Intro & MOA - Folate Foes
- Sulfonamides & Trimethoprim: Key synthetic antimicrobials. Bacteriostatic individually.
- MOA: Synergistic sequential blockade of bacterial folic acid synthesis. Humans utilize pre-formed dietary folate, ensuring selective toxicity.
- Sulfonamides (e.g., Sulfamethoxazole):
- PABA (para-aminobenzoic acid) structural analogues.
- Competitively inhibit bacterial Dihydropteroate Synthase.
- Prevent PABA $\rightarrow$ Dihydropteroic acid.
- Trimethoprim:
- Potent inhibitor of bacterial Dihydrofolate Reductase (DHFR).
- Prevents DHF (Dihydrofolic acid) $\rightarrow$ THF (Tetrahydrofolic acid - active form).
- Sulfonamides (e.g., Sulfamethoxazole):
- 📌 Mnemonic: Sulfa drugs Stop PABA at the Start; Trimethoprim Targets DHFR Downstream.
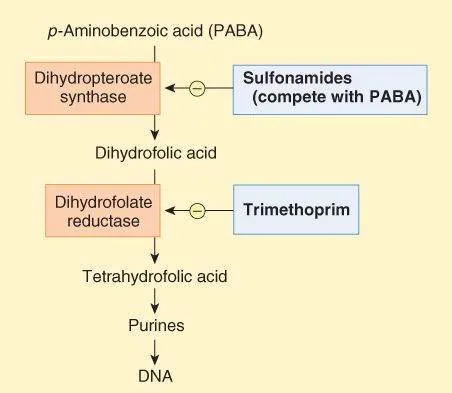
⭐ Co-trimoxazole (TMP-SMX combination) exhibits synergistic bactericidal activity due to this dual blockade, broadening spectrum and reducing resistance development.
Pharmacokinetics - Dynamic Duo's Journey
- Sulfonamides (e.g., Sulfamethoxazole - SMX):
- Absorption: Good orally.
- Distribution: Variable protein binding (↑drug interactions: bilirubin, warfarin); crosses placenta.
- Metabolism: Hepatic acetylation (📌 Slow acetylators ↑toxicity; metabolite → crystalluria).
- Excretion: Renal (filtration, secretion); adjust dose in renal failure.
- Trimethoprim (TMP):
- Absorption: Good orally.
- Distribution: Wide; excellent tissue penetration (CSF, prostate); lipophilic.
- Metabolism: Hepatic (minor).
- Excretion: Renal (mostly unchanged); adjust dose in renal failure.
- Co-trimoxazole (SMX + TMP):
- Pharmacokinetic match: Similar $T_{1/2}$ (~10-12h) allows combined dosing.
- Dosing SMX 5:TMP 1 → plasma conc. 20:1 for synergy.
⭐ Sulfonamides displace bilirubin from albumin → ↑risk of kernicterus in neonates.
Clinical Spectrum - Germ Warfare Gurus
Co-trimoxazole (TMP-SMX): A broad-spectrum agent. Key uses:
- Urinary Tract Infections (UTIs): Uncomplicated & complicated.
- Pneumocystis jirovecii Pneumonia (PJP):
- Treatment: Drug of Choice (DOC).
- Prophylaxis: Immunocompromised (e.g., HIV CD4 < 200/mm³).
- Nocardiosis: DOC.
- Toxoplasmosis: Alternative for cerebral toxo in AIDS.
- Listeriosis: Alternative, especially if penicillin-allergic.
- Others: Shigellosis, Salmonella (select cases), Stenotrophomonas maltophilia.
Other Sulfonamides/Related:
- Sulfasalazine: IBD (UC, Crohn's), Rheumatoid Arthritis.
- Silver sulfadiazine: Topical for burn infections.
- Sulfacetamide: Ophthalmic for bacterial conjunctivitis.
- Pyrimethamine-Sulfadoxine: Malaria (limited by resistance).
⭐ Co-trimoxazole is the Drug of Choice (DOC) for Pneumocystis jirovecii pneumonia (PJP) treatment/prophylaxis and Nocardiosis.
Adverse Effects & Cautions - The Watch-Out List
- Hypersensitivity: Rashes, fever, photosensitivity. Severe: Stevens-Johnson Syndrome (SJS), TEN.
- Crystalluria: (Sulfonamides) Prevent with hydration. Risk with older agents.
- Hematologic:
- Sulfonamides: Hemolytic anemia (G6PD deficiency), agranulocytosis.
- Trimethoprim: Megaloblastic anemia (folate deficiency), leukopenia.
- Kernicterus: (Sulfonamides) In newborns; bilirubin displacement from albumin.
⭐ Sulfonamides: Contraindicated in neonates (< 2 months) & late pregnancy due to kernicterus risk.
- Trimethoprim Specific: Hyperkalemia (monitor K+), GI upset.
- 📌 Mnemonic (SULFA ADRs): SJS, Skin, Solubility low (crystalluria), Serum albumin displacement, Anemia (G6PD).
- Contraindications:
- Infants < 2 months (Sulfonamides).
- Pregnancy (Sulfonamides near term; Trimethoprim 1st trimester).
- G6PD deficiency (Sulfonamides).
- Drug Interactions (↑ effect of): Warfarin, Methotrexate, Phenytoin. (Sulfonylureas with Sulfonamides).
High‑Yield Points - ⚡ Biggest Takeaways
- Sulfonamides (Dihydropteroate synthase inhibitor) & Trimethoprim (Dihydrofolate reductase inhibitor) cause sequential folate blockade.
- Co-trimoxazole (TMP-SMX) treats UTIs, PJP, Nocardiosis, Toxoplasmosis.
- Sulfonamide ADRs: Hypersensitivity, SJS, crystalluria, G6PD hemolysis, kernicterus.
- Trimethoprim ADRs: Megaloblastic anemia, leukopenia, hyperkalemia.
- Resistance: Altered enzymes, ↑PABA, ↓permeability.
- Contraindications: Newborns, late pregnancy (kernicterus); G6PD deficiency (sulfonamides).
- Key precaution: Hydration with sulfonamides to prevent crystalluria.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

