AFS: Pathophysiology - Fungal Fiesta Fright
- Nature: Allergic reaction to extramucosal fungi; non-invasive.
- Hypersensitivity:
- Predominantly Type I (IgE-mediated) against fungal antigens.
- Possible Type III (immune complex) involvement.
- Causative Fungi: Primarily dematiaceous molds (e.g., Bipolaris, Curvularia, Alternaria).
- Host Factor: Atopic individuals (history of allergy, asthma).
- Key Pathological Features:
- Allergic Mucin: Thick, eosinophilic, "peanut butter-like" consistency.
- Contains fungal hyphae (no tissue invasion), numerous eosinophils, Charcot-Leyden crystals.
- Chronic inflammation causes sinus expansion.

- Allergic Mucin: Thick, eosinophilic, "peanut butter-like" consistency.
⭐ AFS is a non-invasive fungal sinusitis driven by a Type I hypersensitivity reaction to extramucosal fungi, not tissue invasion.
AFS: Clinical Features - Sinus Siege Symptoms
- Chronic Sinusitis Symptoms:
- Nasal blockage, persistent congestion.
- Thick, discolored discharge (often unilateral).
- Facial pain/pressure, headache.
- ↓ Sense of smell (hyposmia/anosmia).
- Nasal Polyposis: Frequently seen, can be extensive.
- Allergic Mucin: Hallmark finding!
- Thick, tenacious, "peanut butter" or "machine grease" consistency.
- Greenish-black to brown.
- History of atopy (asthma, eczema, allergic rhinitis).
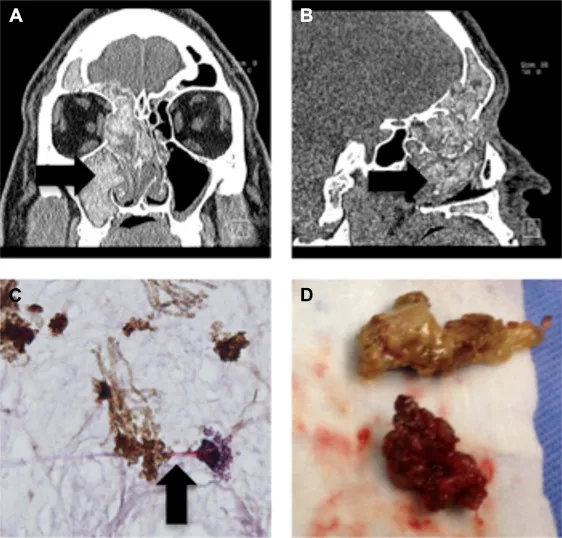
⭐ Key presentation: chronic rhinosinusitis, nasal polyposis, and thick, tenacious, 'peanut butter-like' eosinophilic mucin.
AFS: Diagnosis - Spotting Spores Sleuth
- Nasal Endoscopy:
- Reveals thick, tenacious, eosinophilic mucin (classic "peanut butter" or "machine oil" appearance).
- Imaging:
- CT Scan (PNS):
- Sinus opacification.
- Central hyperattenuation (pathognomonic).
- Bony erosion/remodeling (no frank invasion).

- MRI:
- T1: Hypointense.
- T2: Markedly hypointense (signal void).
- CT Scan (PNS):
- Histopathology (HPE) of Mucin:
- Allergic mucin: Abundant eosinophils, Charcot-Leyden crystals.
- Fungal hyphae (non-invasive); positive fungal stain.
- Allergy Testing:
- ↑ Total IgE & fungal-specific IgE.
- Positive skin prick test to fungal allergens.
- Bent & Kuhn Diagnostic Criteria (Key):
- Type I hypersensitivity (skin test or serology).
- Nasal polyposis.
- Characteristic CT findings.
- Eosinophilic mucin with fungal hyphae (no tissue invasion).
- Positive fungal stain or culture of sinus contents.
⭐ CT scans distinctively show central hyperattenuation in opacified sinuses; histopathology reveals allergic mucin with fungal hyphae and Charcot-Leyden crystals without tissue invasion. Bent and Kuhn criteria are key for diagnosis.
AFS: Management - Fungus Fight Formula
⭐ Management cornerstone: surgical debridement (FESS) followed by long-term corticosteroids (systemic/topical); role of antifungals is debated.
- Goals: Eradicate fungus, ↓ inflammation, ventilate sinuses, prevent recurrence.
- Surgical: FESS (Functional Endoscopic Sinus Surgery)
- Essential: Remove all allergic mucin & thick fungal debris.
- Aim: Patent sinuses for drainage & topical drug delivery.
- Medical (Post-FESS):
- Corticosteroids: Mainstay.
- Systemic (Oral Prednisolone): Initial (e.g., 0.5-1 mg/kg/day), slow taper over weeks/months.
- Topical (Nasal sprays): Long-term daily use for maintenance & recurrence prevention.
- Nasal Saline Irrigation: Daily, high-volume; clears secretions.
- Adjunctive Therapies (Consider):
- Antifungals: Controversial. Systemic (e.g., Itraconazole) not routine. Topical may be an option.
- Immunotherapy (allergen-specific): For atopy, may ↓ recurrence.
- Corticosteroids: Mainstay.
- Follow-up: Regular endoscopic surveillance crucial for recurrence.

High‑Yield Points - ⚡ Biggest Takeaways
- AFS is a Type I hypersensitivity reaction to fungal antigens in immunocompetent, often atopic individuals.
- Characterized by nasal polyposis and allergic mucin (thick, tenacious, eosinophilic, with fungal hyphae).
- Allergic mucin contains Charcot-Leyden crystals and numerous eosinophils; fungi are non-invasive.
- CT scans typically reveal hyperattenuation (hyperdensity) within affected sinuses; bony erosion can occur.
- Diagnosis is guided by the Bent and Kuhn criteria.
- Management primarily involves surgical debridement (FESS) followed by corticosteroids (systemic and topical).
- Recurrence is common, necessitating long-term follow-up and management strategies for optimal outcomes.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

