Chronic Pain: Definitions & Pathophysiology - Pain's Lingering Shadow
- Definition: Pain persisting > 3 months or beyond normal tissue healing time.
- Classification:
- Nociceptive: Actual or threatened tissue damage (somatic, visceral).
- Neuropathic: Lesion/disease of somatosensory nervous system.
- Nociplastic: Altered nociception without clear evidence of tissue damage or nervous system lesion (e.g., fibromyalgia).
- Core Pathophysiology:
- Peripheral Sensitization: ↑ responsiveness, ↓ threshold of nociceptors.
- Central Sensitization: CNS hyperexcitability (e.g., wind-up, LTP). Results in allodynia, hyperalgesia.
- Impaired Descending Modulation: Reduced endogenous analgesia.
- Neuroplasticity: Maladaptive structural/functional CNS changes.
⭐ Central sensitization (e.g., NMDA receptor activation, glial cell involvement) is key in the transition from acute to chronic pain and underlies conditions like fibromyalgia, causing allodynia/hyperalgesia.
Neuropathic Pain Syndromes - Zaps, Zings, & Zingers
- Lesion/disease of somatosensory system. Features: burning, shooting, electric shocks ("zaps, zings, zingers"), paresthesia. Allodynia & hyperalgesia common.
- Key Examples:
- Diabetic Neuropathy (DN): Common. Symmetrical, "stocking-glove" pattern. Painful/numb.
- Post-Herpetic Neuralgia (PHN): Pain ≥3 months post-zoster in dermatome. Burning, electric.
⭐ Early antiviral therapy (e.g., Acyclovir, Valacyclovir within 72 hrs of zoster onset) can ↓ PHN incidence & severity.
- Trigeminal Neuralgia (TN): "Tic Douloureux". Sudden, severe, unilateral CN V facial pain. Electric shocks, trigger points.
- Central Pain: Post-stroke, Spinal Cord Injury (SCI), Multiple Sclerosis (MS). Diffuse, often refractory.
- Pharmacotherapy Pillars:
- Anticonvulsants (1st line): Gabapentin, Pregabalin.
- Antidepressants: TCAs (Amitriptyline), SNRIs (Duloxetine).
- Topical: Lidocaine patches, Capsaicin cream.

Musculoskeletal & Specific Syndromes - Deep Ache Dilemmas
- Fibromyalgia (FM):
- Widespread pain > 3 months, fatigue, sleep issues, "fibro fog".
- Dx: Widespread Pain Index (WPI) & Symptom Severity (SS) score. ACR 2016: Pain in 4/5 regions.
- Rx: Education, exercise, CBT. TCAs (amitriptyline), SNRIs (duloxetine), pregabalin.
- Chronic Low Back Pain (CLBP):
- Pain > 3 months. Mostly non-specific.
- ⚠️ Red flags: Neuro deficits, cauda equina, cancer Hx, fever, trauma.
- Rx: Stay active, PT. NSAIDs (short-term). TCAs, duloxetine.
- Complex Regional Pain Syndrome (CRPS):
- Severe pain, sensory (allodynia), vasomotor (temp/color), sudomotor/edema, motor/trophic changes. Disproportionate to injury.
- Budapest criteria. Type I (no nerve lesion), Type II (nerve lesion).
- Rx: Early PT/OT. Gabapentinoids, TCAs, bisphosphonates. Sympathetic blocks.
⭐ CRPS often triggered by minor trauma, especially to distal limbs (e.g., wrist fracture).

Chronic Pain Management Approaches - The Relief Roadmap
- Goal: Improve function & quality of life via multimodal approach.
- Pharmacological Strategy:
- WHO Ladder (Adapted):
- Step 1: Non-opioids (Paracetamol, NSAIDs).
- Step 2: Weak opioids (e.g., Tramadol) ± non-opioids ± adjuvants.
- Step 3: Strong opioids (e.g., Morphine, Buprenorphine) ± non-opioids ± adjuvants.
- Key Adjuvants:
- Anticonvulsants: Gabapentin, Pregabalin (neuropathic pain).
- Antidepressants: TCAs (Amitriptyline), SNRIs (Duloxetine).
- Topical: Lidocaine patches, Capsaicin cream.
- WHO Ladder (Adapted):
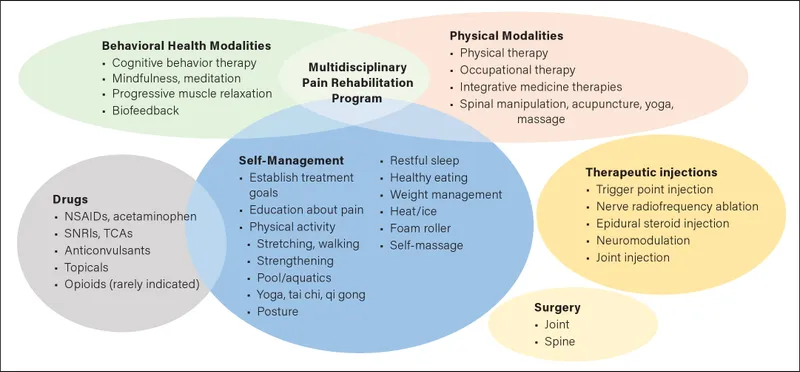
- Non-Pharmacological Pillars (📌 Physical, Psychological, Interventional - PPI):
- Physical therapies: Exercise, TENS, physiotherapy.
- Psychological support: CBT, mindfulness, ACT.
- Interventional techniques: Nerve blocks, RFA, SCS (refractory cases).
⭐ Amitriptyline, a TCA, is highly effective for neuropathic pain, fibromyalgia, and chronic headaches, often used at lower doses (e.g., 10-25 mg nightly) than for depression.
High‑Yield Points - ⚡ Biggest Takeaways
- CRPS: Type I (no nerve injury), Type II (nerve injury). Budapest criteria for diagnosis.
- Fibromyalgia: Widespread pain, tender points, fatigue. Key drugs: amitriptyline, pregabalin.
- Trigeminal Neuralgia: Lancinating facial pain (V2/V3). Carbamazepine is first-line.
- Post-Herpetic Neuralgia: Pain >3 months post-zoster. Treat with gabapentinoids, TCAs.
- Phantom Limb Pain: Pain in amputated limb. Mirror therapy, gabapentinoids used.
- Central Sensitization: Key mechanism causing allodynia, hyperalgesia in chronic pain_
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

