Intro & MOA - The Calm Keepers
- Prophylactic anti-inflammatory agents; prevent/reduce allergic reaction severity.
- Target mast cells, key in Type I hypersensitivity reactions.
- Not bronchodilators; ineffective for acute asthma attacks/anaphylaxis.
- Mechanism of Action (MOA):
- Stabilize mast cell membranes, preventing degranulation upon allergen exposure.
- Inhibit release of inflammatory mediators:
- Histamine
- Leukotrienes (e.g., LTC₄, LTD₄)
- Prostaglandins (e.g., PGD₂)
- Cytokines
- Modulate delayed chloride ($Cl^−$) channels in the cell membrane, reducing $Ca^{2+}$ influx essential for exocytosis.
- 📌 Mnemonic: "Keep the CALM": Chloride channel ALteration Mast cell stabilization.
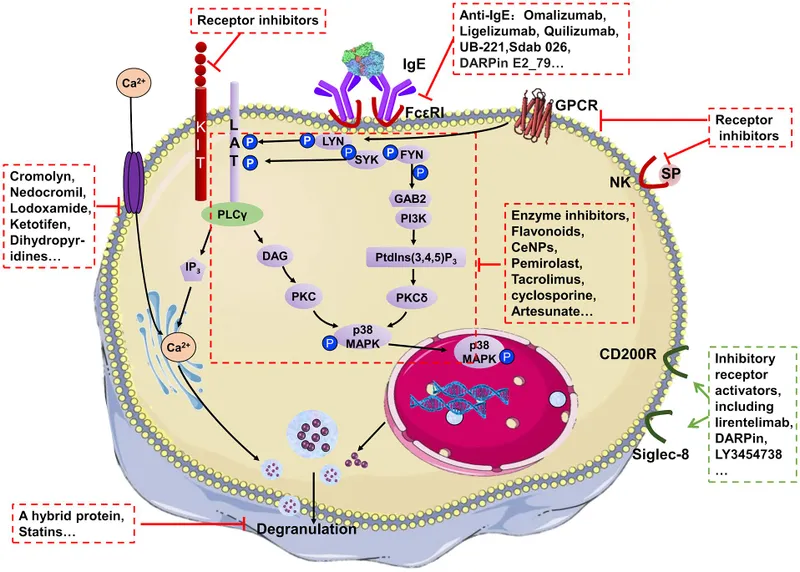
⭐ Cromolyn sodium & Nedocromil are classic examples; primarily used for prophylaxis of mild persistent asthma, especially exercise-induced or allergen-induced asthma in children, and allergic rhinitis/conjunctivitis.
Pharmacokinetics - Journey of Stabilizers
- Absorption (A):
- Oral: Very poor (<1%); not for systemic use.
- Inhalation: Main route for local lung effect. Small systemic absorption.
- Topical: Nasal/ophthalmic for local action.
- Distribution (D):
- Acts locally (airways, nose, eyes). Minimal systemic distribution.
- Metabolism (M):
- Not metabolized; excreted unchanged.
- Excretion (E):
- Absorbed fraction: Urine and bile (equal).
- Unabsorbed oral: Feces.
- Half-life (Cromolyn): ~80-90 min.
⭐ Low systemic absorption (~8-10%) via inhalation is key, minimizing systemic adverse effects.
Key Drugs & Uses - Stabilizer Superstars
- Cromolyn Sodium (Disodium Cromoglycate)
- Mechanism: Stabilizes mast cell membranes, preventing degranulation and release of inflammatory mediators (histamine, leukotrienes).
- Uses:
- Prophylaxis of bronchial asthma (allergic, exercise-induced, irritant-induced). Not for acute bronchospasm.
- Allergic rhinitis (nasal solution).
- Allergic conjunctivitis (ophthalmic solution).
- Food allergy (oral, for GI symptoms).
- Systemic mastocytosis.
- Dosage Forms: Metered-dose inhaler (MDI), nebulizer solution, nasal spray, eye drops (2-4%), oral capsules.
- 📌 Mnemonic: "Cromolyn keeps mast cells from cryin' (degranulating)".
- Nedocromil Sodium
- Mechanism: Similar to cromolyn, inhibits mast cell degranulation and release of mediators. May also inhibit other inflammatory cells.
- Uses:
- Prophylaxis of mild to moderate asthma.
- Allergic conjunctivitis (ophthalmic solution).
- Dosage Forms: MDI, eye drops.
- Ketotifen
- Mechanism: Mast cell stabilizer with potent H1-antihistaminic activity.
- Uses:
- Long-term prophylaxis of asthma (oral).
- Allergic rhinitis (oral, nasal spray).
- Allergic conjunctivitis (ophthalmic solution 0.025%).
- Dosage Forms: Tablets, syrup, eye drops, nasal spray.

⭐ Ketotifen is unique as it combines mast cell stabilizing properties with significant H1-receptor antagonism, making it particularly useful for allergic conditions with prominent itching or sneezing.
Side Effects & Cautions - Stabilizer Setbacks
- General: Usually mild & transient.
- Inhaled (Cromolyn, Nedocromil):
- Common: Throat irritation, cough, bronchospasm (paradoxical).
- Nedocromil: Unpleasant taste.
- Headache.
- Oral (Ketotifen):
- Sedation (H1-blocking effect). 📌 K for Knockout.
- Increased appetite, weight gain, dry mouth.
- Ocular Preparations: Local irritation, stinging.
- Serious (Rare):
- Hypersensitivity reactions (e.g., anaphylaxis).
- Cromolyn: Eosinophilic pneumonia, laryngeal edema.
- Cautions & Contraindications:
- Known hypersensitivity.
- ⚠️ Acute asthma/bronchospasm: Ineffective; for prophylaxis ONLY.
- Ketotifen: Caution with tasks requiring alertness (driving).
- Abrupt withdrawal may precipitate symptoms.
⭐ Mast cell stabilizers are primarily prophylactic; they do not provide immediate relief in an acute asthma attack.
High‑Yield Points - ⚡ Biggest Takeaways
- Mechanism: Inhibit mast cell degranulation, preventing histamine/leukotriene release.
- Key Drugs: Cromolyn sodium, Nedocromil; Ketotifen (also H1 blocker).
- Primary Use: Prophylaxis of allergic asthma (esp. exercise-induced) & allergic rhinitis.
- Not for Acute Attacks: For long-term prevention, not acute relief.
- Administration: Mainly inhalation; Ketotifen also oral/ophthalmic.
- Safety: Excellent safety profile, minimal side effects; safe in children.
- Onset: Slow; benefits in 2-4 weeks with regular use.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

