Pediatric Trauma Anesthesia: Unique Physiology - Tiny Titans, Big Challenges
- Airway: Obligate nose breathers (infants); large occiput (shoulder roll needed); anterior/cephalad larynx; narrowest at cricoid (infants).
- Respiratory: High O₂ consumption (6-8 mL/kg/min); low FRC (rapid desaturation); diaphragmatic breathing, fatigue-prone.
- Cardiovascular: CO primarily HR-dependent. Blood volume: Neonates $\approx \textbf{80-90}$ mL/kg, Children $\approx \textbf{70-80}$ mL/kg.
- ⭐ > Hypotension is a LATE, ominous shock sign. Resuscitate on poor perfusion signs (tachycardia, ↓cap refill), not just BP.
- Thermoregulation: Large surface area-to-volume ratio → ↑ heat loss, high hypothermia risk.
- Drug Metabolism: Immature hepatic/renal function → altered drug pharmacokinetics/dynamics; prolonged effects.

Pediatric Trauma Anesthesia: Resuscitation Essentials - ABCs & Fluid Fixes
Pediatric ATLS: ABCDE approach, age-specific modifications.
- Airway & C-spine: Secure, immobilize.
- Breathing: Assess, ventilate.
- Circulation: Control hemorrhage, assess perfusion.
- Vascular Access: IV attempts; rapid IO if IV fails (<60-90s). Sites: proximal tibia, distal femur.
- 📌 Broselow-Luten tape for drug/equipment sizing.
- Fluid Resuscitation: Initial crystalloid $20 \text{ mL/kg}$ (repeat up to $40-60 \text{ mL/kg}$).
- Blood Products (ongoing shock):
Product Dose (mL/kg) Key Indication PRBCs 10-15 ↑ O₂ capacity, Hb <7-8 g/dL FFP 10-15 Coagulopathy, MTP Platelets 5-10 (or 1U/10kg) Thrombocytopenia <50k, bleeding - MTP: Aim 1:1:1 (PRBCs:FFP:Platelets).
- Disability: AVPU, GCS.
- Exposure: Prevent hypothermia.
⭐ For children in hemorrhagic shock, after initial crystalloid boluses, early administration of blood products in a balanced ratio (e.g., 1:1:1 of PRBCs:FFP:Platelets) is crucial and improves outcomes.
Pediatric Trauma Anesthesia: Airway & Anesthesia - Breathing Easy, Sleeping Safe
- Airway Assessment:
- Pediatric anatomy: Large occiput/tongue, anterior/cephalad larynx, narrow cricoid.
- Adapt LEMON score.
- Equipment:
- Blades: Miller (straight) for infants.
- ETT (cuffed preferred): Uncuffed: $(\text{age in years}/4) + 4$; Cuffed: $(\text{age in years}/4) + 3.5$.
- LMA as rescue.
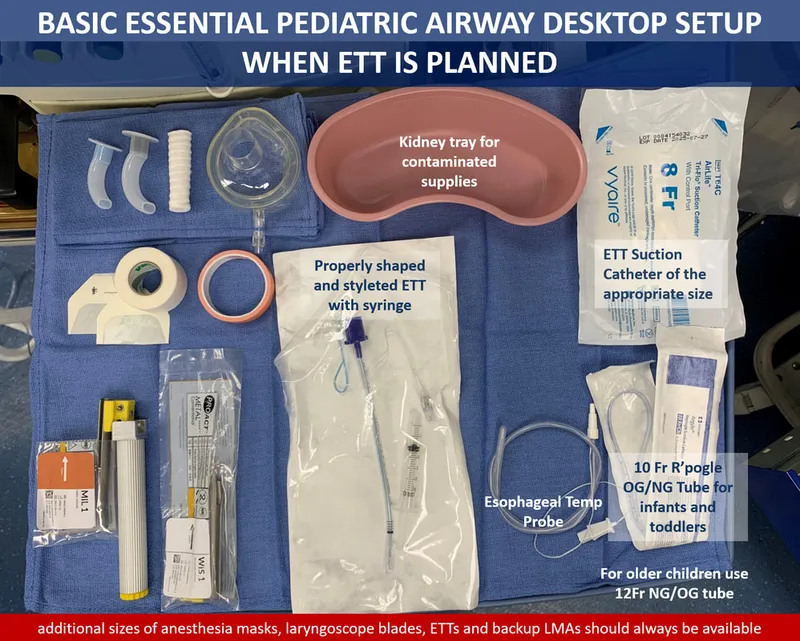
- Rapid Sequence Intubation (RSI):
- Preoxygenate; cricoid pressure.
- Drugs (age/weight-based):
- Atropine: 0.02 mg/kg (<1yr or <5yr with SCh).
- Induction: Ketamine 1-2 mg/kg IV; Etomidate 0.2-0.3 mg/kg IV.
- Paralysis: SCh (Infants 1-2 mg/kg IV, Child 1 mg/kg IV); Roc 0.9-1.2 mg/kg IV.
- Anesthesia:
- Agents: Ketamine, Propofol; Sevoflurane. Avoid N2O.
- Monitoring: ECG, SpO2, EtCO2 (key), NIBP, Temp.
- 📌 DOPE: Dislodgement, Obstruction, Pneumothorax, Equipment.
⭐ Atropine (0.02 mg/kg) for infants (<1yr) & children <5yr with SCh prevents bradycardia in RSI.
Pediatric Trauma Anesthesia: Key Injuries & Pain - Ouchie Fixers, Big Hurts
- TBI: Avoid hypotension/hypoxia; maintain CPP; GCS assessment crucial.
- Thoracic Trauma: Tension pneumothorax (needle decompression); chest tube for hemothorax/pneumothorax.
- Abdominal Trauma: FAST scan utility for diagnosis; consider non-operative management.
- Burns: Airway priority; Parkland formula for fluid resuscitation: $4 \text{ mL} \times \text{Body Weight (kg)} \times % \text{TBSA burned}$; aggressive temperature control.

- Pain Assessment: Use age-appropriate scales: FLACC, Wong-Baker FACES, Numeric Rating Scale.
- Multimodal Analgesia: Opioids (careful titration); regional (caudal/epidural, PNBs); non-opioids (paracetamol, ketamine).
⭐ The 'lethal triad' (hypothermia, acidosis, coagulopathy) is particularly detrimental in pediatric patients and requires aggressive preventative and corrective measures.
High‑Yield Points - ⚡ Biggest Takeaways
- Airway management is paramount; cuffed ETTs preferred for aspiration protection.
- Aggressively prevent/treat hypothermia to avoid coagulopathy and acidosis.
- Fluid resuscitation: initial 20 ml/kg crystalloid, then 10-15 ml/kg PRBCs for hemorrhage.
- Permissive hypotension is generally contraindicated in pediatric TBI.
- Employ multimodal analgesia; titrate opioids cautiously.
- Maintain C-spine immobilization until injury is ruled out.
- Crucial: age-specific physiology, vitals, drug doses, and equipment_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

