Anaphylaxis & Allergic Rxns - Defining Danger
- Anaphylaxis: A severe, potentially life-threatening, systemic hypersensitivity reaction. Characterized by rapid onset.
- Allergic Reaction: An exaggerated immune response to a typically harmless substance (allergen).
- Hypersensitivity Focus:
- Type I (IgE-mediated): Most common in perioperative anaphylaxis. Involves mast cell and basophil degranulation releasing histamine and other mediators.
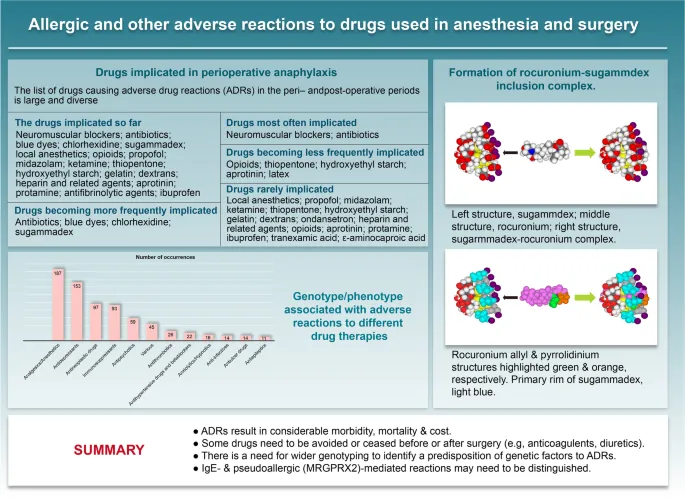
- Common Perioperative Triggers:
- Neuromuscular Blocking Agents (NMBAs): e.g., Rocuronium, Suxamethonium.
- Antibiotics: Especially β-lactams (penicillins, cephalosporins).
- Latex: Gloves, catheters.
- Chlorhexidine: Antiseptic skin preparation.
- 📌 Mnemonic for Triggers: "Never Allow Lethal Complications" (NMBAs, Antibiotics, Latex, Chlorhexidine).
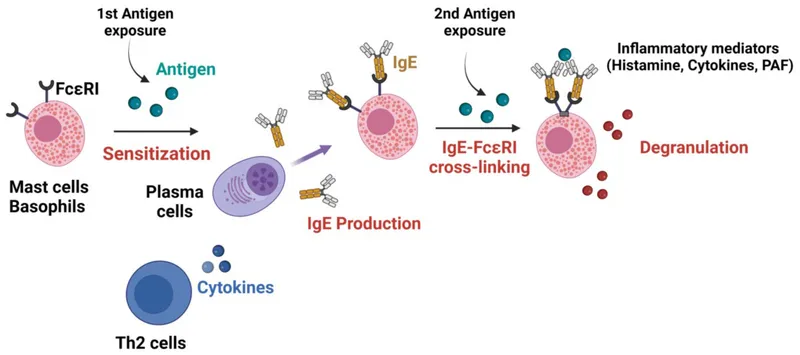
⭐ Neuromuscular blocking agents (NMBAs) are the most frequent cause of perioperative anaphylaxis.
Anaphylaxis & Allergic Rxns - Cascade Catastrophe
- Mechanisms:
- IgE-mediated (Allergic): Type I hypersensitivity. Allergen cross-links IgE on mast cells/basophils → degranulation.
- Non-IgE mediated (Anaphylactoid): Direct mast cell/basophil degranulation (e.g., opioids, NMBAs, contrast media).
- Key Mediators Released:
- Histamine, tryptase (specific mast cell marker), leukotrienes ($LTC_4$, $LTD_4$), prostaglandins ($PGD_2$).
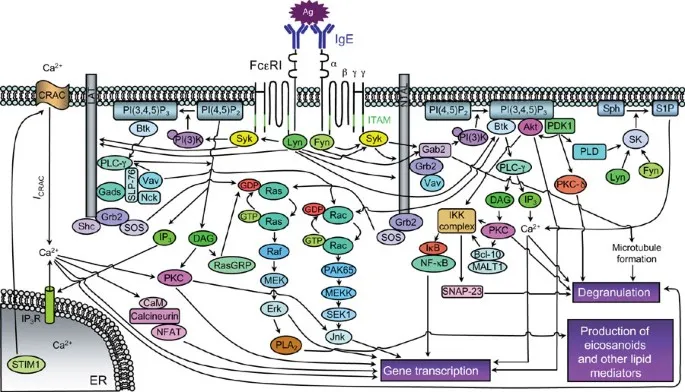
- Histamine, tryptase (specific mast cell marker), leukotrienes ($LTC_4$, $LTD_4$), prostaglandins ($PGD_2$).
- Clinical Features (Systemic):
- Cutaneous (Most common): Urticaria, angioedema, flushing, pruritus.
- Respiratory: Bronchospasm, laryngeal edema, dyspnea, cough, wheeze.
- Cardiovascular: Hypotension, tachycardia (can be bradycardia), arrhythmias, collapse.
- GI: Nausea, vomiting, diarrhea, abdominal cramps.
⭐ Cardiovascular collapse can be the first and only sign of anaphylaxis under general anesthesia, especially in anesthetized patients.
- Severity Grading (Ring & Messmer):
Anaphylaxis & Allergic Rxns - Action Stations!
- Clinical Dx: Rapid hypotension, bronchospasm, urticaria, angioedema.
- DDx: High spinal, vasovagal, MI, PE.
- Labs: Serum tryptase (sample 0.5-2h post-onset; normal <11.4 ng/mL).
- Immediate Management:
- Call for help! Stop trigger.
- ABCDE approach:
- Airway: Secure.
- Breathing: 100% O2.
- Circulation: IV fluids (Crystalloids 1-2L).
- Drugs (see below). Exposure.
- Pharmacotherapy: 📌 Epinephrine First!
- Epinephrine: IM 0.3-0.5mg (1:1000). Repeat 5-15 min.
- Refractory: IV Epi infusion 0.05-0.1 mcg/kg/min or slow IV bolus 5-20 mcg.
- Antihistamines: H1 (Diphenhydramine 25-50mg IV) + H2 (Ranitidine 50mg IV).
- Corticosteroids: Hydrocortisone 100-200mg IV.
- Bronchodilators.
- Epinephrine: IM 0.3-0.5mg (1:1000). Repeat 5-15 min.
⭐ Serum tryptase: key diagnostic marker, peaks 1-2h post-onset; more specific than histamine.
Anaphylaxis & Allergic Rxns - Prevent & Protect
- Post-Acute Management & Documentation:
- Observe for 6-12 hours (biphasic reaction risk).
- Detailed documentation: suspected agents, timeline, vitals, treatment, response.
- Allergy Referral:
- Indications: All suspected perioperative anaphylaxis cases.
- Timing: Crucial for accurate testing.
⭐ Skin testing should ideally be performed 4-6 weeks after the anaphylactic event to allow IgE levels to normalize and avoid false negatives.
- Investigations:
- Skin Prick Tests (SPT): Initial screen.
- Intradermal Tests (IDT): More sensitive if SPT negative.
- Specific IgE assays (e.g., RAST): Blood test for specific allergens.
- Basophil Activation Test (BAT): Cellular test, useful in select cases.
- Prevention Strategies (Known/High-Risk):
- Strict avoidance of confirmed allergens.
- Premedication: Limited evidence; consider for radiocontrast media (corticosteroids, antihistamines).
- Clear communication: Allergy bracelets, updated medical records, alert systems.
High‑Yield Points - ⚡ Biggest Takeaways
- NMBAs are the most common triggers for perioperative anaphylaxis.
- Reactions: IgE-mediated (true anaphylaxis) or non-IgE mediated (anaphylactoid).
- Key signs: sudden hypotension, bronchospasm, tachycardia, skin manifestations.
- Management: Stop agent, 100% O2, epinephrine (critical), IV fluids.
- Epinephrine is life-saving; use IV boluses (e.g., 10-100 mcg), consider infusion.
- Serum tryptase (peaks 1-2 hrs) confirms mast cell degranulation.
- Prior allergy, atopy, or multiple surgeries increase risk.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

