Surgical Site Infections - Defining the Enemy
- SSI: Infection at/near surgical incision. Occurs within 30 days post-op, or 90 days if implant present.
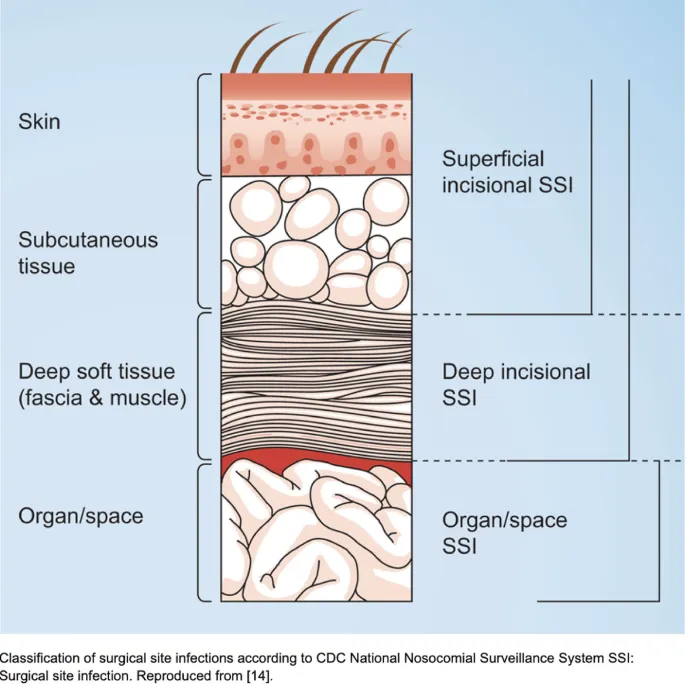
- CDC Classification (based on site):
- Superficial Incisional: Involves skin & subcutaneous tissue of the incision.
- Deep Incisional: Involves deep soft tissues (fascia, muscle layers) of the incision.
- Organ/Space: Involves any organ or space (other than incision) opened or manipulated during surgery.
⭐ SSIs are the most common healthcare-associated infection (HAI) in surgical patients, affecting up to 5% of procedures.
Surgical Site Infections - Bugs & Breaches
- Key Pathogens (Bugs):
- Staphylococcus aureus (MSSA/MRSA): Most common.
- Gram-negatives: E. coli, Pseudomonas aeruginosa, Klebsiella spp.
- Anaerobes: Bacteroides fragilis (esp. gut/pelvic surgery).
- Contributing Factors (Breaches):
- Patient Factors: Diabetes, obesity, smoking, malnutrition, immunosuppression.
- Procedural Factors:
- Surgery duration >2 hrs.
- Wound class (Dirty > Contaminated > Clean-Contaminated > Clean).
- Surgical technique (hematoma, dead space).
- Inadequate skin prep/antibiotic prophylaxis.
- 📌 Shaving (use clippers just before surgery).
⭐ Most SSIs are caused by the patient's endogenous flora (skin, mucous membranes, or hollow viscera).
Surgical Site Infections - Dodging Infection Darts
- Risk Factors:
- Patient: Diabetes (HbA1c > 7%), smoking, obesity (BMI > 30), malnutrition (Albumin < 3 g/dL), immunosuppression, MRSA carriage.
- Procedure: ↑Duration, emergency, implants, wound class (Dirty > Contaminated > Clean-contam. > Clean), poor technique.
- Prevention Pillars:
- Pre-op:
- Optimize: Glucose (<200mg/dL), nutrition, smoking cessation (4-6 wks).
- Skin: CHG shower, clip hair (no shaving).
- Prophylactic Antibiotics (AMP):
- IV within 60 min pre-incision (Vanco/FQ: 120 min).
- Correct drug. Re-dose if surgery >2 half-lives or blood loss >1500mL.
- Intra-op:
- Strict asepsis, normothermia, supplemental O2.
- Gentle tissue handling, minimize dead space.
- Post-op:
- Sterile dressing 24-48h. Glucose control.
- Stop AMP within 24h (Cardiac: 48h).
- Pre-op:
⭐ Prophylactic antibiotics: Administer within 60 minutes before incision (Vancomycin/Fluoroquinolones: 120 minutes). Discontinue within 24 hours post-op.
Surgical Site Infections - Spot, Diagnose, Defeat
- Spotting SSI:
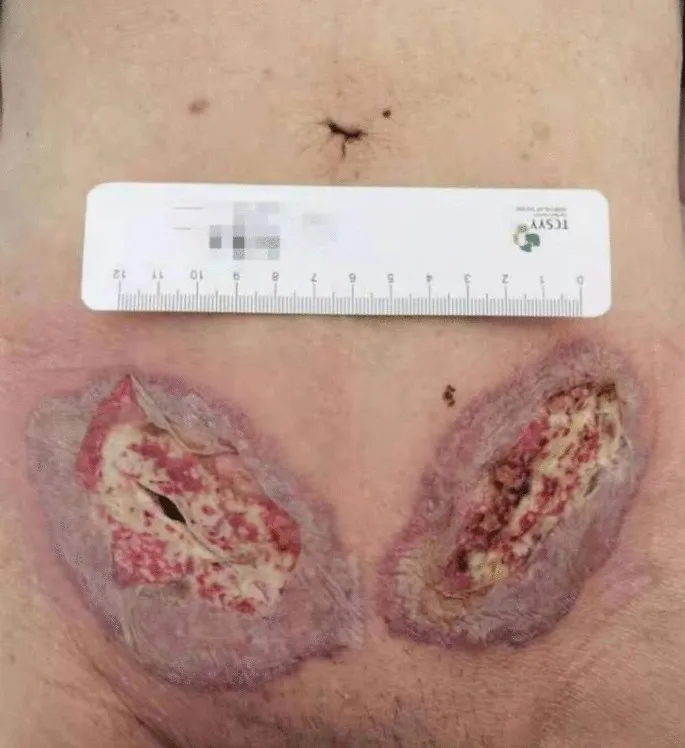
- Local: Pain, erythema, warmth, swelling, purulent discharge.
- Systemic: Fever >38°C, tachycardia, ↑WBC.
- Timing: Superficial (first 30 days), Deep/Organ-space (up to 1 year if implant).
- Diagnosis:
- Clinical: Local signs (pus, dehiscence) & systemic signs.
- Culture: Wound aspirate/biopsy for C&S (before Abx).
- Imaging: USG/CT for deep/organ-space collections.
- Labs: ↑WBC, ↑CRP; blood cultures if sepsis suspected.
- Defeating SSI (Management): 📌 4 D's: Drainage, Debridement, Dressings, Drugs (Antibiotics).
- Open & drain collections. Debride necrotic tissue.
- Antibiotics: Empiric: cover S. aureus (Cloxacillin/Cephalosporin); add Gram-neg/anaerobic for severe/deep. Then C&S guided.
- Consider Negative Pressure Wound Therapy (NPWT).
⭐ Staphylococcus aureus is the most common pathogen in SSIs.
High‑Yield Points - ⚡ Biggest Takeaways
- Staphylococcus aureus is the most common pathogen causing SSIs.
- SSIs are classified by depth: Superficial incisional, Deep incisional, Organ/Space.
- Give prophylactic antibiotics (e.g., Cefazolin) within 1 hour before incision.
- Key risk factors: diabetes, obesity, smoking, malnutrition, immunosuppression, prolonged surgery.
- Prevention: aseptic technique, clipping hair (not shaving), normothermia, glycemic control.
- Diagnosis is primarily clinical; wound culture guides antibiotics for established infection.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more