DMARDs Overview - RheumaRiders Kickoff
- DMARDs: Disease-Modifying Antirheumatic Drugs; aim to alter the underlying rheumatic disease process.
- Goals of Therapy:
- Achieve remission or low disease activity.
- Prevent structural joint damage & long-term disability.
- Improve Quality of Life (QoL).
- General Principles:
- Early diagnosis and prompt initiation.
- Treat-to-target strategy.
- Regular monitoring for efficacy and adverse effects.
- Broad Classification:
- csDMARDs (Conventional Synthetic)
- bDMARDs (Biologic: original & biosimilars)
- tsDMARDs (Targeted Synthetic)

⭐ Methotrexate is the cornerstone DMARD for most Rheumatoid Arthritis patients, often initiated first-line unless contraindicated.
csDMARDs - Old Guard Allies
- Methotrexate (MTX): 📌 'Mother Of All DMARDs'
- MoA: Inhibits DHFR, AICAR transformylase → ↑adenosine.
- Dose: Weekly.
- Supplement: Folic acid (reduces ADRs).
- ADRs: Oral ulcers, hepatotoxicity, myelosuppression, pneumonitis.
- Contra: Pregnancy, liver disease.
- Leflunomide:
- MoA: Inhibits dihydroorotate dehydrogenase → ↓pyrimidine synthesis.
- ADRs: Hepatotoxicity, teratogenicity, diarrhea.
- Elimination: Cholestyramine wash-out.
- Sulfasalazine (SSZ):
- MoA: Prodrug → 5-ASA (anti-inflammatory) + sulfapyridine (antibacterial/immunomodulatory).
- ADRs: GI upset, rash, oligospermia (reversible), yellow-orange skin/urine.
- Hydroxychloroquine (HCQ):
- MoA: ↑lysosomal pH, ↓TLR signaling.
- ADRs: Retinal toxicity ('bull's eye maculopathy'), GI upset, skin pigmentation.
- Monitor: Regular ophthalmologic exam.
⭐ MTX is the anchor drug for rheumatoid arthritis and is often the first csDMARD prescribed.
Table: Comparative Overview of csDMARDs
| Feature | Methotrexate | Leflunomide | Sulfasalazine | Hydroxychloroquine |
|---|---|---|---|---|
| MoA | DHFR inhibitor, ↑adenosine | Dihydroorotate dehydrogenase inhibitor | Prodrug (5-ASA + sulfapyridine) | ↑lysosomal pH, ↓TLR signaling |
| Key ADRs | Myelosuppression, hepatotoxicity, oral ulcers | Hepatotoxicity, teratogenicity, diarrhea | GI upset, rash, oligospermia | Retinal toxicity, GI upset |
| Monitoring | CBC, LFTs, renal function | LFTs, BP | CBC, LFTs | Ophthalmologic exam |
| Pregnancy | Category X | Category X | Category B (folate needed) | Generally considered safe (Cat C debated) |
bDMARDs - BioLogic Blockers
- Anti-TNF-α Agents: Infliximab (chimeric mAb), Etanercept (fusion protein), Adalimumab (human mAb), Golimumab (human mAb), Certolizumab pegol (pegylated Fab' fragment).
- MoA: Neutralize TNF-α.
- ADRs: Injection site/infusion reactions, ↑risk of infections (esp. TB reactivation, fungal), demyelination, worsening HF, drug-induced lupus.
- Screening: TB, HBV, HCV.
⭐ Pre-treatment screening for TB (latent & active), HBV, and HCV is crucial before starting anti-TNF-α therapy due to risk of reactivation.
- Rituximab (Anti-CD20 mAb):
- MoA: Depletes B-cells.
- Uses: RA refractory to anti-TNF agents.
- ADRs: Infusion reactions, PML, HBV reactivation.
- Abatacept (CTLA4-Ig):
- MoA: T-cell co-stimulation modulator.
- ADRs: ↑infections; ⚠️ avoid with TNF-α inhibitors.
- Tocilizumab/Sarilumab (Anti-IL-6R mAb):
- MoA: Block IL-6 receptor.
- ADRs: ↑infections, dyslipidemia, ↑LFTs, neutropenia, GI perforation.
- Anakinra (IL-1 receptor antagonist):
- Less commonly used in RA.

tsDMARDs & Combos - Tiny Targets, Team Tactics
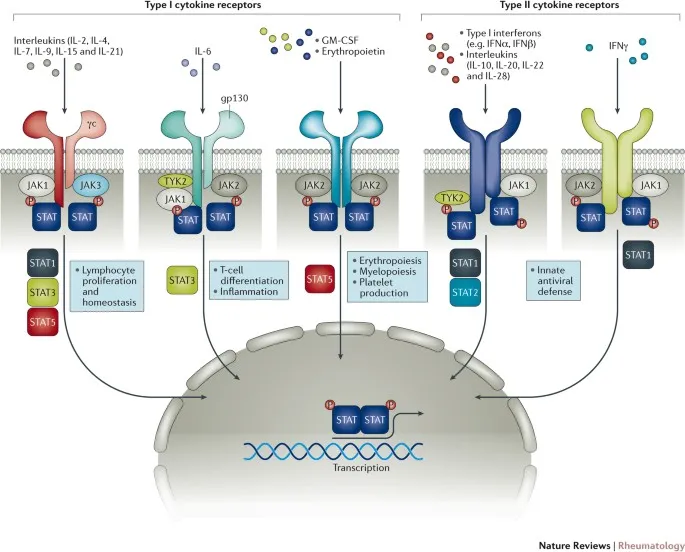
- JAK Inhibitors (tsDMARDs)
- Oral: Tofacitinib, Baricitinib, Upadacitinib.
- MoA: Inhibit Janus kinases (JAKs) → ↓cytokine signaling.
- ADRs: ⚠️ ↑Serious infections (Herpes Zoster, TB), hyperlipidemia, cytopenias, ↑thrombosis, malignancy. FDA Boxed Warnings.
- Monitoring: Lipids, CBC, LFTs (baseline & periodic).
- Combination DMARDs
- Strategy: MTX + bDMARD or MTX + other csDMARDs.
- ⚠️ Avoid combining two bDMARDs (↑immunosuppression).
- General DMARD Monitoring
- Baseline: CBC, LFTs, renal fx, ESR/CRP, viral (HBV/HCV/TB) screen.
- Periodic: For efficacy & toxicity.
- DMARDs in Special Populations
- Pregnancy:
- Safer: HCQ, SSZ.
- Contraindicated: MTX, Leflunomide.
- Breastfeeding:
- Generally compatible: HCQ, SSZ.
- Avoid: MTX, Leflunomide.
- Pregnancy:
⭐ Tofacitinib (a JAK inhibitor) carries FDA Boxed Warnings for serious infections, MACE, malignancy, and thrombosis.
High‑Yield Points - ⚡ Biggest Takeaways
- Methotrexate (MTX): first-line DMARD for RA; folic acid supplementation is crucial.
- Leflunomide: inhibits dihydroorotate dehydrogenase; an alternative to MTX.
- Hydroxychloroquine (HCQ): monitor for retinal toxicity (bull's eye maculopathy).
- Sulfasalazine: used in RA and IBD; side effects include hemolysis in G6PD deficiency.
- TNF-α inhibitors (e.g., Infliximab, Adalimumab): screen for latent TB before starting.
- Tofacitinib: an oral JAK inhibitor, for RA refractory to other DMARDs_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

