General Management of Poisoning - The First Response
- Initial Stabilization (ABCDs):
- Airway: Secure.
- Breathing: Oxygen, ventilate if needed.
- Circulation: IV access, fluids, vasopressors.
- Disability: GCS, pupils, glucose (check & correct).
- Decontamination: Goal: Prevent absorption.
- Skin/Eyes: Remove clothes, irrigate.
- GI Decontamination:
- Activated Charcoal (AC): 1 g/kg. Best within 1 hr. 📌 Not for PHAILS (Petroleum, Heavy metals, Alcohols, Iron, Lithium, Solvents/Corrosives).
- Gastric Lavage: Rarely used; within 1 hr for severe cases.
- Whole Bowel Irrigation (WBI): Body packers, SR tabs, metals.
- Enhanced Elimination:
- Multiple Dose AC (MDAC): For enterohepatic recirculation (Theophylline, Phenobarbital, Carbamazepine, Dapsone).
- Urinary Alkalinization: Salicylates, Phenobarbital.
- Hemodialysis: Severe cases (Salicylates, Lithium, Ethylene glycol, Methanol, Barbiturates). 📌 I STUMBLE.
⭐ Prioritize ABCDs stabilization before decontamination or antidotes in all poisoning cases.
Paracetamol & Opioids - Popular Poisons
Paracetamol (Acetaminophen) Toxicity
- Mechanism: Glutathione depletion → NAPQI (toxic metabolite) accumulation → hepatic necrosis.
- Toxic dose: >150 mg/kg or >7.5 g. Peak hepatotoxicity: 72-96h.
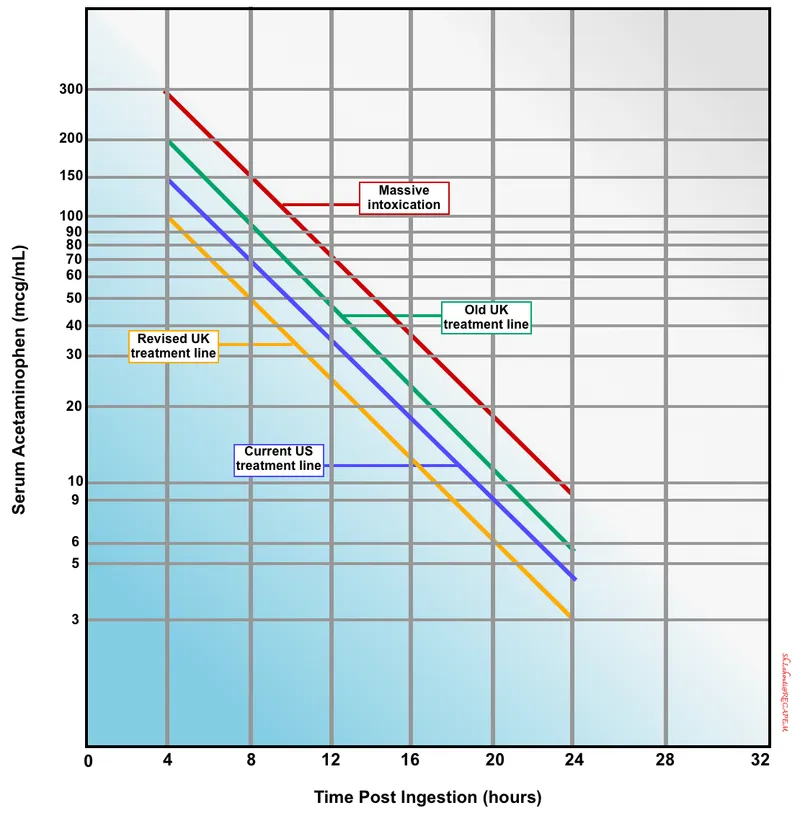
- Diagnosis: Rumack-Matthew nomogram (use ≥4h post-ingestion).
- Antidote: N-acetylcysteine (NAC).
- IV regimen: 150 mg/kg (1h), then 50 mg/kg (4h), then 100 mg/kg (16h).
- Best if given within 8-10h.
⭐ NAC is also used for contrast-induced nephropathy prevention.
Opioid Overdose
- Classic triad: Coma, respiratory depression, miosis (pinpoint pupils).
- ⚠️ Mydriasis: meperidine, hypoxia.
- Antidote: Naloxone.
- Dose: 0.4-2 mg IV/IM/SC; repeat. Max initial: 10 mg.
- Continuous IV infusion for long-acting opioids (e.g., methadone) due to naloxone's short half-life (30-90 min).
OPs & Heavy Metals - Chemical Chaos
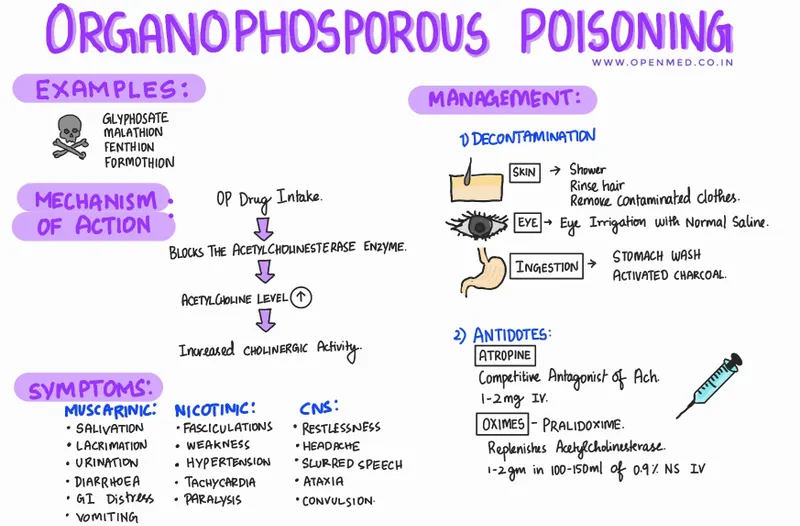
- Organophosphates (OPs): Irreversible AChE inhibitors.
- 📌 DUMBELS/SLUDGE (muscarinic); Muscle weakness, paralysis (nicotinic).
- Rx: Atropine (2-5 mg IV, titrate), Pralidoxime (PAM, 1-2 g IV for nicotinic signs, <48h).
- Heavy Metals: Chelation therapy is key.
- Lead (Pb): Paint, batteries. Colic, anemia, wrist drop. Chelation: BAL+EDTA (severe), Succimer (DMSA).
- Arsenic (As): Garlic breath, rice-water stools. Chelation: BAL, DMSA.
- Mercury (Hg): Neurotoxicity (organic), renal (inorganic). Chelation: DMSA, BAL (not methylHg).
- Iron (Fe): GI bleed, acidosis, liver damage. Rx: Deferoxamine IV (if severe, serum Fe >500 µg/dL). ⭐ > Deferoxamine causes "vin rosé" urine.
- Toxic Alcohols (Methanol, Ethylene Glycol): ↑AGMA, ↑Osmolal gap.
- Methanol → Formic acid (blindness). Ethylene Glycol → Oxalic acid (renal failure).
- Rx: Fomepizole (15 mg/kg LD) or Ethanol; Hemodialysis. Folate (Methanol), Thiamine/Pyridoxine (EG).
Toxidrome Spotting - The Poison Profiler
Recognizing toxidromes is key when the specific poison is unknown.
| Toxidrome | Vitals (HR,BP,RR,T) | Pupils | Skin | Bowel Sounds | Mental Status | Other Signs |
|---|---|---|---|---|---|---|
| Anticholinergic | ↑HR, ↑Temp; BP/RR variable | Mydriasis | Hot, Dry, Red | ↓ | Agitated, Delirium | Urinary retention, Myoclonus; "Mad as a hatter..." |
| Cholinergic | Bradycardia (musc) or Tachycardia (nic); RR/Temp variable | Miosis | Diaphoretic | ↑ | Confusion, Coma | 📌 SLUDGE-BAM; Bronchorrhea, Bronchospasm |
| Opioid | ↓HR, ↓BP, ↓RR, ↓Temp | Miosis | Cool, Clammy | ↓ | CNS Depression | Respiratory depression, Track marks |
| Sympathomimetic | ↑HR, ↑BP, ↑RR, ↑Temp | Mydriasis | Diaphoretic | ↑ | Agitated, Psychosis | Seizures, Tremors, Hyperreflexia |
| Sedative-Hypnotic | ↓HR, ↓BP, ↓RR, ↓Temp | Variable | Cool | ↓ | CNS Depression | Slurred speech, Ataxia, Nystagmus, Hyporeflexia |
High‑Yield Points - ⚡ Biggest Takeaways
- Key antidotes: N-acetylcysteine (paracetamol), naloxone (opioids), flumazenil (benzodiazepines), atropine/pralidoxime (organophosphates).
- Identify toxidromes (e.g., cholinergic, anticholinergic) for rapid diagnosis.
- Management: ABCDE, decontamination (activated charcoal), enhanced elimination.
- Paracetamol toxicity: Hepatotoxicity risk; use N-acetylcysteine per Rumack-Matthew nomogram.
- Organophosphates: Treat with atropine (muscarinic) and pralidoxime (cholinesterase regeneration).
- Salicylate poisoning: Mixed acid-base disturbance; alkaline diuresis is key.
- TCA overdose: Sodium bicarbonate for QRS prolongation (cardiotoxicity).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

