Hematuria 101 - Red Flag Rules
- Definition: >3 Red Blood Cells (RBCs) per High Power Field (HPF).
- Types:
- Microscopic: Asymptomatic, incidental finding.
- Macroscopic (Gross): Visible blood in urine.
- Initial Sort:
- Glomerular: Dysmorphic RBCs, RBC casts.
- Non-glomerular: Eumorphic RBCs, no casts.
- ⚠️ Red Flag Rules (Suspect Malignancy):
- Painless gross hematuria.
- Age >40 years.
- Smoking history.
- Occupational exposure (aniline dyes, benzenes).
- History of urologic disease/instrumentation.
- Persistent asymptomatic microscopic hematuria.
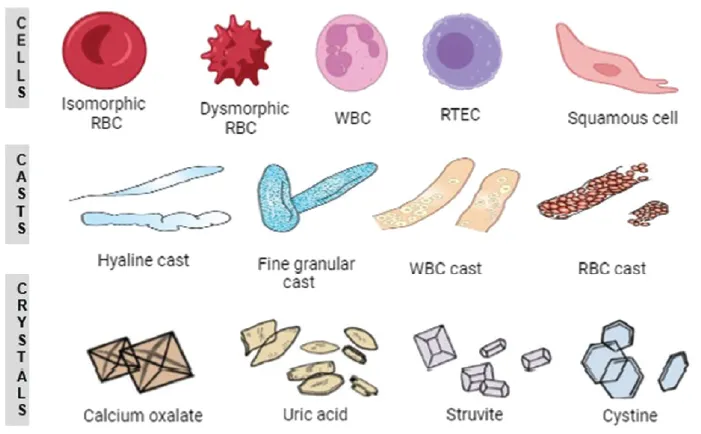
⭐ The presence of RBC casts in urine is pathognomonic for glomerular hematuria.
Etiology Maze - Source Sleuthing
- Glomerular (Nephrologic): Dysmorphic RBCs, RBC casts, proteinuria.
- IgA Nephropathy (Berger's)
- Post-Streptococcal GN (PSGN)
- Alport Syndrome
- Thin Basement Membrane Disease
- Lupus Nephritis
- Non-Glomerular (Renal):
- Neoplasms: Renal Cell Carcinoma (RCC)
- Infections: Pyelonephritis
- Stones (Nephrolithiasis)
- Polycystic Kidney Disease (PKD)
- Trauma, Vascular (AVM, infarct)
- Papillary Necrosis (DM, Sickle Cell, 📌 Analgesics)
- Urologic (Lower Tract):
- Bladder: UTI, Stones, TCC
- Prostate: BPH, Prostatitis, Cancer
- Urethra/Ureters: Stricture, Stones, Trauma, TCC
- Other Causes:
- Coagulopathy, Anticoagulants
- Vigorous exercise
- Drugs (e.g., Cyclophosphamide)
⭐ In adults > 40 years, painless gross hematuria is a strong indicator of malignancy (e.g., bladder cancer) and requires thorough investigation.
Clinical Detective - Clue Collection
- History is Key:
- Hematuria Type: Gross/Microscopic; Initial, Terminal, Total; Clots; Color (red vs. cola).
- Symptoms: Pain (flank, dysuria), Fever, Weight loss. Systemic (rash, joint pain).
- Risk Factors: Age >40, Smoking, Occupation (dyes), Meds (anticoagulants, cyclophosphamide 📌), Family Hx (cancer), URI, Trauma, Exercise.
⭐ A history of cyclophosphamide use is a significant risk factor for hemorrhagic cystitis and bladder cancer.
- Physical Exam Pointers:
- General: Pallor, Edema, Lymphadenopathy.
- Abdomen: Masses, CVA tenderness.
- GU: Meatal stenosis; DRE (prostate); Pelvic exam.
- BP: Hypertension.
Diagnostic Toolkit - Scope & Scan
- Imaging (Upper Tract):
- CT Urography (CTU): Multi-phasic (non-contrast, nephrographic, excretory).
⭐ CT Urography is the gold standard imaging for evaluating upper tract causes of hematuria, especially when malignancy is suspected.
- MR Urography (MRU): If CTU contraindicated (e.g., contrast allergy, pregnancy, radiation).
- Ultrasound (KUB): Initial, non-invasive; detects stones, hydronephrosis, large masses.
- CT Urography (CTU): Multi-phasic (non-contrast, nephrographic, excretory).
- Endoscopy:
- Cystoscopy: Mandatory for gross hematuria & high-risk microscopic hematuria.
- Direct visualization of bladder & urethra.
- Biopsy capability.
- Types: Flexible (outpatient), Rigid (OR). Enhanced: Blue light / NBI.
- Ureteroscopy (URS): If upper tract lesions suspected on imaging or for biopsy.
- Cystoscopy: Mandatory for gross hematuria & high-risk microscopic hematuria.
- Urine Cytology:
- Adjunct for high-risk patients to detect malignant cells. Not standalone.

High‑Yield Points - ⚡ Biggest Takeaways
- Painless gross hematuria in those >40 years strongly suggests urothelial cancer; mandates CT urogram & cystoscopy.
- Hematuria localization: Initial (urethral), terminal (bladder neck/prostatic), total (bladder/upper tract).
- Microscopic hematuria (≥3 RBCs/HPF on ≥2 occasions) or any gross hematuria needs full workup.
- Glomerular indicators: Dysmorphic RBCs, RBC casts, significant proteinuria point to renal origin.
- Gold standard evaluation: CT urogram for upper tracts, cystoscopy for lower tracts.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

