Hemostasis & Clotting Factors - Body's Plug Plan
- Hemostasis: Physiological process stopping blood loss.
- Primary: Immediate vascular spasm. Platelet plug formation:
- Adhesion (von Willebrand Factor (vWF) binds GpIb).
- Activation (platelets release ADP, TXA2).
- Aggregation (GpIIb/IIIa binds fibrinogen, linking platelets).
- Secondary: Coagulation cascade (Intrinsic, Extrinsic, Common pathways) activation → Fibrin mesh formation, stabilizing the plug.
- Primary: Immediate vascular spasm. Platelet plug formation:
- Key Clotting Factors: Series of plasma proteins (mostly zymogens from liver).
- I: Fibrinogen (precursor to fibrin).
- II: Prothrombin (precursor to thrombin).
- III: Tissue Factor (TF) / Thromboplastin (activates extrinsic pathway).
- IV: Calcium ($Ca^{2+}$) (essential cofactor).
- Vitamin K-dependent factors: II, VII, IX, X, Protein C, Protein S. 📌 Mnemonic: "1972" (IX, X, VII, II) + C&S.

⭐ Factor VII has the shortest half-life among all clotting factors, making it the first to decrease with warfarin therapy or liver disease affecting Vitamin K-dependent factor synthesis.
Coagulation Cascade - Clotting Dominoes

- Intrinsic Pathway (aPTT): Activated by contact with negatively charged surfaces (e.g., collagen).
- Factors: XII → XI → IX (+VIIIa, Phospholipids (PL), $Ca^{2+}$) → X.
- Monitored by: Activated Partial Thromboplastin Time (aPTT).
- 📌 Mnemonic: PTT - Play Table Tennis (Inside). Factors 12, 11, 9, 8.
- Extrinsic Pathway (PT): Activated by Tissue Factor (TF/Factor III) release from damaged tissue.
- Factors: VII (+TF, PL, $Ca^{2+}$) → X.
- Monitored by: Prothrombin Time (PT).
- 📌 Mnemonic: PT - Play Tennis (Outside). Factor 7 (and 3).
- Common Pathway: Convergence of intrinsic and extrinsic pathways.
- Factors: Xa (+Va, PL, $Ca^{2+}$) converts Prothrombin (II) → Thrombin (IIa).
- Thrombin (IIa): Converts Fibrinogen (I) → Fibrin (Ia); Activates Factor XIII.
- Factor XIIIa: Cross-links fibrin monomers → Stable clot.
- 📌 Mnemonic: Factors 10, 5, 2, 1 (e.g., $10 bill, $5 bill, $2 coin, $1 coin).
⭐ Vitamin K is crucial for the $\gamma$-carboxylation and activation of clotting factors II, VII, IX, X, and anticoagulant proteins C & S. Warfarin acts by inhibiting Vitamin K epoxide reductase.
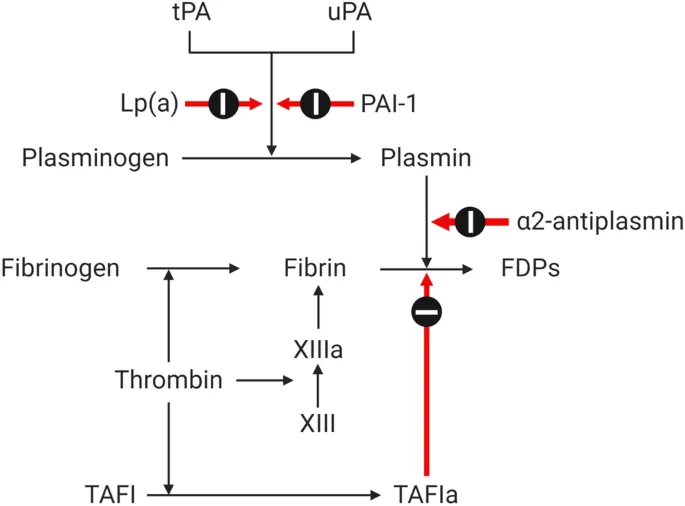
Fibrinolysis & Regulation - Clot Dissolution Crew
- Core Process: Breakdown of fibrin clot.
- Key Enzyme: Plasmin (active form of Plasminogen).
- Activation: Plasminogen → Plasmin by:
- Tissue Plasminogen Activator (t-PA): Endothelial cells; major physiological.
- Urokinase Plasminogen Activator (u-PA).
- Plasmin Action: Degrades fibrin mesh → FDPs (incl. D-dimer).
- $Fibrin \xrightarrow{Plasmin} FDPs + D-dimer$
- Regulation (Inhibitors):
- α2-Antiplasmin (α2-AP): Primary inhibitor of free plasmin.
- PAI-1 (Plasminogen Activator Inhibitor-1): Inhibits t-PA & u-PA.
- TAFI (Thrombin Activatable Fibrinolysis Inhibitor): ↓ fibrinolysis (modifies fibrin, ↓ plasminogen/t-PA binding).
⭐ D-dimer: Specific marker for active fibrinolysis (cross-linked fibrin breakdown); elevated in Deep Vein Thrombosis (DVT), Pulmonary Embolism (PE), and Disseminated Intravascular Coagulation (DIC).
Lab Tests & Disorders - When Clotting Goes Wrong
- Common Lab Tests:
- PT/INR: Extrinsic/Common (FVII). Warfarin (INR 2-3).
- aPTT: Intrinsic/Common (FVIII, IX, XI, XII). Heparin.
- Bleeding Time/PFA-100: Platelet function, vWD.
- Fibrinogen: ↓ in DIC.
- D-dimer: ↑ Fibrin Degradation Product (DVT, PE, DIC).
- Mixing studies: Factor deficiency (corrects) vs. inhibitor (no correction).
- Bleeding Disorders:
- Hemophilia A (↓FVIII), B (↓FIX): X-linked. ↑aPTT.
- Von Willebrand Disease (vWD): Most common inherited. ↑BT/PFA.
- Vitamin K Deficiency: ↑PT, ↑aPTT (Factors II, VII, IX, X, Protein C, S).
- DIC: ↑PT, ↑aPTT, ↓Fibrinogen, ↑D-dimer, ↓Platelets.
- Thrombotic Disorders (Hypercoagulable):
- Factor V Leiden (APC resistance) - Most common inherited.
- Antiphospholipid Syndrome (APS).
⭐ Failure of aPTT to correct with a 1:1 mixing study (plasma mixing test) suggests the presence of a coagulation factor inhibitor (e.g., lupus anticoagulant or specific factor inhibitor).
High‑Yield Points - ⚡ Biggest Takeaways
- Vitamin K is essential for synthesis of factors II, VII, IX, X, Protein C & S.
- Hemophilia A (Factor VIII deficiency) and B (Factor IX deficiency) are key X-linked recessive disorders.
- von Willebrand Disease, most common inherited bleeding disorder, impacts vWF and Factor VIII activity.
- PT/INR measures extrinsic/common pathways (Warfarin); aPTT measures intrinsic/common pathways (Heparin).
- Plasmin, from plasminogen via tPA/uPA, mediates fibrinolysis; D-dimer indicates active clot breakdown.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

