MDD Basics - Deep Dive Diagnosis
- Definition: Persistent low mood or anhedonia causing significant distress/impairment; common, often recurrent.
- DSM-5 Criteria: $\ge$ 5 of 9 symptoms in same 2-week period; must include (1) depressed mood or (2) anhedonia (loss of interest/pleasure).
- 📌 SIGECAPS:
- Sleep disturbance (insomnia/hypersomnia)
- Interest decreased (anhedonia)
- Guilt or worthlessness
- Energy decreased (fatigue)
- Concentration difficulties
- Appetite change (↑/↓) or weight change ($\ge$ 5%/month)
- Psychomotor agitation/retardation
- Suicidal ideation/thoughts
- 📌 SIGECAPS:
- Symptoms cause clinically significant distress or functional impairment.
- Not attributable to substance use or another medical condition. Episode not better explained by a psychotic disorder. No history of manic/hypomanic episode.
⭐ MDD is approximately twice as common in women as in men, a finding consistent across many cultures and countries.
Etiopathogenesis - Brain's Blue Notes
- Biological Factors:
- Monoamine Hypothesis: ↓ Serotonin (5-HT), ↓ Norepinephrine (NE), ↓ Dopamine (DA).
- Neuroendocrine:
- Hypothalamic-Pituitary-Adrenal (HPA) axis hyperactivity: ↑ Cortisol; Dexamethasone Suppression Test (DST) non-suppression.
- Thyroid dysfunction (e.g., hypothyroidism).
- Neuroinflammation: ↑ Pro-inflammatory cytokines (e.g., IL-6, TNF-α).
- Genetics:
- Heritability approx. ~37%.
- Gene-environment interaction (e.g., 5-HTTLPR polymorphism & stress).
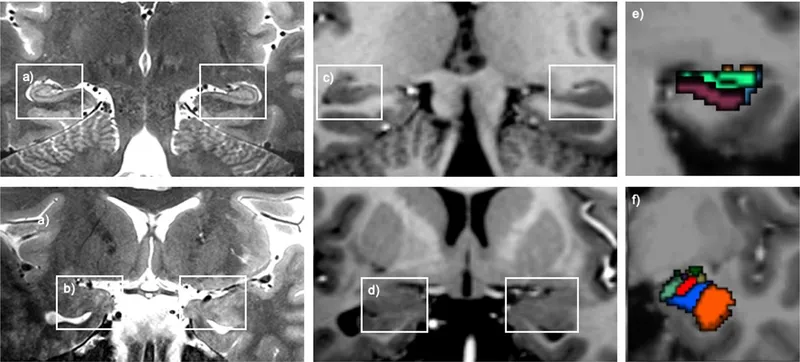
- Brain Structural & Functional Changes: ↓ Hippocampal volume; altered Prefrontal Cortex (PFC), amygdala, Anterior Cingulate Cortex (ACC) activity.
- Psychosocial Factors:
- Stressful life events (e.g., loss, trauma, abuse).
- Early life adversity.
- Personality traits (e.g., neuroticism, introversion).
- Cognitive theory (Beck's cognitive triad: negative view of self, world, future).
⭐ HPA axis dysregulation, particularly hypercortisolemia and non-suppression on the Dexamethasone Suppression Test (DST), is a well-documented biological finding in many patients with MDD.
Clinical Features & Diagnosis - Symptom Spotlight
- Core Criteria (DSM-5): ≥5 of 9 symptoms for ≥2 weeks; must include (1) depressed mood OR (2) anhedonia.
- 📌 SIGECAPS Mnemonic:
- Sleep disturbance (↑/↓)
- Interest loss (↓, anhedonia)
- Guilt (excessive, worthlessness)
- Energy loss (↓, fatigue)
- Concentration difficulties (↓, indecisiveness)
- Appetite change (↑/↓, weight change >5%/month)
- Psychomotor agitation/retardation (observable)
- Suicidal thoughts/ideation
- Key Exclusions: Symptoms not due to substance, other medical condition, or better explained by other psychotic disorders. Crucially, no history of mania/hypomania.
- Common Specifiers:
- Atypical features (mood reactivity, weight gain, hypersomnia, leaden paralysis, rejection sensitivity)
- Melancholic features (severe anhedonia, early morning awakening, diurnal variation worse AM, guilt)
- Psychotic features (delusions/hallucinations)
- Anxious distress
⭐ MDD with psychotic features often requires combination treatment with an antidepressant and an antipsychotic, or Electroconvulsive Therapy (ECT).
Management - Mood Menders
- Principles: Stepped care; aim for remission. Combine pharmacotherapy & psychotherapy.
- Pharmacotherapy:
- SSRIs (e.g., Fluoxetine): 1st line; SEs: GI, sexual.
- SNRIs (e.g., Venlafaxine).
- TCAs (e.g., Amitriptyline): Cardiotoxic, anticholinergic.
- MAOIs (e.g., Phenelzine): Hypertensive crisis risk.
- Augment/switch if poor response.
- Psychotherapy: CBT, IPT.
- Somatic Therapies:
- ECT: Severe, treatment-resistant, psychotic MDD, catatonia, high suicide risk.
- rTMS: For non-response.
- Duration: Continue antidepressants 6-9 months post-remission.
⭐ ECT is the most effective treatment for severe MDD, especially with psychotic features or high suicide risk. It is considered the safest psychotropic intervention during pregnancy.
High‑Yield Points - ⚡ Biggest Takeaways
- Core symptoms: Depressed mood or anhedonia for ≥2 weeks is essential for diagnosis.
- Use SIGECAPS mnemonic for common associated symptoms.
- SSRIs (e.g., Fluoxetine, Escitalopram) are first-line pharmacotherapy.
- ECT is indicated for severe/treatment-resistant depression, active suicidality, or catatonia.
- Key risk factors include female gender, family history, and stressful life events.
- Suicide risk assessment is paramount in all patients with MDD.
- Differentiate from Persistent Depressive Disorder (chronic depression, ≥2 years).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

