NOTES Basics - Scarless Surgery Secrets
- Definition: Natural Orifice Transluminal Endoscopic Surgery (NOTES) involves accessing the peritoneal cavity via a natural orifice (e.g., mouth, vagina, anus) and an internal, transluminal incision.
- Core Principle: Achieve "scarless" abdominal surgery.
- Key Advantages:
- No external incisions/scars.
- Potential for ↓ postoperative pain, faster recovery.
- ↓ incisional hernia risk, ↓ immunosuppression.
- vs. Laparoscopy: NOTES offers superior cosmesis (no visible scars) compared to minimal port-site scars in laparoscopy; potentially better patient perception.
⭐ Pioneering Procedure: The first human NOTES procedure was a transgastric appendectomy performed by Rao and Reddy in India in 2004.
Entry Points - Gateway to Guts
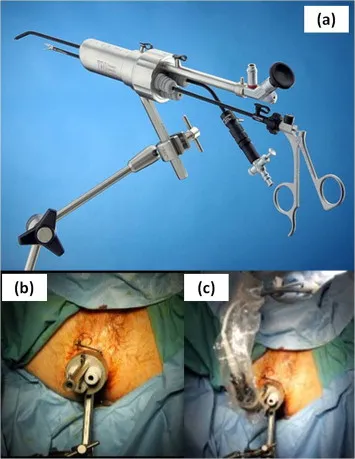
Access via natural orifices minimizes external scarring. Key routes include:
| Route | Key Considerations |
|---|---|
| Transgastric | Stomach wall access; Risk: peritonitis, bleeding; Closure: established techniques |
| Transvaginal | Preferred (♀); Robust closure, direct pelvic access; Low contamination risk |
| Transcolonic | Bowel access (rectum/colon); High contamination; Closure: technically challenging |
| Transvesical | Bladder access; Risk: urine leak, infection; Closure: still developing |
- Cholecystectomy, appendectomy
- Peritonoscopy, liver biopsy, lymph node biopsy
⭐ Transvaginal access is often preferred for female patients due to robust closure techniques and established safety in gynecological procedures.
NOTES Toolkit - Tiny Tools, Big Impact
- Specialized Endoscopes: Flexible endoscopes (e.g., R-scope, T-scope) with multiple (2-3) working channels for instrument passage.
- Endoluminal Suturing: Devices like T-tags, OverStitch enable internal tissue approximation and closure.
- Visualization Platforms: Articulating cameras provide dynamic views; enhanced imaging (e.g., NBI) improves tissue characterization.
- Energy Sources: Argon plasma coagulation (APC), monopolar/bipolar cautery for precise dissection and hemostasis.
- Key Challenges: Maintaining instrument stability, effective force application, and diminished haptic feedback.
⭐ A major challenge is achieving adequate 'triangulation' for tasks when instruments are passed coaxially through a single endoscope channel.
NOTES Hurdles - Navigating the Risks
⭐ Secure and reliable closure of the viscerotomy (access site) is the Achilles' heel of NOTES procedures.
- Major Challenges:
- Secure viscerotomy closure: Critical to prevent leaks, peritonitis; technically demanding.
- Infection control: Managing inevitable contamination from luminal contents; requires meticulous technique.
- Insufflation issues: Maintaining stable pneumoperitoneum; risk of CO2 embolism, subcutaneous emphysema.
- Spatial orientation & navigation: Challenging without traditional laparoscopic views or triangulation.
- Training, credentialing & ethics: Ensuring patient safety with novel procedures; clear guidelines needed.
- Potential Complications:
- Bleeding: Intra-operative or delayed, from access site or operative field.
- Visceral injury: To adjacent organs during access or dissection.
- Sepsis & abscess: Due to contamination or anastomotic/closure failure.
NOTES Now & Next - The Evolving Endoscope
- Current Status: Largely investigational, performed in highly specialized centers.
- Commonly Trialed: Transvaginal cholecystectomy; hybrid procedures (NOTES + laparoscopic aid).
⭐ Hybrid NOTES procedures, combining NOTES access with laparoscopic assistance, represent the most clinically relevant application currently.
- Adoption Barriers: Significant technical challenges, absence of dedicated platforms, high cost, steep learning curve.
- Future Horizons: Robotic NOTES (e.g., da Vinci SP via natural orifice), integrated advanced imaging, development of purpose-built NOTES platforms, AI-driven navigation and decision support.
- PG Relevance: Awareness of cutting-edge techniques and their potential future impact.
High‑Yield Points - ⚡ Biggest Takeaways
- NOTES involves accessing the peritoneal cavity via a natural orifice (e.g., mouth, vagina, anus).
- Aims for scarless surgery, potentially reduced pain, and quicker recovery.
- Transvaginal (TV-NOTES) is the most common and developed access route, often for cholecystectomy.
- Key challenges include secure viscerotomy closure, infection control, and specialized instrument development.
- Offers potential for less postoperative pain, improved cosmesis, and reduced incisional hernia risk.
- Remains largely investigational for many procedures but is established for select applications like transvaginal cholecystectomy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

