Introduction & Classification - Vessel Vandals Intro
- Vasculitis: Inflammation of blood vessel walls → vessel damage (stenosis, occlusion, aneurysm).
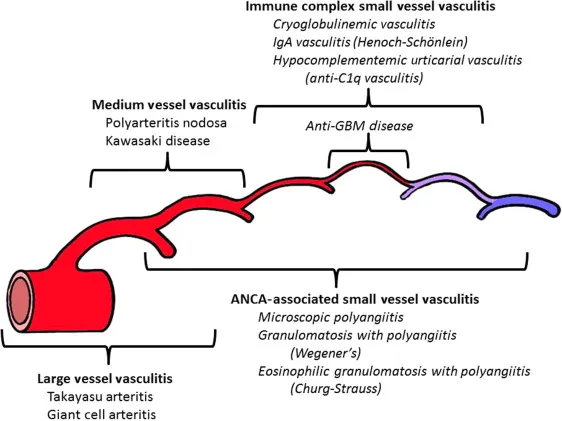
- Chapel Hill Consensus Conference (CHCC) 2012 Classification:
| Vessel Size | Vasculitis Type | Key Examples |
|---|---|---|
| Large | Large Vessel Vasculitis (LVV) | Giant Cell Arteritis (GCA; Age >50 yrs), Takayasu Arteritis (TA) 📌 'Giant Takayasu' |
| Medium | Medium Vessel Vasculitis (MVV) | Polyarteritis Nodosa (PAN), Kawasaki Disease (KD) |
| Small | Small Vessel Vasculitis (SVV) | ANCA-Associated (AAV): MPA, GPA, EGPA Immune Complex: IgA Vasculitis, Cryoglobulinemic Vasculitis |
⭐ Giant Cell Arteritis (GCA) is the most common systemic vasculitis in individuals aged >50 years in Western countries.
Pathophysiology & Etiology - Inflammation Ignition
- Immune Mechanisms: Vessel inflammation driven by:
- Type II (antibody-mediated cytotoxicity).
- Type III (immune complex deposition).
- Type IV (cell-mediated immunity).
- ANCA (Anti-Neutrophil Cytoplasmic Antibodies): Key in pauci-immune types.
- PR3-ANCA (c-ANCA): Targets Proteinase 3; associated with GPA.
- 📌 c-ANCA/PR3 ~ GPA ('C' for 'Ceiling' - affects upper respiratory/sinuses).
- MPO-ANCA (p-ANCA): Targets Myeloperoxidase; linked to MPA, EGPA.
- PR3-ANCA (c-ANCA): Targets Proteinase 3; associated with GPA.
- Common Triggers:
- Infections: HBV (PAN), HCV (cryoglobulinemia).
- Drugs: e.g., Hydralazine, Propylthiouracil.
- Malignancies.
⭐ PR3-ANCA (formerly c-ANCA) is highly specific for Granulomatosis with Polyangiitis (GPA).
Common Vasculitides - Rogues' Gallery
| Vasculitis Type | Vessel Size | Key Demographics | Clinical Hallmarks | Diagnostic Markers |
|---|---|---|---|---|
| GCA | Large | >50 yrs, F>M | Temporal headache, jaw claudication, visual loss, PMR | ESR >50, CRP ↑, Temporal artery biopsy (granuloma) |
| Takayasu Arteritis | Large | <40 yrs, Asian F | "Pulseless disease", claudication, BP discrepancy, aortic arch | ESR/CRP ↑, Angiography (MRA/CTA) |
| PAN | Medium | Mid-age, M>F, Hep B (10-30%) | Renal (no GN), HTN, skin (livedo), neuropathy, GI; spares lungs. 📌 "Beads on string" (angio) | pANCA neg, Biopsy (necrotizing), Angio (microaneurysms) |
| Kawasaki Disease | Medium | Children <5 yrs, Asian | 📌 CRASH & Burn (Conjunctivitis, Rash, Adenopathy, Strawberry tongue, Hand/foot) + Fever ≥5d. Coronary aneurysms. | Clinical, ESR/CRP ↑, Echo (coronary) |
| GPA (Wegener's) | Small | Adults (mean 40-55) | Triad: Upper/Lower resp. tract (sinusitis, nodules, hemoptysis), Kidneys (GN) | c-ANCA (PR3-ANCA) +, Biopsy (necrotizing granulomas) |
| IgA Vasculitis (HSP) | Small | Children (peak 4-6 yrs), post-URI | Tetrad: Palpable purpura, Arthritis, Abd pain, Renal (IgA nephropathy) | Clinical, Biopsy (skin/kidney): IgA deposition |
Management Principles - Dousing the Flames
Goals of Treatment:
- Induce remission rapidly.
- Maintain long-term remission.
- Prevent disease relapse and minimize organ damage.
General Therapeutic Arsenal:
- Corticosteroids: e.g., Prednisone (initial dose often 1 mg/kg/day).
- Immunosuppressants:
- Cyclophosphamide (CYC)
- Azathioprine (AZA)
- Methotrexate (MTX)
- Mycophenolate Mofetil (MMF)
- Rituximab (RTX)
Severe ANCA-Associated Vasculitis (AAV) Strategy:
- Induction: Typically Cyclophosphamide (CYC) or Rituximab (RTX) combined with high-dose corticosteroids.
⭐ Rituximab is increasingly used as an alternative to cyclophosphamide for induction of remission in severe ANCA-associated vasculitis, particularly in relapsing disease or if cyclophosphamide is contraindicated.
High‑Yield Points - ⚡ Biggest Takeaways
- Giant Cell Arteritis: Elderly (>50 yrs); temporal artery involvement; jaw claudication, visual loss; prompt steroids.
- Takayasu Arteritis: Young females; "Pulseless disease"; affects aortic arch & branches; discrepant BP.
- Buerger's Disease: Strongly linked to heavy smokers; affects distal extremity vessels; claudication, gangrene.
- Polyarteritis Nodosa (PAN): Affects medium arteries; Hepatitis B association; renal/mesenteric ischemia; spares lungs.
- Kawasaki Disease: Primarily in children; risk of coronary artery aneurysms; treat with IVIG & aspirin.
- GPA (Wegener's): c-ANCA positive; involves respiratory tract & kidneys; characterized by granulomas.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

