Antiplatelet Drugs - Setting the Stage
- Hemostasis & Thrombosis: Platelets crucial for primary hemostasis; dysregulation leads to thrombosis.
- Platelet Plug Formation:
- Adhesion (GPIb-vWF to collagen)
- Activation & Release (TXA2, ADP)
- Aggregation (GPIIb/IIIa crosslinking)
- Primary Drug Targets:
- COX-1 (TXA2 synthesis)
- P2Y12 Receptors (ADP action)
- GPIIb/IIIa Receptors (Aggregation)
⭐ Thromboxane A2 (TXA2) is a potent platelet aggregator and vasoconstrictor, synthesized from arachidonic acid by COX-1 in platelets.
Antiplatelet Drugs - Aspirin's Reign
- Mechanism: Irreversibly acetylates & inhibits COX-1 → ↓ Thromboxane A2 (TXA2) → ↓ platelet aggregation.
- Duration: Effect lasts for platelet lifespan (7-10 days).
- Dose (Antiplatelet): Low dose, 75-150 mg daily.
- Key Uses:
- MI & stroke prophylaxis/treatment.
- TIA prevention.
- Adverse Effects:
- GI upset/bleeding.
- Aspirin-induced asthma.
- ⚠️ Reye's syndrome (children with viral illness).
⭐ Aspirin's antiplatelet effect is due to irreversible acetylation of a serine residue on COX-1, lasting for the platelet's lifespan (7-10 days).
Antiplatelet Drugs - P2Y12 Blockers
Block ADP binding to P2Y12 platelet receptor → ↓platelet activation/aggregation. Crucial in DAPT with Aspirin.
- Thienopyridines (Irreversible, Prodrugs)
- Clopidogrel: CYP2C19 activation needed. Load: 300-600 mg; Maint: 75 mg OD. 📌 "ClOPidogrel needs Cytochrome P enzymes."
- Prasugrel: Potent, faster onset. Contra: TIA/stroke. Load: 60 mg; Maint: 10 mg OD.
- Ticlopidine: Older, more SE (neutropenia, TTP).
- Non-Thienopyridines (Reversible)
- Ticagrelor: Direct-acting. Load: 180 mg; Maint: 90 mg BD. Dyspnea common.
⭐ Ticagrelor is a reversible, direct-acting P2Y12 inhibitor that does not require metabolic activation, unlike clopidogrel and prasugrel.
- Cangrelor: IV, rapid on/off. PCI use.
- Ticagrelor: Direct-acting. Load: 180 mg; Maint: 90 mg BD. Dyspnea common.
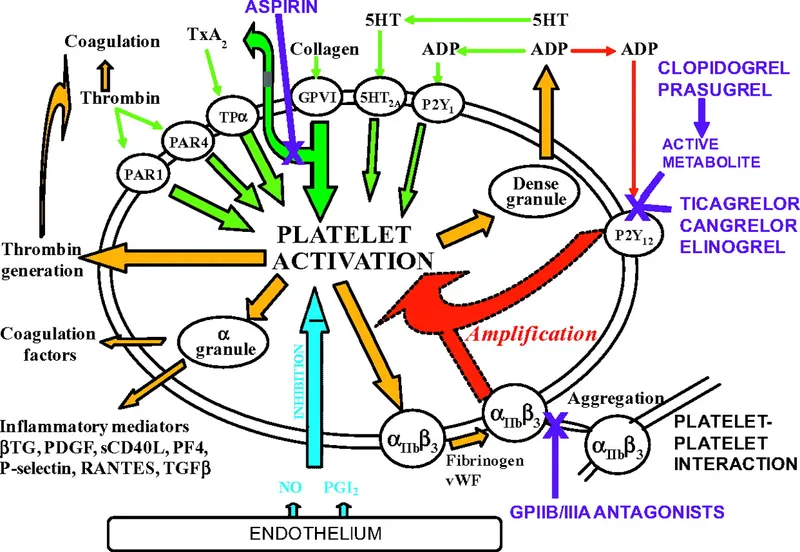
Uses: ACS, PCI, stroke prevention. Main AE: Bleeding; TTP (rare).
Antiplatelet Drugs - Final Pathway Blockers
- Glycoprotein (GP) IIb/IIIa inhibitors: Block the final common pathway of platelet aggregation, preventing fibrinogen binding.
- Agents (IV only):
- Abciximab (monoclonal antibody)
- Eptifibatide (peptide)
- Tirofiban (non-peptide)
- Use: High-risk acute coronary syndromes (ACS), percutaneous coronary intervention (PCI).
- Side Effects: Bleeding, thrombocytopenia.
⭐ Abciximab, a chimeric monoclonal antibody against GP IIb/IIIa, can cause profound and long-lasting platelet inhibition and carries a risk of thrombocytopenia.
- 📌 Abciximab, Eptifibatide, Tirofiban = AETiology of no clots!
Antiplatelet Drugs - Diverse Mechanisms
- Dipyridamole: PDE inhibitor (↑cAMP); inhibits adenosine uptake. Used with aspirin.
- Cilostazol: Selective PDE3 inhibitor (↑cAMP). For intermittent claudication.
⭐ Cilostazol, a PDE3 inhibitor used for intermittent claudication, is contraindicated in patients with heart failure of any severity due to increased mortality risk.
- Epoprostenol (PGI₂): Prostacyclin analog (↑cAMP). Potent vasodilator; for PAH, dialysis.
- Vorapaxar: PAR-1 antagonist (thrombin receptor). Blocks thrombin-induced platelet activation.
High‑Yield Points - ⚡ Biggest Takeaways
- Aspirin irreversibly inhibits COX-1, reducing Thromboxane A2 (TXA2) and platelet aggregation.
- P2Y12 inhibitors: Clopidogrel & Prasugrel (prodrugs, irreversible), Ticagrelor (not prodrug, reversible).
- Clopidogrel efficacy reduced by CYP2C19 polymorphisms; Prasugrel contraindicated in TIA/stroke.
- GPIIb/IIIa inhibitors (e.g., Abciximab) are most potent, blocking the final aggregation step.
- Cilostazol, a PDE3 inhibitor, treats intermittent claudication via vasodilation and antiplatelet effects.
- Primary risk for all antiplatelets: Increased bleeding.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

