Body Fluid Compartments - Our Inner Oceans
- Total Body Water (TBW): Approx. 60% of body weight in adult males (lower in females, obese individuals).
- Intracellular Fluid (ICF): Constitutes 2/3 of TBW.
- Primary cation: $K^+$.
- Primary anions: $PO_4^{3-}$, proteins.
- Extracellular Fluid (ECF): Constitutes 1/3 of TBW.
- Primary cation: $Na^+$.
- Primary anion: $Cl^-$.
- Subdivisions:
- Interstitial Fluid (ISF): ~75% of ECF.
- Plasma: ~25% of ECF.
- Transcellular fluid (e.g., CSF, synovial fluid; small volume).
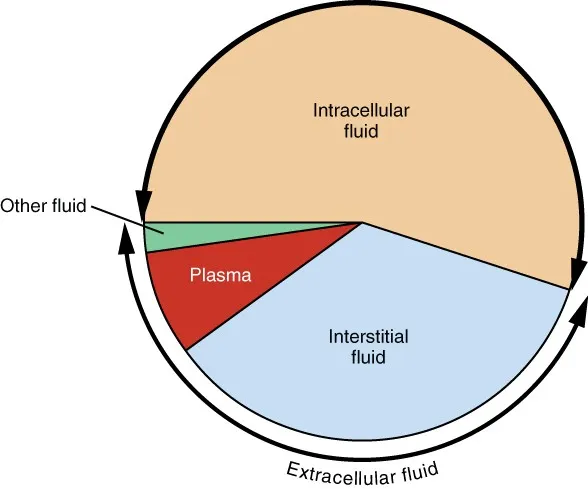
⭐ The 60-40-20 rule is a key clinical approximation: 60% of total body weight is water, 40% is ICF, and 20% is ECF.
Starling's Forces - Capillary Pressure Play
-
Fluid exchange between plasma & interstitium is governed by Starling's forces.
-
Net Filtration Pressure (NFP) dictates movement: $NFP = (P_c - P_{if}) - (\mathbf{\pi}c - \mathbf{\pi}{if})$.
- $P_c$: Capillary Hydrostatic Pressure; pushes fluid OUT (main outward force).
- $\mathbf{\pi}_c$: Capillary Oncotic Pressure (albumin); pulls fluid IN (main inward force).
- $P_{if}$: Interstitial Fluid Hydrostatic Pressure; pushes fluid IN.
- $\mathbf{\pi}_{if}$: Interstitial Fluid Oncotic Pressure; pulls fluid OUT.
-
Arteriolar end: Filtration favored ($P_c$ > $\mathbf{\pi}_c$).
-
Venular end: Reabsorption favored ($\mathbf{\pi}_c$ > $P_c$).

⭐ Increased capillary permeability (e.g., inflammation) allows protein leakage into interstitium (↑$\mathbf{\pi}_{if}$), causing edema.
Osmolality & Tonicity - Solute's Mighty Pull
- Osmolality: Measure of total solute concentration per kg solvent.
- Normal plasma: 280-295 mOsm/kg $H_2O$.
- Calculated: $2 \times [\text{Na}^+] + \frac{[\text{Glucose}]}{18} + \frac{[\text{BUN}]}{2.8}$ (units: Na mEq/L, others mg/dL).
- Mainly regulated by ADH.
- Tonicity: Effective osmolality; drives H₂O movement across membranes. Depends on impermeable solutes.
- Isotonic: No net H₂O movement (e.g., 0.9% NaCl).
- Hypotonic: H₂O enters cells → cells swell (e.g., 0.45% NaCl).
- Hypertonic: H₂O leaves cells → cells shrink (e.g., 3% NaCl, Mannitol).
- 📌 Osmolality: all solutes. Tonicity: only non-penetrating solutes. Urea: ineffective osmole.
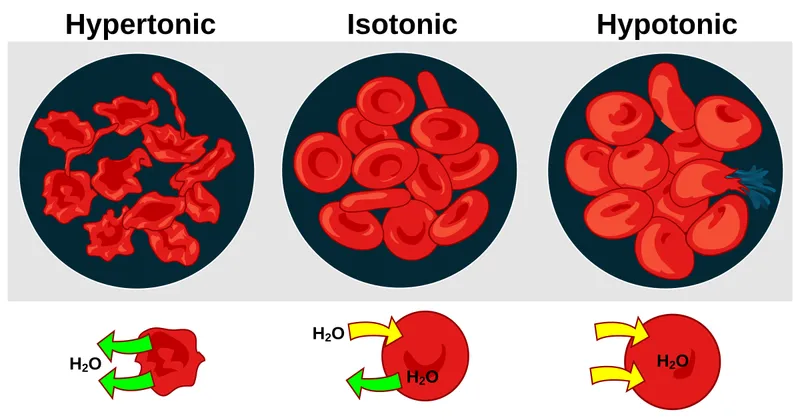
⭐ Mannitol (osmotic diuretic) ↑ ECF osmolality, draws H₂O from ICF. Used to ↓ intracranial & intraocular pressure.
Fluid Shift Scenarios - Clinical Case Clues
- Heart Failure: ↑$P_c$ (systemic/pulmonary) → Peripheral/pulmonary edema. Clues: Dyspnea, JVD, crackles.
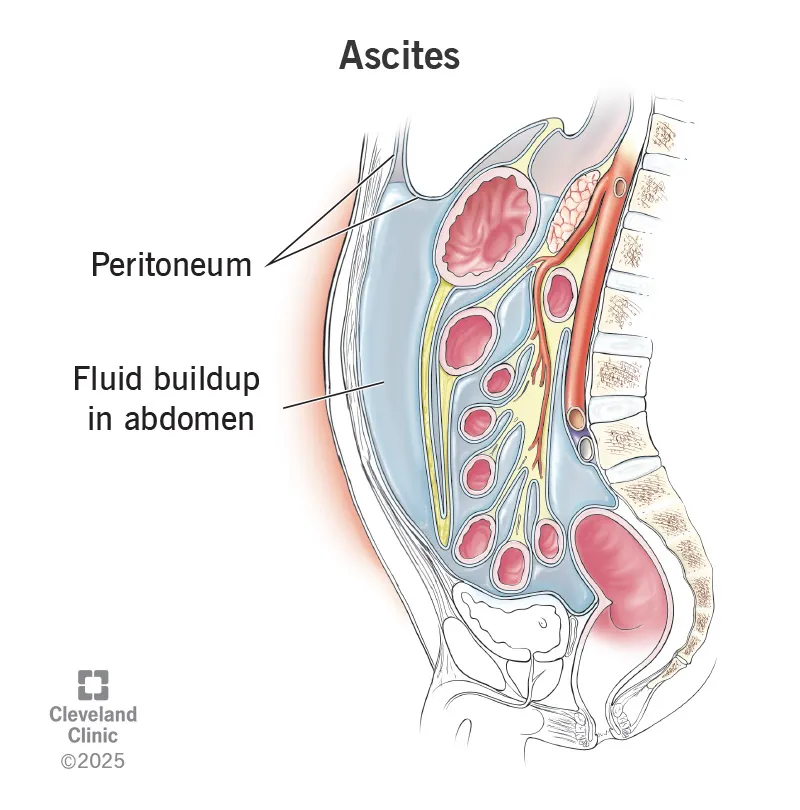
- Liver Cirrhosis: ↓$\pi_p$ (↓albumin synthesis) + ↑$P_c$ (portal HTN) → Ascites, peripheral edema. Clues: Jaundice, spider nevi.
- Nephrotic Syndrome: ↓$\pi_p$ (proteinuria) → Generalized edema (anasarca), periorbital puffiness. Clues: Frothy urine, >3.5 g/day proteinuria.
- Sepsis/Burns: ↑Capillary permeability → Generalized edema, intravascular volume depletion. Clues: Fever, hypotension, inflammation.
- Lymphatic Obstruction: Impaired interstitial fluid drainage → Lymphedema. Clues: Non-pitting edema, history of surgery/radiation.
⭐ In nephrotic syndrome, massive proteinuria (typically >3.5 g/day) leads to decreased plasma oncotic pressure, a primary driver of generalized edema (anasarca).
Regulation of Balance - Hormonal Harmony
- ADH (Vasopressin): From posterior pituitary. Trigger: ↑plasma osmolality, ↓volume. Action: ↑$H_2O$ reabsorption (collecting ducts).
- Aldosterone (RAAS): From adrenal cortex. Trigger: ↓renal perfusion (Angiotensin II), ↑$K^+$. Action: ↑$Na^+$ & $H_2O$ reabsorption, ↑$K^+$ excretion (DCT/CD).
- Natriuretic Peptides (ANP/BNP): From heart. Trigger: Atrial/ventricular stretch. Action: Natriuresis, diuresis, vasodilation; oppose RAAS.
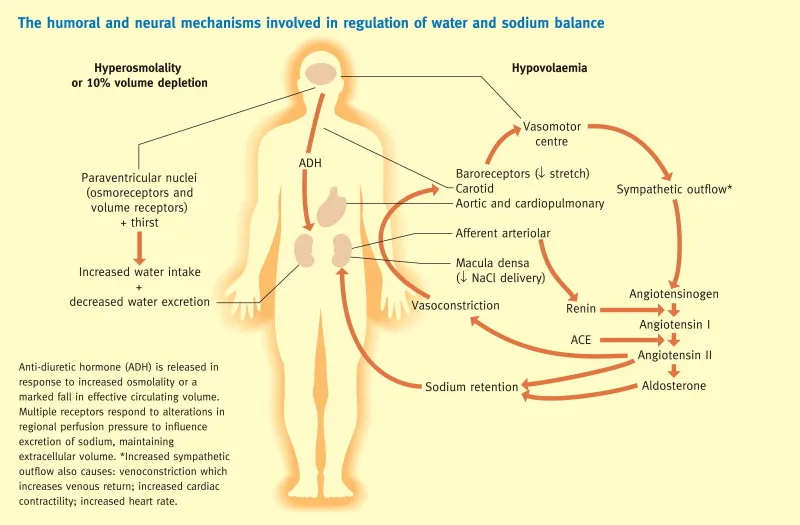
⭐ SIADH (Syndrome of Inappropriate ADH) leads to euvolemic hyponatremia due to excessive water retention and resultant sodium dilution.
High‑Yield Points - ⚡ Biggest Takeaways
- Osmolality differences drive water movement between ICF and ECF.
- Sodium (Na+) is the main determinant of ECF osmolality and volume.
- Water moves passively from lower to higher osmolality areas.
- Isotonic solutions (0.9% Saline) expand ECF volume without major ICF shifts.
- Hypotonic solutions (0.45% Saline) shift water into cells, causing ICF expansion.
- Hypertonic solutions (3% Saline) draw water out of cells, causing ICF contraction.
- Starling forces govern fluid exchange between plasma and interstitial fluid.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

