Lymphadenectomy Basics - Node Know-How
- Definition: Surgical removal of lymph nodes (LNs) for cancer staging & locoregional control.
- Purpose: Diagnose nodal metastasis, regional control, guide therapy, prognostication.
- Types:
- Sentinel LN Biopsy (SLNB): Biopsy of first draining LN(s); ↓morbidity. Uses dye/radioisotope (Tc-99m).
- Regional LN Dissection (RLND): Removal of regional LNs (axillary, cervical etc.).
- Radical: Complete removal.
- Modified Radical: Spares key structures.
- Selective: Specific LN levels.
- Nodal Yield: Min. LNs for staging (e.g., ≥12 CRC, ≥10 breast ALND).
- Skip Metastases: Mets bypassing proximal LNs.
⭐ SLN is the first LN draining a tumor; its status predicts regional node status (e.g., breast, melanoma).
Nodal Anatomy - Lymphatic Landscapes
- Lymphatic drainage follows venous system; vital for cancer staging & surgical approach.
- Sentinel Lymph Node (SLN): First node(s) draining a tumor. SLNB guides further nodal dissection.
- Key Nodal Basins:
- Axilla: Levels I-III relative to pectoralis minor. Rotter's nodes (interpectoral).
- Neck: Levels I-VII define anatomical compartments.
- Mediastinum: IASLC map (e.g., paratracheal, subcarinal, hilar).
- Stomach: Perigastric stations (JGCA classification).
- Pelvis/Groin: Iliac, obturator nodes. Groin: Cloquet's node (deep inguinal).
- Major Ducts: Thoracic duct (drains ~75% body lymph to left venous angle); Right lymphatic duct (right upper quadrant).

⭐ Virchow's node (left supraclavicular) classically signals metastatic gastric cancer (Troisier's sign).
Procedural Pointers - Cutting to Cure
- Goal: Achieve R0 resection (microscopically negative margins), accurate staging.
- Types:
- Sentinel Lymph Node Biopsy (SLNB): For clinically node-negative (cN0) patients.
- Regional LND: For positive SLN or cN+.
- Radical LND: Extensive, rare.
- SLNB Technique:
- Tracer: Tc-99m colloid + blue dye.
- Identify: Gamma probe & visual.
- Nerves (Axilla):
- Long thoracic (serratus ant.).
- Thoracodorsal (lat. dorsi).
- Intercostobrachial (medial arm sensation) - often cut.
- Complications: Lymphedema, seroma, nerve injury.
⭐ In breast cancer, if SLNB shows 1-2 positive nodes without extracapsular extension, patients undergoing breast-conserving surgery with whole breast radiation may not require completion ALND (AMAROS/ACOSOG Z0011 criteria).
Complications & Management - Navigating Node Nightmares
- Immediate/Early:
- Hemorrhage/Hematoma: Prompt surgical control.
- Nerve Injury: Meticulous dissection crucial.
- Examples: Spinal accessory (neck), long thoracic (axilla), recurrent laryngeal (thyroid/neck), obturator (pelvic).
- Management: Physiotherapy; rarely surgery.
- Lymphocele/Seroma: Observation, aspiration; sclerotherapy for persistence.
- Wound Infection: Antibiotics, drainage.
- Late:
- Lymphedema: Most common, debilitating.
- Prevention: Sentinel Lymph Node Biopsy (SLNB) over completion dissection where appropriate.
- Management: Complex Decongestive Therapy (CDT) - Manual Lymphatic Drainage (MLD), compression, exercises, skin care. 📌 DECS (Drainage, Exercise, Compression, Skin care)
- Surgical: Lymphaticovenous anastomosis (LVA), vascularized lymph node transfer (VLNT) for refractory cases.
- Chronic Pain/Paresthesia: Multimodal analgesia, physiotherapy.
- Functional Deficits (e.g., shoulder stiffness): Early physiotherapy.
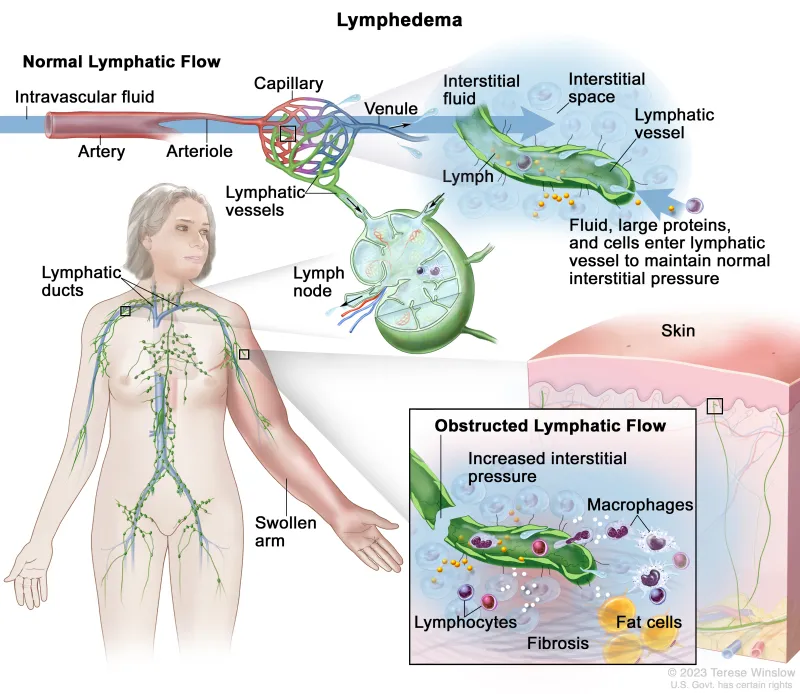
- Lymphedema: Most common, debilitating.
⭐ Lymphedema risk post-axillary dissection for breast cancer can be 20-30% with Axillary Lymph Node Dissection (ALND), reduced to <5-7% with SLNB alone_
High‑Yield Points - ⚡ Biggest Takeaways
- Sentinel Lymph Node Biopsy (SLNB) is key for staging melanoma & breast cancer; guides further dissection.
- Axillary Lymph Node Dissection (ALND) for positive SLNB or clinically positive axillary nodes in breast cancer.
- Radical Neck Dissection (RND) removes levels I-V nodes, SCM, IJV, & SAN; high morbidity.
- Modified Radical Neck Dissection (MRND) spares ≥1 non-lymphatic structures (SCM, IJV, SAN).
- Selective Neck Dissection (SND) targets specific at-risk nodal levels based on primary site.
- Common complications: lymphedema, seroma, nerve injury (e.g., spinal accessory).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

