Opioid Basics & Receptors - Poppy's Keyholes
- Source: Opium poppy (Papaver somniferum) or synthetic.
- Endogenous Opioids (natural ligands):
- Enkephalins (bind μ, δ)
- Endorphins (bind μ)
- Dynorphins (bind κ)
- Receptors (GPCRs) 📌 "Poppy's Keyholes":
- μ (MOR): Supraspinal/spinal analgesia, euphoria, resp. depression, miosis, dependence.
- κ (KOR): Spinal analgesia, dysphoria, sedation, miosis.
- δ (DOR): Analgesia (spinal/supraspinal), antidepressant effects.
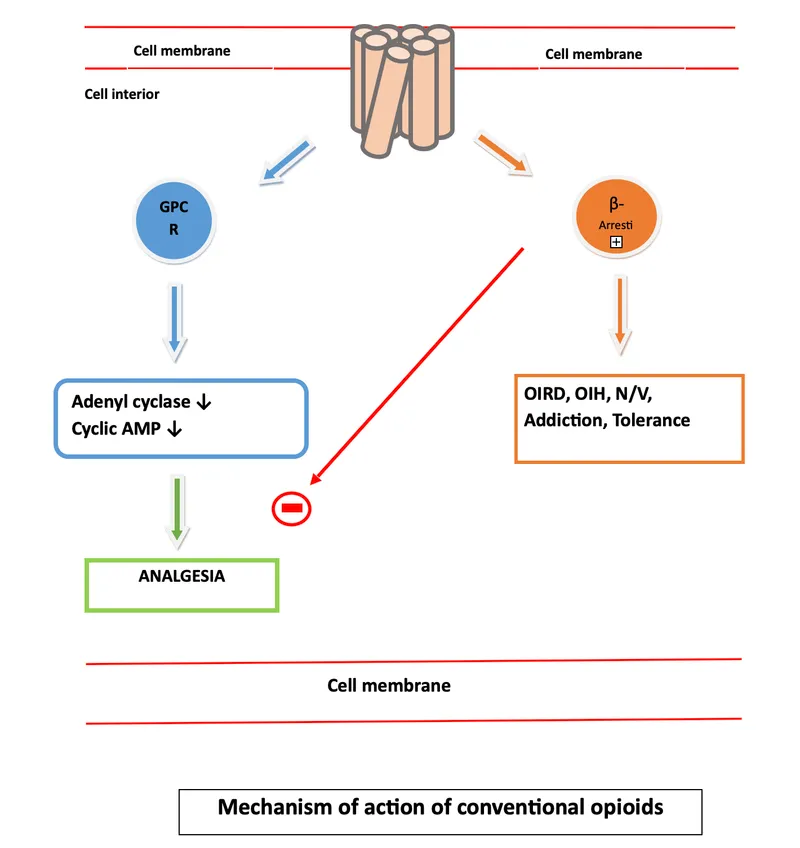
- Mechanism: All inhibit adenylyl cyclase (↓cAMP); Open K+ channels (hyperpolarize); Close Ca2+ channels (↓neurotransmitter release).
⭐ Mu (μ) receptors are key for analgesia and euphoria, but also mediate respiratory depression & dependence.
Opioid Actions & Uses - Pain Killers' Punch
- Analgesia: Modifies pain perception & response (moderate-severe acute/chronic pain).
- CNS Effects: Euphoria/dysphoria, sedation, potent respiratory depression ⚠️, antitussive, miosis (pinpoint pupils), nausea/vomiting.
- Peripheral Effects: Constipation (↓motility), biliary spasm, histamine release (morphine: hypotension, itching).
- Key Uses:
- Pain relief (post-op, cancer, MI).
- Anesthesia adjunct.
- Acute Pulmonary Edema (morphine).
- Severe diarrhea (loperamide).
⭐ Tolerance develops to most opioid effects (analgesia, euphoria, respiratory depression) but NOT to miosis or constipation.
Key Opioids - The Morphine Mob
- Morphine: Gold standard for severe pain. Active metabolite: Morphine-6-glucuronide (M6G).
- Key side effects: Respiratory depression, constipation, miosis, nausea.
- Codeine: Prodrug (CYP2D6 to morphine). Weak analgesic, good antitussive.
- Heroin (Diamorphine): Highly lipophilic, rapid CNS penetration. High abuse potential.
- Pethidine (Meperidine): Synthetic. Norpethidine (toxic metabolite) → seizures. Atropine-like effects. ⚠️ Avoid in renal failure, with MAOIs.
- Fentanyl & congeners (Sufentanil, Remifentanil): Highly potent (Fentanyl ~100x morphine). Rapid onset, short duration. Used in anaesthesia.
- Methadone: Long half-life. Used for opioid dependence (maintenance therapy) & chronic pain. ⚠️ QT prolongation.
⭐ Pethidine: Mydriasis (atropine-like effect), unlike typical opioid miosis.
Adverse Effects & Dependence - The Addiction Agony
- Common: Nausea, vomiting, constipation (📌 OIC), sedation, miosis (📌 PPupils), pruritus, urinary retention.
- Serious: Respiratory depression (dose-dependent, often fatal), hypotension, bradycardia, truncal rigidity (esp. fentanyl).
- Tolerance: Develops to analgesia, euphoria, sedation, respiratory depression. Mechanism: receptor changes, cAMP pathway upregulation.
- Minimal/no tolerance to miosis & constipation.
- Dependence (Physical): Withdrawal on cessation/antagonist (naloxone). Features autonomic hyperactivity (lacrimation, rhinorrhea, yawning, mydriasis, cramps, diarrhea, anxiety).
- Addiction (Psychological): Compulsive use; mesolimbic dopamine pathway.
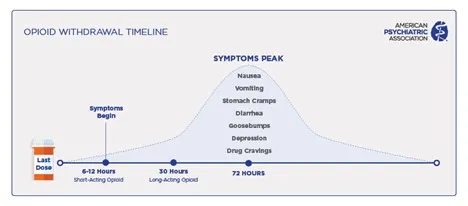
⭐ Miosis and constipation are opioid effects to which tolerance develops minimally or not at all.
Opioid Poisoning & Antagonists - Overdose Overturners
- Triad: Coma, respiratory depression (e.g., RR < 12/min, cyanosis), pinpoint pupils (miosis).
- Antidote: Naloxone. IV: 0.4-2mg q2-3min (max 10mg). Short t½ (1-2h).
- 📌 Naloxone Often Xits (short action), ONE dose may not be enough.
- Naltrexone: Oral, long-acting; for relapse prevention.
⭐ Naloxone's short half-life (~1 hour) often necessitates repeated doses or continuous infusion, especially with long-acting opioids like methadone.
High‑Yield Points - ⚡ Biggest Takeaways
- Opioids primarily act via μ-receptors (analgesia, respiratory depression, euphoria, miosis, constipation).
- Morphine is the prototype; naloxone is the antidote for overdose.
- Methadone is used for opioid dependence (long t½) and neuropathic pain.
- Fentanyl is highly potent; tramadol is an atypical opioid (SNRI activity).
- Pethidine may cause tachycardia and seizures (normeperidine).
- Pentazocine is a mixed agonist-antagonist, can precipitate withdrawal in dependent users.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

