Blood Products & Indications - What's in the Bag?
| Product | Contents | Vol (mL) | Indications (Key Thresholds) | Storage | Notes |
|---|---|---|---|---|---|
| PRBCs | RBCs, residual plasma/WBCs/plts | ~300 | Anemia (Hb < 7 g/dL), Acute loss >20% | 2-6°C; 35-42d | Leukoreduce, Irradiate |
| Platelets (PC) | Platelets, plasma | ~50-70 | Plt < 10,000/µL, Dysfunctional plts + bleeding | 20-24°C (agitate); 5d | RDP/SDP |
| FFP | All clotting factors, plasma proteins | ~250 | Coagulopathy (INR > 1.5), TTP, DIC | ≤ -18°C; 1yr | Thaw 30-37°C |
| Cryoprecipitate | Fibrinogen, FVIII, FXIII, vWF | ~15 | Fibrinogen < 100 mg/dL, FVIII/FXIII def, vWD | ≤ -18°C; 1yr | Factor concentrate |
| Whole Blood | All components | ~450 | Massive hemorrhage, Exchange Txn | 2-6°C; 21-35d | Rare; component therapy preferred |
Compatibility & Crossmatching - Perfect Match Quest
- ABO System (Landsteiner's Law): RBC Ag + plasma Ab.
Grp Ag Ab Donates RBC to Receives RBC from A A Anti-B A, AB A, O B B Anti-A B, AB B, O AB A, B None AB A,B,AB,O (All) O H Anti-A/B A,B,AB,O (All) O - Rh System: RhD Ag key. Rh(D)-neg: Anti-D (IgG) if sensitized (Rh+ exposure) → HDN risk.
- Crossmatching: Pre-transfusion.
- Major: Donor RBCs + Recipient serum (Recipient Ab vs Donor Ag).
- Minor: Donor serum + Recipient RBCs.
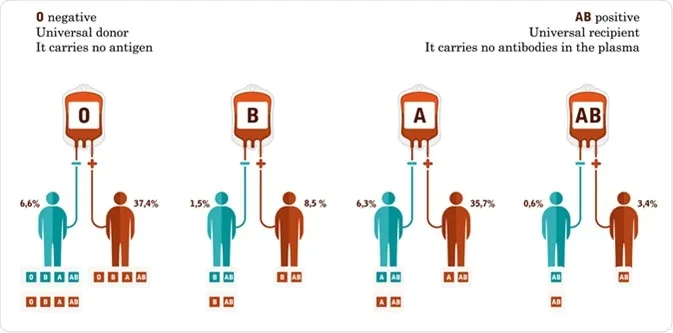
- 📌 O RhD neg: Universal RBC Donor; AB RhD pos: Universal RBC Acceptor.
⭐ Bombay Blood Group (Oh): Lacks H antigen. Has anti-A, anti-B, anti-H. Can only receive Oh blood.
Transfusion Reactions - When Good Blood Goes Bad
- Immediate Reactions (Minutes to hours)
- Acute Hemolytic Transfusion Reaction (AHTR)
- Onset: Minutes
- Symptoms/Signs: Fever, chills, hemoglobinuria (red urine), hypotension, DIC, flank pain.
- Pathophysiology: ABO incompatibility; intravascular hemolysis (IgM mediated).
- Prevention: Meticulous pre-transfusion testing.
- Management: Stop transfusion, IV fluids, diuretics, manage DIC.
- Febrile Non-Hemolytic Transfusion Reaction (FNHTR)
- Onset: 30 min - 6 hrs
- Symptoms/Signs: Fever (↑ 1°C), chills, rigors.
- Pathophysiology: Cytokines from donor WBCs. 📌 Mnemonic: Febrile = Cytokines from WBCs.
- Prevention: Leukoreduction.
- Management: Antipyretics; exclude hemolysis.
- Allergic/Anaphylactic Reaction
- Onset: Minutes (anaphylaxis) to hours (mild allergic)
- Symptoms/Signs: Urticaria, pruritus; (anaphylaxis: angioedema, bronchospasm, hypotension).
- Pathophysiology: IgE mediated (recipient IgE vs donor plasma proteins); IgA deficiency (anaphylaxis).
- Prevention: Antihistamines; washed RBCs for IgA deficient.
- Management: Antihistamines, steroids; epinephrine for anaphylaxis.
- Transfusion-Associated Circulatory Overload (TACO)
- Onset: Within 6 hrs
- Symptoms/Signs: Dyspnea, orthopnea, hypertension, pulmonary edema.
- Pathophysiology: Volume overload.
- Prevention: Slow infusion, diuretics.
- Management: Oxygen, diuretics, sit upright.
- Transfusion-Related Acute Lung Injury (TRALI)
- Onset: Within 6 hrs
- Symptoms/Signs: Acute dyspnea, hypoxia, bilateral pulmonary infiltrates, fever, hypotension.
- Pathophysiology: Donor antibodies vs. recipient leukocytes.
- Prevention: Screen donors (multiparous women).
- Management: Supportive, oxygen, ventilation if needed.
- Acute Hemolytic Transfusion Reaction (AHTR)
⭐ Exam Favourite: TRALI: Donor antibodies vs. recipient leukocytes (immune); TACO: Simple volume overload, often in elderly or cardiac patients. Key differentiator: BNP levels (↑ in TACO, normal/low in TRALI).
- Delayed Reactions (Days to weeks)
- Delayed Hemolytic Transfusion Reaction (DHTR)
- Onset: 3-10 days
- Symptoms/Signs: Jaundice, fever, unexpected ↓Hb.
- Pathophysiology: Anamnestic response to non-ABO antigens (e.g., Kidd, Duffy); extravascular hemolysis (IgG).
- Prevention: Antibody screening.
- Management: Usually supportive.
- Delayed Hemolytic Transfusion Reaction (DHTR)
Alternatives & Special Situations - Beyond the Donor
- Pharmacological Alternatives:
- Erythropoiesis-Stimulating Agents (ESAs): E.g., Epoetin, Darbepoetin; stimulate RBC production.
- Iron Therapy: Oral/IV for iron deficiency anemia.
- Non-Pharmacological Alternatives:
- Autologous Transfusion: Patient's pre-donated blood.
- Intraoperative Cell Salvage: Collects & reinfuses shed surgical blood.
- Acute Normovolemic Hemodilution: Pre-op blood removal, volume replacement, later reinfusion.
- Massive Transfusion Protocol (MTP):
- For major hemorrhage (e.g., >10 units PRBCs/24h).
- Components: PRBC:FFP:Platelets, typically 1:1:1 ratio.
- Aims: Correct lethal triad (acidosis, hypothermia, coagulopathy).
- Adjuncts: Calcium, Tranexamic Acid (TXA).
⭐ Tranexamic acid (TXA) inhibits fibrinolysis; used in trauma and MTPs to ↓ bleeding. Dose: 1g IV loading, then 1g over 8 hours.
High‑Yield Points - ⚡ Biggest Takeaways
- Universal RBC donor: O RhD negative; Universal RBC recipient: AB RhD positive.
- Universal plasma donor: AB group; Universal plasma recipient: O group.
- Massive transfusion: >10 units PRBCs in 24h or >4 units in 1h; risks hypothermia, coagulopathy, hypocalcemia.
- FNHTR: Most common reaction; due to cytokines; prevent with leukoreduction.
- TRALI: Leading mortality cause; donor antibodies vs recipient leukocytes.
- Blood storage lesion: ↓ 2,3-DPG, ↓ pH, ↑ K+; RBCs viable 35-42 days.
- Alternatives: Erythropoietin, iron, autologous transfusion, cell salvage.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

