Indications & Goals - Breathless Kiddos SOS
- Indications (Why ventilate?):
- Respiratory Failure:
- Hypoxemic: e.g., ARDS, pneumonia ($PaO_2/FiO_2 < \textbf{200}$)
- Hypercapnic: e.g., severe asthma, NMD ($PaCO_2 > \textbf{55}$ mmHg, pH < 7.25)
- Airway Protection: GCS < 8, risk of aspiration
- Apnea: Central or prolonged obstructive
- ↑ Work of Breathing: Impending fatigue, respiratory muscle exhaustion
- Cardiopulmonary Arrest
- Respiratory Failure:
- Goals (What to achieve?):
- Improve Gas Exchange: Target $SpO_2 > \textbf{92}%$, acceptable $PaCO_2$
- ↓ Work of Breathing: Patient comfort, prevent muscle fatigue
- Lung Protection: Minimize Ventilator-Induced Lung Injury (VILI)
- Supportive Care: Allow recovery from underlying pathology
⭐ In children, respiratory distress progressing to failure is a more common pathway to cardiac arrest than primary cardiac events.

Initiation & Modes - Tiny Lungs, Big Help
- Initiation:
- Secure airway: ETT $(Age/4)+4$ uncuffed, $(Age/4)+3.5$ cuffed. Confirm.
- Initial Vt: 4-8 mL/kg (IBW).
- PEEP: 3-5 cm H₂O.
- FiO₂: Start 100%, titrate for SpO₂ >92%.
- RR & Ti: Age-dependent.
- Common Modes:
- VC: Set Vt.
- PC: Set PIP; Vt varies. Good for stiff lungs.
- PSV: Spontaneous breaths; for weaning.
- HFOV: Severe ARDS.
⭐ Lung Protective Strategy (LPS): Low Vt (4-6 mL/kg PBW), Pplat <28-30 cm H₂O.
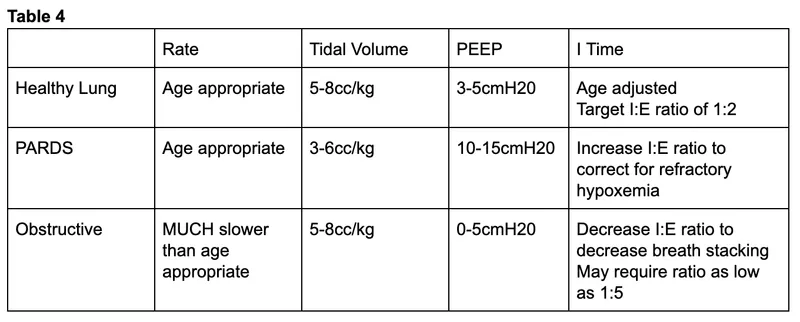
Key Parameters & Settings - Numbers Game For Lungs

- Tidal Volume (Vt): 6-8 mL/kg (ideal body weight); ARDS: 4-6 mL/kg.
- PEEP: Initial 5 cm H₂O; titrate for oxygenation & hemodynamics.
- Respiratory Rate (RR): Age-specific:
- Infant: 25-40/min
- Child: 20-30/min
- Adolescent: 12-20/min
- Inspiratory Time (Ti): Infants 0.3-0.7s; Children 0.5-1.0s. I:E ratio 1:2 - 1:3.
- FiO₂: Start 100% if hypoxic; titrate to maintain SpO₂ >92-94%.
- Pressures:
- Peak Inspiratory Pressure (PIP): Keep <30-35 cm H₂O (ARDS <28).
- Plateau Pressure (Pplat): Keep <28-30 cm H₂O (ARDS <25).
- Driving Pressure ($P_{driving}$ = Pplat - PEEP): Target <15 cm H₂O.
⭐ Driving pressure ($P_{driving}$ = Pplat - PEEP) <15 cm H₂O is associated with improved survival in ARDS patients, including children.
Monitoring & Weaning - Freedom Breath Quest
- Monitoring: Clinical (RR, WOB, effort), $SpO_2$ (>92%), ABG ($PaCO_2$ 35-45 mmHg), EtCO2, ventilator waveforms & mechanics.
- Weaning Readiness (📌 ROAM criteria):
- Resolution/Improvement of illness.
- Oxygenation: $PaO_2/FiO_2 > \textbf{150-200}$, PEEP $\le \textbf{5-8}$ cm H2O, $FiO_2 \le \textbf{0.4}$.
- Awake, alert, adequate cough.
- Minimal sedation/vasopressors.
- SBT: Low PSV (5-7 cm H2O)/CPAP (5 cm H2O) for 30 min-2 hrs. Success if stable vitals, no distress. Then extubate.
⭐ Successful Spontaneous Breathing Trial (SBT) is the most reliable indicator for extubation readiness.
Complications & Special Cases - Tricky Breaths
- Barotrauma/Volutrauma: Pneumothorax, PIE. Prevent with low $V_T$, $P_{plat}$ <30 cmH2O.
- VAP: ↑ Risk with duration. Prevention bundles.
- Oxygen Toxicity: Use lowest FiO2 for $SpO_2$ >92%.
- Auto-PEEP: Esp. in asthma. ↑ $T_E$, ↓ RR.
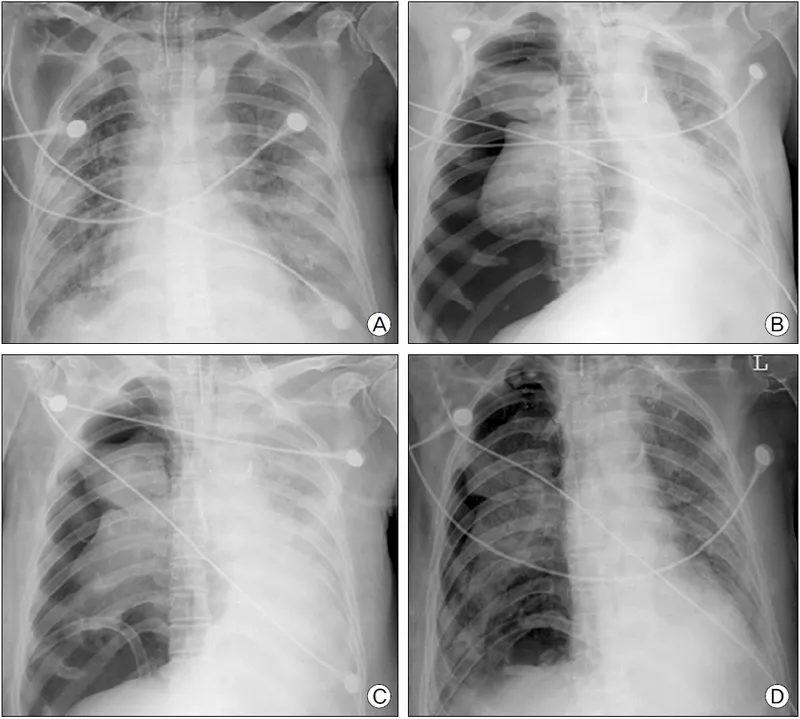
- ARDS: LPS: $V_T$ 4-6 mL/kg PBW, PEEP guided by $SpO_2$/FiO2.
⭐ In pediatric ARDS, target $P_{plat}$ ≤28-30 cmH2O; higher PEEP may be needed.
- Asthma: Permissive hypercapnia, avoid breath stacking.
 oka
oka
High‑Yield Points - ⚡ Biggest Takeaways
- Target tidal volume (Vt) is 6-8 mL/kg of ideal body weight (IBW).
- Initial PEEP is typically 5 cm H2O; titrate for oxygenation and hemodynamics.
- Employ lung protective strategies: low Vt, appropriate PEEP, and limit plateau pressure (Pplat) <28-30 cm H2O.
- Permissive hypercapnia (PaCO2 ↑) is acceptable in ARDS if pH remains >7.20-7.25.
- Cuffed endotracheal tubes are increasingly preferred for precise ventilation and aspiration prevention.
- Key complications include Ventilator-Associated Pneumonia (VAP), barotrauma, and volutrauma.
- Spontaneous Breathing Trials (SBTs) are crucial for assessing readiness for extubation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

