofibromas.
⭐ Primary hyperparathyroidism is the most common (>90%) and often the first clinical manifestation of MEN1.
MEN 2A - Sipple's MPT Trio
- Autosomal dominant; RET proto-oncogene mutation (codon 634 commonest).
- 📌 Mnemonic: MPH (Medullary thyroid ca, Pheochromocytoma, Hyperparathyroidism).
- Key Features:
- Medullary Thyroid Carcinoma (MTC): ~100% penetrance.
- Pheochromocytoma: Often bilateral; screen with plasma metanephrines.
- Hyperparathyroidism: Parathyroid hyperplasia; ↑Ca, ↑PTH.
- Screening: Annual calcitonin, metanephrines, serum calcium.
- Management: Prophylactic thyroidectomy (by age 5-6 years).
⭐ Nearly 100% of untreated MEN2A individuals develop medullary thyroid carcinoma (MTC); prophylactic thyroidectomy is crucial.

MEN 2B - Gorlin's Neuroma Gang
- Autosomal dominant; RET proto-oncogene mutation (codon 918).
- 📌 MEN2B = Medullary thyroid ca, Marfanoid/ Mucosal neuromas, Pheochromocytoma.
- Features:
- Medullary Thyroid Carcinoma (MTC): 100% penetrant, aggressive, early onset.
- Pheochromocytoma: ~50%, often bilateral.
- Mucosal Neuromas: Lips, tongue, eyelids.
- Marfanoid Habitus: Tall, slim, high arched palate.
- Intestinal ganglioneuromatosis.
- No hyperparathyroidism (unlike MEN 2A).
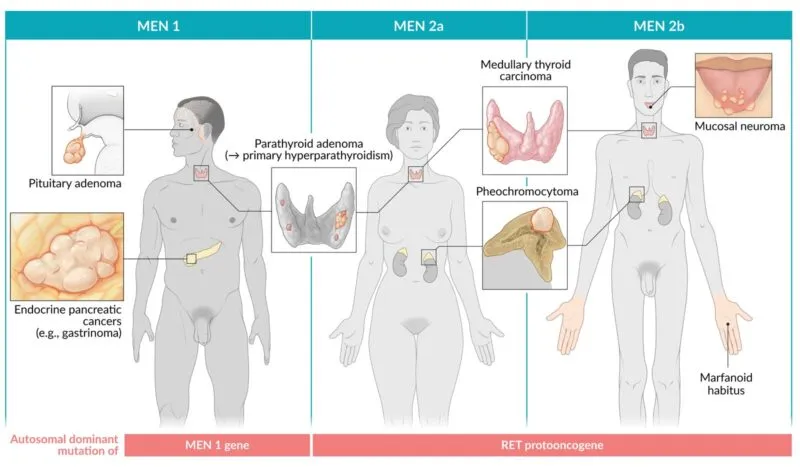
⭐ MEN2B is characterized by a very early onset and aggressive MTC; prophylactic thyroidectomy is often recommended within the first year of life.
MEN 4 & Genetics - Code & Counsel
- MEN 4:
- Gene: CDKN1B (p27Kip1, cell cycle inhibitor).
- Features: Pituitary adenomas, parathyroid tumors, NETs (pancreatic, GEP), adrenal, renal. Often MEN1-like.
⭐ MEN4 is a rare syndrome associated with mutations in the CDKN1B gene, and often involves pituitary and parathyroid tumors.
- Genetic Strategy (All MEN):
- Testing: If clinical suspicion or +ve family history.
- Counseling: Pre/post-test; discuss penetrance, surveillance, prophylactic options, family implications.
High‑Yield Points - ⚡ Biggest Takeaways
- MEN 1: Parathyroid, Pancreatic (e.g., gastrinoma), Pituitary tumors. MEN1 gene mutation.
- MEN 2A: Medullary Thyroid Cancer (MTC), Pheochromocytoma, Parathyroid hyperplasia. RET gene mutation.
- MEN 2B: MTC, Pheochromocytoma, Mucosal neuromas, Marfanoid habitus. RET gene mutation.
- MTC is common to MEN 2A/2B; screen for RET mutations.
- Always screen for Pheochromocytoma in MEN 2 before thyroid/parathyroid surgery.
- Calcitonin is the tumor marker for MTC.
- Primary hyperparathyroidism is most common in MEN 1.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

