Rapid Sequence Induction - Why, When, Wow!
- Why perform RSI? For rapid airway control, crucially preventing pulmonary aspiration in high-risk patients.
⭐ Primary goal of RSI is to minimize the risk of pulmonary aspiration in patients with a full stomach.
- Key Indications:
- Emergency surgery.
- Full stomach (e.g., trauma, pregnancy, bowel obstruction, GERD, uncontrolled diabetes).
- Key Goals/Features:
- Achieve swift, definitive airway.
- Minimize time to intubation.
- Avoid Bag-Mask Ventilation (BMV) pre-intubation to limit gastric insufflation.

Rapid Sequence Induction - Breathe Easy Now
- Aim: Rapid airway control, ↓ aspiration risk (full stomach, emergency).
- Core Sequence:
- Preparation: Check equipment, drugs (e.g., Propofol, Suxamethonium/Rocuronium), suction.
- Pre-oxygenation: 100% O₂ for 3-5 min.
⭐ Effective pre-oxygenation with 100% O₂ for 3-5 minutes can provide an apneic window of up to 8 minutes in a healthy adult.
- Induction & Paralysis: Simultaneous IV push.
- Intubation: No/gentle Bag-Mask Ventilation (BMV) prior. Cricoid pressure (Sellick). Confirm placement.
Rapid Sequence Induction - The Knockout Crew
- Goal: Rapid unconsciousness & paralysis to secure airway, minimizing aspiration risk.
- Induction Agents (IV):
- Propofol: 1.5-2.5 mg/kg. Rapid onset, short duration. ↓BP, apnea.
- Etomidate: 0.2-0.3 mg/kg. Hemodynamically stable. Adrenal suppression. Myoclonus.
- Ketamine: 1-2 mg/kg. Sympathomimetic (↑HR, ↑BP). Analgesic. Emergence delirium.
- Neuromuscular Blocking Agents (NMBAs):
- Succinylcholine (SCh): 1-1.5 mg/kg. Depolarizing. Fastest onset (30-60s).
⭐ Succinylcholine, despite its side effects, remains the fastest onset NMBA, crucial for RSI, but contraindicated in severe burns after 24h and crush injuries due to hyperkalemia risk.
- Rocuronium: 0.6-1.2 mg/kg. Non-depolarizing. Longer onset (60-90s). Reversible with Sugammadex.
- Succinylcholine (SCh): 1-1.5 mg/kg. Depolarizing. Fastest onset (30-60s).
- 📌 P.L.S. (Please Let's Secure-airway): Preparation, Preoxygenation, Pretreatment, Paralysis with induction, Positioning, Placement of tube, Post-intubation management (not part of RSI itself but crucial follow-up).
Rapid Sequence Induction - The Swift Seven
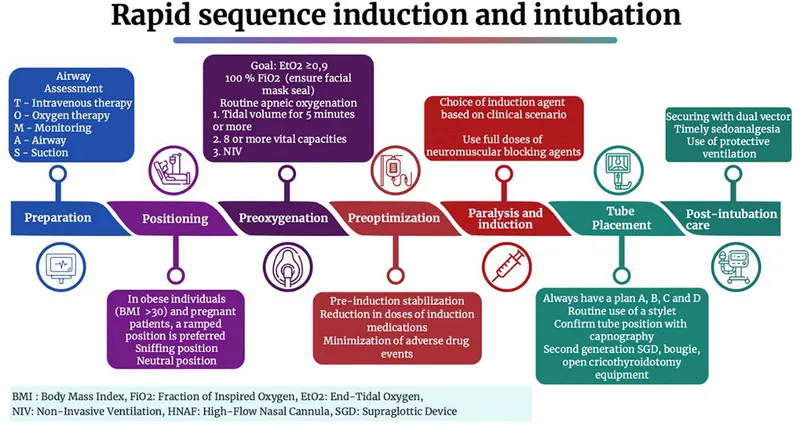
📌 The 7 P's of RSI:
- Preparation: Equipment, drugs, team ready.
- Preoxygenation: 100% O₂ for 3-5 min or 8 vital capacity breaths/60s. Target ETO₂ >90%.
- Pretreatment (Optional): Lidocaine, fentanyl, atropine (if indicated).
- Paralysis & Induction: Co-administer:
- Sedative: Propofol 1.5-2.5 mg/kg / Etomidate 0.2-0.3 mg/kg.
- NMB: Succinylcholine 1-1.5 mg/kg / Rocuronium 1-1.2 mg/kg.
- Protection & Positioning: Cricoid pressure (Sellick's), sniffing position.
⭐ Cricoid pressure (Sellick's maneuver) involves applying 10N of force before LOC and 30N after LOC, aimed at occluding the esophagus.
- Placement & Proof: Intubate. Confirm: ETCO₂, chest rise, auscultation.
- Post-intubation Management: Secure ETT, ventilate, post-intubation care.
Rapid Sequence Induction - Trouble Shooters' Guide
- Hypotension: IV fluids, vasopressors.
- Hypoxemia: ↑FiO2, optimize PEEP, airway maneuvers, LMA.
- Difficult Airway: Follow algorithm; VL, SGA, bougie, surgical kit.
- Aspiration: Cricoid pressure (Sellick’s), immediate suction, consider antibiotics.
- Laryngospasm: 100% O2, PPV, Larson's maneuver, suxamethonium ($0.1 \text{ mg/kg}$ IV).
- Bradycardia: Atropine ($0.02 \text{ mg/kg}$).
⭐ In a 'Can't Intubate, Can't Oxygenate' (CICO) scenario during RSI, progression to a surgical airway (e.g., cricothyroidotomy) must be rapid and decisive.
High‑Yield Points - ⚡ Biggest Takeaways
- RSI aims to rapidly secure the airway in full stomach patients, minimizing aspiration risk.
- Preoxygenation with 100% O2 for 3-5 minutes or 4 vital capacity breaths is crucial.
- Cricoid pressure (Sellick’s maneuver) at 30N is applied before loss of consciousness until cuff inflation.
- Common induction agents: Propofol; Etomidate for hemodynamic stability; Ketamine for bronchospasm/hypotension.
- Paralytics: Succinylcholine (gold standard, rapid onset/offset) or high-dose Rocuronium.
- Traditionally, no bag-mask ventilation (BMV) before intubation to prevent gastric insufflation and aspiration.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

