Neck Overview & Levels - Axial Atlas
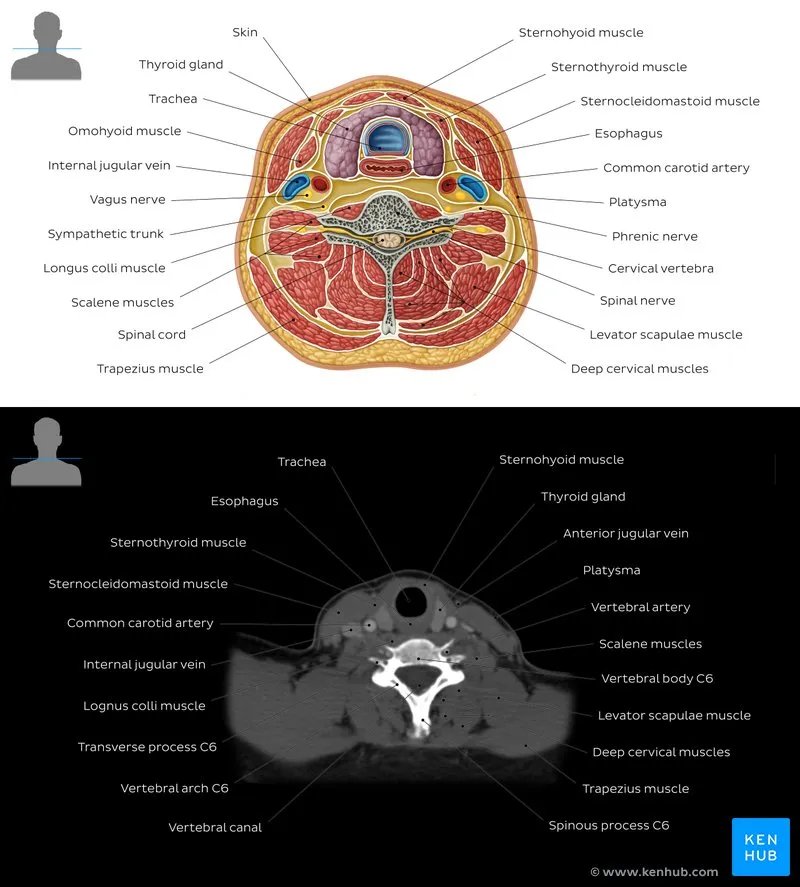
- Key Concept: Neck levels are crucial for staging & surgical planning, defined by consistent anatomical landmarks on axial imaging.
- Levels (Robbins/AJCC simplified for radiology):
- Level I: Submental & Submandibular triangles.
- IA: Submental (between anterior bellies of digastric).
- IB: Submandibular (posterior to anterior belly, anterior to posterior belly of digastric).
- Level II: Upper jugular (skull base to hyoid).
- IIA: Anterior to spinal accessory nerve (CN XI).
- IIB: Posterior to CN XI.
- Level III: Middle jugular (hyoid to cricoid).
- Level IV: Lower jugular (cricoid to clavicle).
- Level V: Posterior triangle (posterior to SCM, anterior to trapezius).
- VA: Superior (above cricoid arch inferior border).
- VB: Inferior (below cricoid arch inferior border, supraclavicular).
- Level VI: Anterior compartment (pretracheal, paratracheal, prelaryngeal/thyroid, recurrent laryngeal nerve nodes).
- Level VII: Superior mediastinal nodes (between common carotid arteries, below top of manubrium to innominate artery).
- Level I: Submental & Submandibular triangles.
⭐ Exam Favourite: The hyoid bone is a key landmark separating Level II (above) from Level III (below) in the jugular chain.
- Axial Views: Best for delineating fascial planes & lymph node groups.
- Identify major vessels: Carotid arteries, Jugular veins.
- Key muscles: Sternocleidomastoid (SCM), Digastric, Trapezius.
- Bony landmarks: Hyoid, Cricoid, Clavicle, Mandible, Vertebral bodies.
📌 Mnemonic (Levels): "Superman Saves Many Little Puppies Always" (Submental/Submandibular, Superior jugular, Middle jugular, Lower jugular, Posterior triangle, Anterior compartment) - Note: Level VII not included in this common mnemonic.
Fascial Layers & Spaces - Infection Mazes
- Superficial Cervical Fascia (SCF): Encloses platysma.
- Deep Cervical Fascia (DCF):
- Investing: Surrounds SCM, trapezius.
- Pretracheal: Encloses thyroid, trachea, esophagus.
- Prevertebral: Covers vertebral column, deep neck muscles.
- Carotid Sheath: Common carotid a., IJV, CN X.
Key Neck Spaces & Infection Pathways:
- Retropharyngeal Space (RPS):
- Buccopharyngeal fascia (ant) to alar fascia (post).
- Infection → danger space.
- Danger Space (Space 4):
- Alar fascia (ant) to prevertebral fascia (post).
- 📌 Extends skull base to diaphragm; infection → rapid mediastinitis.
- Prevertebral Space:
- Post. to prevertebral fascia; skull base to coccyx.
- Ludwig's Angina: Bilateral submandibular, sublingual, submental space infection.

⭐ Retropharyngeal abscess in children < 5 years often from URI; in adults, often from trauma/instrumentation.
Neck Viscera - Core Components
- Thyroid Gland: Butterfly-shape, anterior neck. Hyperdense on CT (iodine). Isthmus: 2nd-4th tracheal rings. Homogeneous enhancement.
- Key signs: Nodules, goiter.
- Parathyroid Glands: Typically 4, posterior to thyroid. Small; visualized if abnormal (e.g., adenoma).
- Larynx: Cartilaginous framework (thyroid, cricoid, arytenoids).
- Levels: Supraglottis, glottis, subglottis.
- Assess: Cartilage invasion, cord mobility.
- Pharynx: Posterior to nasal/oral cavities, larynx.
- Parts: Naso-, Oro-, Laryngopharynx.
- Trachea: Anterior to esophagus. C-shaped cartilages. Air-filled.
- Esophagus: Muscular tube, posterior to trachea. Usually collapsed.

⭐ The tracheoesophageal groove is a critical landmark housing the recurrent laryngeal nerve (RLN); injury leads to hoarseness.
Vessels, Nerves & Nodes - Vital Pathways
- Arteries:
- CCA: Bifurcates C3-C4. ICA: no neck branches.
- ECA: Supplies face/neck. Branches 📌 SALFOPMS (e.g., Sup. Thyroid, Facial).
- Vertebral: From subclavian, in C6-C1 transverse foramina.
- Veins:
- IJV: Main drainage, in carotid sheath.
- EJV: Superficial.
- Nerves:
- Vagus (X): In carotid sheath.
- CN IX, XI, XII: Close to major vessels.
- Phrenic (C3,4,5): To diaphragm. 📌 "C3,4,5 keeps diaphragm alive".
- Sympathetic trunk: Posterior to sheath.
- Lymph Nodes (Levels I-VI):
- I: Submental/mandibular. II: Upper Jugular. III: Mid Jugular.
- IV: Lower Jugular. V: Posterior Triangle. VI: Central.
⭐ Virchow's node (left supraclavicular - Level IV) signals GI malignancy.
High‑Yield Points - ⚡ Biggest Takeaways
- Cervical fascial layers (investing, pretracheal, prevertebral, carotid sheath) determine spread of neck infections and tumors.
- Carotid sheath contents: CCA/ICA (medial), IJV (lateral), CN X (posterior).
- Retropharyngeal space infection is a red flag; can cause mediastinitis.
- Thyroid gland: note its lobes, isthmus, and relation to trachea/esophagus.
- Key landmarks: hyoid bone, thyroid cartilage, cricoid cartilage, epiglottis.
- Lymph node levels (I-VII) are vital for H&N cancer staging and treatment.
- Vertebral arteries run superiorly within transverse foramina (typically C1-C6).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

