Introduction & Definition - Tiny Lungs, Big Trouble
- Chronic Lung Disease (CLD) / Bronchopulmonary Dysplasia (BPD): Impaired lung development in preterm infants, leading to long-term respiratory problems.
- Key risk factors: Prematurity (especially <32 weeks gestation), prolonged oxygen therapy, and mechanical ventilation.
- Diagnostic criteria (NIH consensus):
- Oxygen requirement for ≥28 days PLUS
- Assessment of respiratory support needed at 36 weeks Postmenstrual Age (PMA) for infants born <32 weeks GA, OR at 56 days postnatal age (or discharge) for infants born ≥32 weeks GA.
⭐ BPD is defined by the need for supplemental oxygen for at least 28 days, with severity assessed at 36 weeks PMA for infants born <32 weeks gestation (or equivalent for older preterms).
Pathophysiology - The Perfect Storm
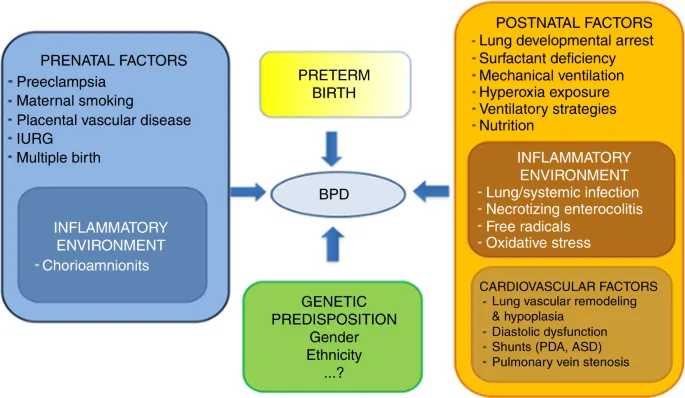
A vulnerable premature lung, often at the saccular stage of development with inherent surfactant deficiency and fewer antioxidants, encounters multiple postnatal insults. This "perfect storm" disrupts normal lung maturation. Key factors include:
- Oxygen Toxicity: Prolonged hyperoxia (↑FiO2) generates Reactive Oxygen Species (ROS), overwhelming antioxidant defenses and causing cellular damage.
- Ventilator-Induced Lung Injury (VILI): Mechanical ventilation (baro/volutrauma) incites an inflammatory cascade.
- Inflammation: Prenatal (e.g., chorioamnionitis) or postnatal infections trigger and sustain damaging inflammation.
- Impaired Repair & Remodeling: Disrupted healing processes lead to characteristic alveolar simplification (fewer, larger alveoli) and dysmorphic pulmonary vasculature, hallmarks of "new" BPD.

⭐ "New" BPD is characterized more by arrested lung development (alveolar simplification & dysregulated angiogenesis) than the severe airway injury and fibrosis of "old" BPD.
Risk Factors & Prevention - Dodging the Danger
- Key Risk Factors:
- Extreme prematurity (< 28 wks), very LBW (< 1000g)
- RDS, prolonged mechanical ventilation (baro/volutrauma)
- Oxygen toxicity (prolonged high $F_iO_2$)
- Sepsis, chorioamnionitis, PDA
- Prevention Strategies:
- Antenatal corticosteroids (e.g., Betamethasone)
- Exogenous surfactant for RDS
- Gentle ventilation: NIV (CPAP), low tidal volumes (4-6 mL/kg), optimal PEEP
- Judicious O₂: Target SpO₂ 90-95%
- Caffeine for apnea, Vitamin A supplementation
- Strict infection control, nutritional support
⭐ Antenatal corticosteroids significantly reduce RDS incidence, a major BPD precursor.
Clinical Features & Management - Breathing Battles
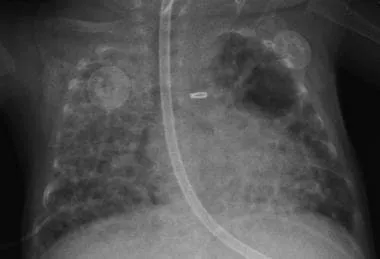
- Clinical Presentation:
- Persistent $O_2$ need > 28 days or > 36 wks PMA.
- Tachypnea, retractions, wheeze, crackles.
- Poor growth, $CO_2$ retention.
- Signs of pulmonary hypertension (PHT).
- Management Strategy:
- Respiratory Support:
- Oxygen (Target $SpO_2$ 90-95%).
- CPAP/NIPPV; gentle ventilation.
- Pharmacotherapy:
- Diuretics (e.g., Furosemide, Thiazides).
- Bronchodilators (trial if reactive airways).
- Caffeine (apnea, extubation).
- Postnatal steroids (low dose, short course for severe cases).
- Vitamin A.
- Nutrition: High calorie (120-150 kcal/kg/d), careful fluid balance.
- Prophylaxis & Monitoring:
- Palivizumab (RSV).
- Monitor for PHT, GERD, neurodevelopment.
- Respiratory Support:
⭐ BPD severity (Mild, Moderate, Severe) is defined by oxygen requirement at 36 weeks PMA or discharge (whichever is first).
Complications & Prognosis - The Long Haul
- Respiratory: Persistent wheeze, cough; ↑ susceptibility to infections (e.g., RSV); asthma-like symptoms; Pulmonary Hypertension (PHTN).
- Neurodevelopmental: High risk of developmental delay, cerebral palsy, learning difficulties.
- Growth: Failure to thrive, poor somatic growth.
- Cardiovascular: Systemic hypertension.
- Prognosis: Severity-dependent. Lung function abnormalities may persist into adulthood.
⭐ Pulmonary hypertension is a significant cause of mortality in severe BPD.
- Mortality highest in first 2 years; neurodevelopmental outcomes are a major long-term concern.
High‑Yield Points - ⚡ Biggest Takeaways
- BPD Definition: Oxygen dependency at 36 weeks Postmenstrual Age (PMA) or for ≥28 days after birth.
- Primary Risk Factors: Extreme prematurity, prolonged mechanical ventilation, and oxygen toxicity.
- Pathophysiology: Characterized by arrested alveolar and pulmonary vascular development.
- Prevention Strategies: Antenatal corticosteroids, caffeine therapy, and gentle ventilation techniques.
- Key Management: Includes oxygen supplementation, diuretics, bronchodilators, and nutritional support.
- Significant Complications: Pulmonary hypertension, neurodevelopmental impairment, and recurrent respiratory infections.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

