AMR Fundamentals - Resistance Rising
- Antimicrobial Resistance (AMR): Microbe's ability to survive/grow despite antimicrobial agent exposure, making infections harder to treat.
- Types of Resistance:
- Intrinsic (Natural): Innate characteristic of a microbe (e.g., Gram-negatives resistant to Vancomycin due to outer membrane).
- Acquired: Microbe develops resistance through genetic change (mutation) or horizontal gene transfer (HGT - conjugation, transduction, transformation).
- Impact: ↑ Treatment failure, prolonged illness, ↑ healthcare costs, ↑ mortality.

⭐ ESKAPE pathogens (Enterococcus faecium, Staphylococcus aureus, Klebsiella pneumoniae, Acinetobacter baumannii, Pseudomonas aeruginosa, and Enterobacter species) are critical due to high resistance rates and causing nosocomial infections. They effectively "escape" common antibiotics.
Resistance Mechanisms - Bacterial Armoury
Bacteria employ an arsenal of mechanisms to evade antimicrobial action, leading to resistance.
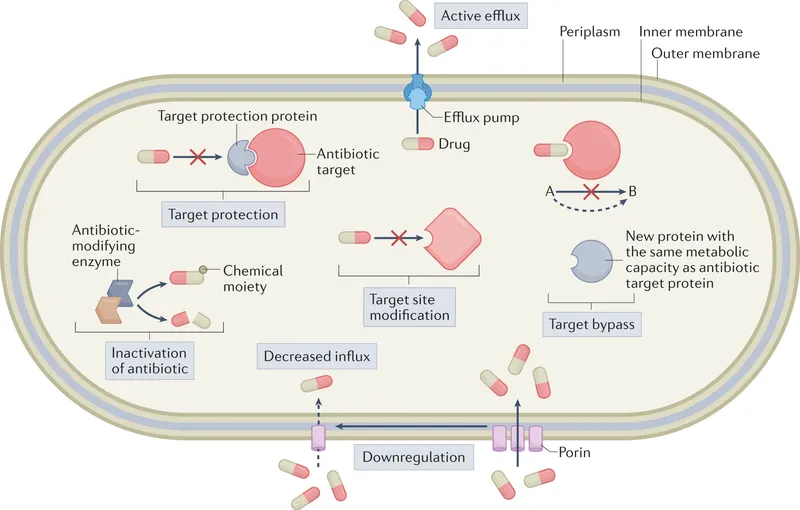
| Mechanism Type | Drugs Affected | Examples (Gene/Species) |
|---|---|---|
| 1. Enzymatic Inactivation | β-lactams, Aminoglycosides, Macrolides, Chloramphenicol | β-lactamases (bla), AAC, CAT (S. aureus, E. coli) |
| 2. Target Site Modification | Penicillins (PBPs), Macrolides (rRNA), FQs (Gyrase), Vancomycin (Peptide) | MRSA (mecA), VRE (vanA), erm genes |
| 3. ↓ Permeability / Porin Loss | β-lactams, Tetracyclines, FQs | P. aeruginosa (OprD loss) |
| 4. Efflux Pumps (MDR) | Tetracyclines, Macrolides, FQs, β-lactams | P. aeruginosa, E. coli (AcrAB-TolC) |
| 5. Target Protection | FQs (DNA gyrase), Tetracyclines (Ribosome) | Qnr proteins, Tet(O), Tet(M) |
| 6. Target Bypass/Overproduction | Sulfonamides (DHPS), Trimethoprim (DHFR) | ↑PABA (Sulfa), ↑DHFR (TMP) |
Gene Transfer - Superbug Shuffle
Rapid spread of antimicrobial resistance (AMR) genes, mainly by Horizontal Gene Transfer (HGT). 📌 CTT for HGT: Conjugation, Transduction, Transformation.
- HGT Mechanisms:
- Conjugation: "Bacterial sex"; plasmid (R-factor) transfer via pilus. Common in Gram (-).
- Transduction: Bacteriophage mediates DNA transfer.
- Transformation: Uptake of naked DNA by competent cells.
- Mobile Genetic Elements (MGEs): Vehicles for AMR genes.
- Plasmids: Extrachromosomal DNA; often carry multiple resistance genes (MDR).
- Transposons: "Jumping genes"; move within/between DNA.
- Integrons: Capture & express gene cassettes (arrays of AMR genes).
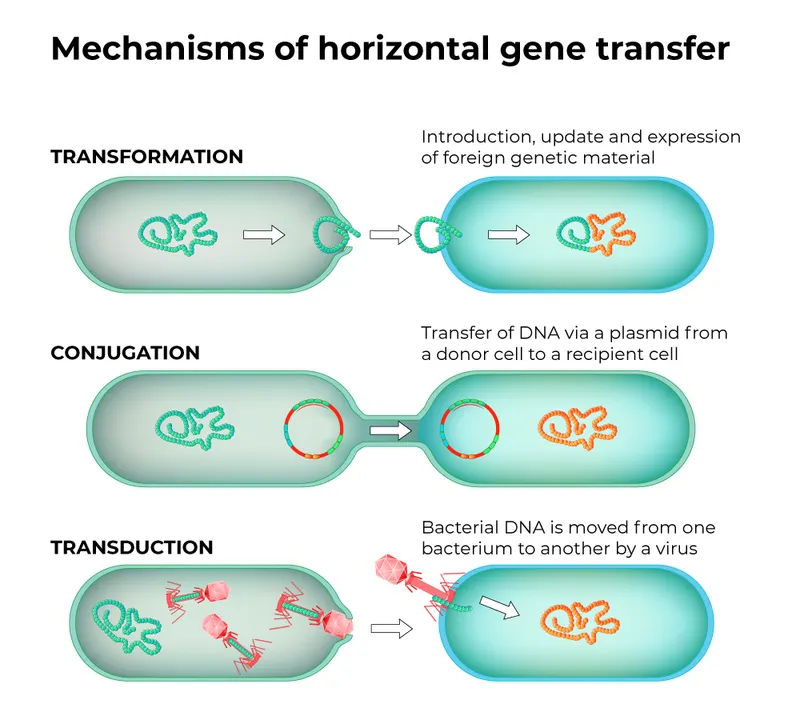
⭐ Plasmids often carry multiple resistance genes, conferring multi-drug resistance (MDR) in one transfer, rapidly creating "superbugs".
Key Culprits & Countermeasures - Villains & Vigilance
- Key Villains (Resistant Organisms):
- MRSA (Methicillin-Resistant S. aureus): Common in skin/soft tissue infections, pneumonia.
- VRE (Vancomycin-Resistant Enterococci): Cause UTIs, bacteremia, endocarditis.
- ESBLs (Extended-Spectrum β-Lactamase producers): e.g., E. coli, Klebsiella; resist most β-lactams (not carbapenems/cephamycins).
- CREs (Carbapenem-Resistant Enterobacteriaceae): e.g., KPC, NDM-1, OXA-48; "nightmare bacteria", high mortality.
- Vigilance (Countermeasures):
- Antimicrobial Stewardship (AMS): Optimize use, prevent resistance development.
- Infection Prevention & Control (IPC): Hand hygiene, isolation, active surveillance.
- New Drug Development & Novel Therapies: e.g., phage therapy, new antibiotics.
- Rapid Diagnostics: Quick identification of pathogens & resistance patterns.
⭐ NDM-1 (New Delhi Metallo-beta-lactamase-1) confers broad β-lactam resistance (incl. carbapenems); plasmid-mediated spread is a major concern in India.
High‑Yield Points - ⚡ Biggest Takeaways
- Intrinsic resistance is inherent; acquired resistance via mutation or horizontal gene transfer (e.g., plasmids).
- ESBLs resist most penicillins & cephalosporins; treat with carbapenems or beta-lactamase inhibitor combinations.
- MRSA (mecA gene, altered PBP2a) treated with vancomycin, linezolid, daptomycin.
- VRE (VanA/VanB genes) treated with linezolid, daptomycin.
- Carbapenemases (KPC, NDM-1) hydrolyze carbapenems, severely limiting options.
- Efflux pumps and target site modification are major mechanisms of multi-drug resistance (MDR).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

